Does Rheumatoid Arthritis Cause Rashes
RA dorashRAcauserashRashesRARA rashes
Rheumatoid patients can develop skin disorders. UIHC notes that the same kind of immune system problems that cause joint inflammation, swelling, and pain can also affect your skin. When this happens, RA patients may develop lesions or rashes on the skin, reflecting immunological dysfunctions.
Secondly, how long does RA rash last? These are usually mild and clear up in a few days. More worrisome are overall rashes or hives that appear during or within 24 hours after you receive infusion of a drug directly into your bloodstream.
Similarly, what type of arthritis causes a rash?
Psoriatic arthritis is a form of arthritis that typically occurs in people with psoriasis. In addition to pain, stiffness, and swelling of the joints, psoriatic arthritis can cause a red, scaly rash. In this article, we discuss whether psoriatic arthritis always causes a rash.
Is there a link between eczema and arthritis?
And eczema, psoriasis, skin infections and rosacea have also been associated with RA. Why and how RA and these skin diseases are related is a subject of research. One study found that drugs that block tumor necrosis factor one of the inflammatory proteins that are elevated in people with RA may play a role.
Reactive Arthritis Skin Rash
Skin problems. Reactive arthritis can affect your skin a variety of ways, including a rash on your soles and palms and mouth sores. Low back pain. The pain tends to be worse at night or in the morning. When to see a doctor. If you develop joint pain within a month of having diarrhea or a genital infection, contact your doctor.
Diagnosing Rheumatoid Arthritis Rash
If you experience an RA rash, you should call your rheumatologist right away, as it could be a reaction to one of your . Your doctor can do a number of tests to figure out what is going on, and can also examine the skin and adjust your RA medication, if needed.
Your care specialist may do any of the following to find out the ultimate cause of your rash:
Also Check: Dog Hives All Over Body
Chronic Autoimmune Illnesses Linked To Chronic Hives
Chronic hives can be a formidable foe, especially when its not clear whats causing the itchy, red welts or wheals that can appear anywhere on the body and recur for six weeks or more. Sometimes a hidden illness may be an underlying cause. Studies have found a strong association between chronic hives and autoimmune diseases such as thyroid disease, rheumatoid arthritis, celiac disease, type 1 diabetes, Sjögren syndrome, and lupus.
Rashes In The Early Stages Ra
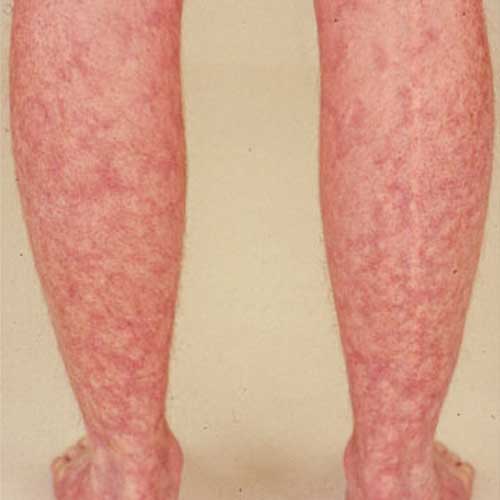
While not common, skin rashes may appear along with the first signs and symptoms of rheumatoid arthritis.10Alves F, Gonçalo M. Suspected inflammatory rheumatic diseases in patients presenting with skin rashes.& nbsp Best Pract Res Clin Rheumatol. 2019 33:101440. doi:10.1016/j.berh.2019.101440 PMID:& nbsp 31585842 The diagnosing physician will need to rule out other autoimmune conditions, such as lupus and psoriatic arthritis, that are more likely to cause skin abnormalities.
Recommended Reading: Where Does Hiv Rash Appear
What Causes A Rash In Rheumatoid Arthritis
Eczema, Sweet’s syndrome, and pyoderma gangrenosum are all related to autoimmune problems. Both Sweets syndrome and pyoderma gangrenosum are neutrophilic dermatoses, inflammatory skin conditions related to an overload of a type of white blood cell called neutrophils. Neutrophils naturally produce an inflammatory response to infection. In an autoimmune condition, the skin may be attacked as foreign by the immune system, leading to neutrophils overwhelming the skin and causing inflammation as if the skin was infected.
While the precise cause of eczema is not known, it is generally considered to be an autoimmune response that causes inflammation of the skin. Other autoimmune conditions besides RA have been associated with eczema, including Crohns disease and ulcerative colitis.
Rheumatoid vasculitis is caused by inflammation of both small- and medium-sized blood vessels, often as part of an RA flare-up. It usually occurs in people who have had severe RA for more than 10 years. Certain factors play a part in those who are at higher risk for this complication. Most people who develop rheumatoid vasculitis have a high rheumatoid factor in their blood and many smoke cigarettes.
Palmar erythema, reddening in the palms, has a wide variety of causes. When someone with RA experiences red palms, however, it is most likely to be as a result of an autoimmune response. It can also be caused by medication taken to treat RA.
What Does Rheumatoid Vasculitis Look Like
Rheumatoid vasculitis is hard to miss.
“Visually, I can recognize it right away,” said Dr. Koval. “It’s an impressive rash with a sudden onset and can be scary looking.”
According to the Vasculitis Foundation, rheumatoid vasculitis can appear as any of the following:
- Small pits on the fingertips
- Painful, red rash
Don’t Miss: Where Did Hiv Aids Begin
Treatment For Psoriatic Arthritis
Some people with psoriatic arthritis have mild symptoms. They may be able to control pain and swelling with over-the-counter anti-inflammatory drugs.
People with advanced disease usually need prescription medications. These drugs can relieve symptoms and prevent permanent joint damage. They include:
- Nonsteroidal anti-inflammatory medications to reduce pain and swelling.
- Cortisone injections and oral steroids to quickly reduce inflammation in the short term.
- Disease-modifying antirheumatic drugs , which protect joints by blocking inflammation.
- Biologics, a special class of DMARDs that target the specific parts of your immune system that drive inflammation.
Besides medications, there are things you can do to help relieve pain and protect your joints:
- Maintain a healthy weight.
- Use splints to stabilize inflamed joints.
- Use hot packs and ice packs to ease pain and swelling.
- Engage in gentle exercises like walking, swimming and tai chi.
- Consider surgery. Most people with psoriatic arthritis dont need surgery. But if you have severely damaged joints, joint replacement surgery can restore function.
Theres no cure for psoriasis or psoriatic arthritis, but you can manage both with treatment. And new medications come out every year, says Dr. Parody. By working with your doctor, you can develop a plan to protect your joints and keep doing the things you love.
How Are These Autoimmune Diseases Diagnosed
Because conditions such as lupus and scleroderma have symptoms that can resemble many other diseases, they can be difficult to diagnose initially. Lupus, for instance, can have symptoms that include fatigue and fever. Symptoms of scleroderma can include heartburn.
When you notice the first symptomsgenerally some form of skin rash that doesnt go away or that worsens over timeyou may seek treatment from a primary care doctor or dermatologist. An examination with a doctor can include discussion of symptoms, personal medical history and family history, as well as blood and other laboratory tests . The patient may then consult with a rheumatologist, who will have more experience working with the internal symptoms of the disease. Over time and depending on his or her symptoms, a patient may work with either a dermatologist or a rheumatologist, or both.
You May Like: What Can You Take For Arthritis In Your Fingers
Don’t Miss: Can I Get An Hiv Test At Walgreens
Psoriasis And Psoriatic Arthritis
and are autoimmune diseases that can cause skin rashes, and can present on the skin in the form of plaques, pustules, lesions and blisters, according to Creaky Joints. And a 2021 study published in the Journal of the American Academy of Dermatology found that adults with psoriasis had an increased likelihood of having rheumatoid arthritis compared to adults who didnt have psoriasis.
What Is A Juvenile Rheumatoid Arthritis Rash
Juvenile rheumatoid arthritis is part of a wider systemic condition known as juvenile idiopathic arthritis . This general term of arthritic conditions affects children before the age of 16 with symptoms that last for 6 weeks or longer.
One of the key symptoms can be a rash that may look pink or purple. It typically affects the trunk, arms, and legs, but not the face. It usually occurs alongside a fever.
Recommended Reading: What Causes False Positive Hiv Test
An Adverse Reaction To Exercise And Environment
Although a daily dose of thirty minutes of exercise is highly recommended, it may also be causing an individual to break out in hives. The body produces a chemical that can inhibit cell breakdown as cause rashes, known as acetylcholine, during exercise as a natural bodily response. Sweating is also known to cause a breakout of hives in those who are already prone to the condition. The sweat itself is not causing the hives, but the excess warmth of the skin can irritate the area concerned. Managing the inhabited environment, exercise, and what is consumed is paramount if hives are affecting an individual on a regular basis. There are also many environmental occurrences that can cause hives to break out such as excess heat, powerful winds, bug bites, and some plants are known to cause a breakout. If environmental concerns are worrisome, talk to a health professional about taking an antihistamine to reduce skin irritability.
Are Rashes From Rheumatoid Arthritis And Eczema Connected
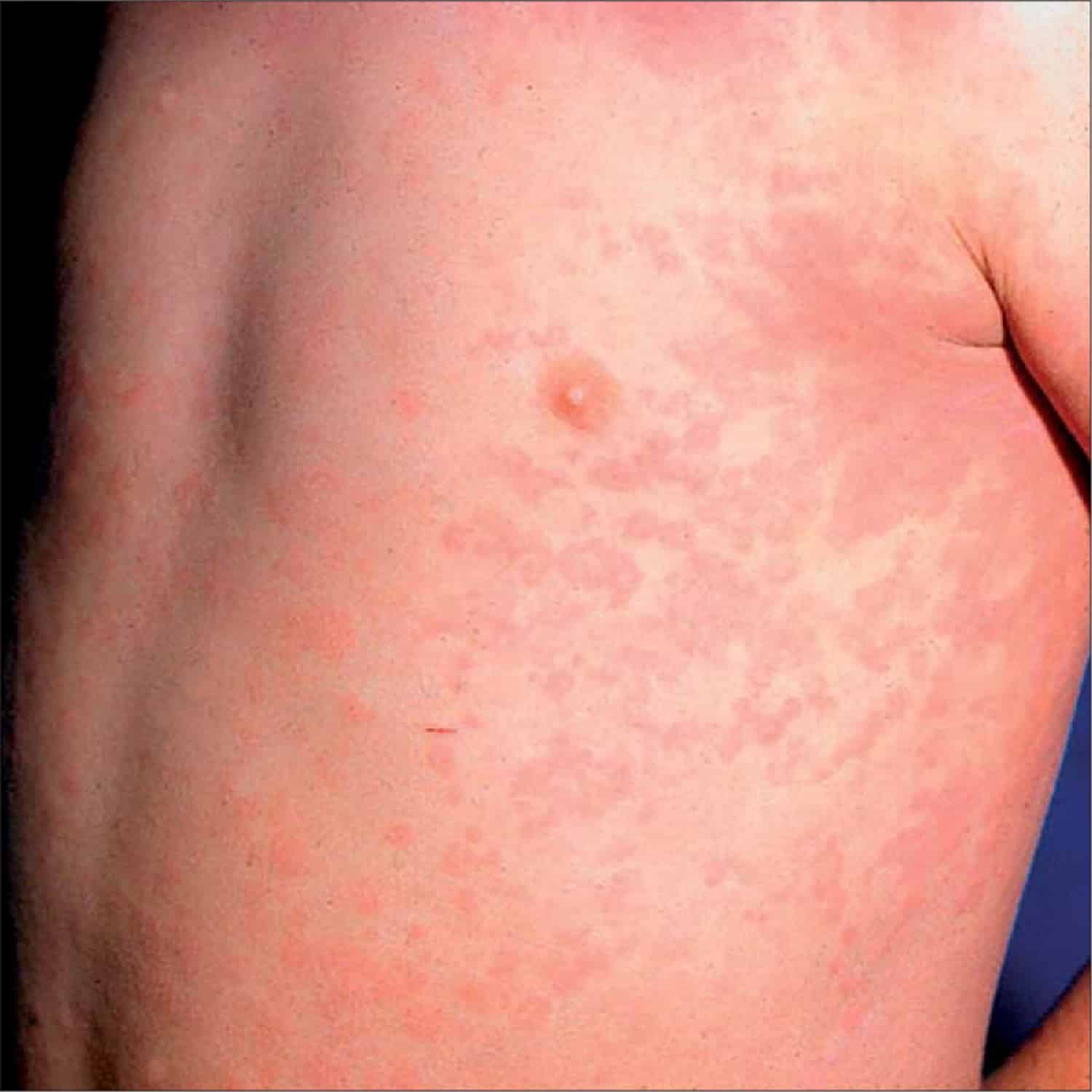
Any person that is suffering from rheumatoid arthritis is dealing with a health condition where the body attacks its own joints instead of fighting off bacteria and viruses like its supposed to. The result of the autoimmune disease is painful wrists, feet, ankles, and fingers.
However, that isnt necessarily the only problem that surfaces. For some, because of the swelling of the joints, eczema can also be a symptom.
The skin above where the inflammation of the joints is occurring can become inflamed as well. It will get rough, itchy, bleed, and in severe cases, blisters may even form. More often than not, these two conditions appear separately.
Eczema is a skin condition that first appears in early childhood years for most patients and continues on throughout their lives. Sometimes though, an individual can get eczema as a result of their arthritis.
While there is still more research that needs to be done on the connection between arthritis and eczema, experts suggest that the red, itchy, and bumpy skin frequently shows up as an indicator that something related to the restriction in blood flow is happening beneath the surface.
Read Also: Best Thing For Arthritic Knees
Read Also: How Do Hiv Drugs Work
How To Spot Juvenile Arthritis In Your Child
What comes to mind when you think of arthritis? More often than not, you may picture an elderly person hobbling around, dealing with the daily struggles of joint inflammation with each painful step.
But arthritis affects children, too. At any point before your child matures into an adult, his or her body may experience a chronic inflammatory response that causes joint pain, skin rashes or more complex internal organ issues.
These symptoms are treatable, as well outline below, but youll first need to recognize if your child has juvenile arthritis. The quicker you obtain a diagnosis, the more proactive doctors can be with treatments that can allow your child to live a long, healthy life. With July serving as Juvenile Arthritis Awareness Month, we put together a comprehensive guide outlining how to spot these diseases, the types of arthritis in children, and ways to keep symptoms under control.
Articular Features Of Rheumatoid Arthritis
Rheumatoid arthritis initially affects the small joints, such as those in the hands, but in later stages can affect any joint. It presents as episodic flares of symmetrical synovitis , morning stiffness, and enthesitis. Untreated, it progresses to irreversible joint destruction with loss of cartilage and bone.
Recommended Reading: Rheumatoid Arthritis Edema
Recommended Reading: Can You Catch Hiv Twice
Living With Rheumatoid Arthritis Rash
The addition of a skin rash while dealing with other symptoms of rheumatoid arthritis is not easy, but rest assured, theres hope. If you struggle with RA skin rashes or related symptoms, reach out to your rheumatologist, who can help you determine the cause and work on an effective treatment. Your physician can also connect you with other specialists so you can feel better and live your best lifehopefully, rash-free.
Can Rheumatoid Arthritis Cause Skin Eruptions
Rheumatoid arthritis is an autoimmune disorder with dermatology problems.
Your immune system attack itself by attacking the joints.
The active immunity system causes various skin conditions such as eczema and allergies.
Reduces immunity to autoimmune diseases and can cause you to become more sensitive to infection. Symptoms include cellulitis, which causes skin inflammation, swelling, or inflammation. Measures should be taken to prevent infection.
All medications can affect rheumatoid arthritis rashes differently.
Below are four dermatology problems associated with RA that may cause rash-like symptoms. Symptoms typically occur on both sides of the body.
Palmar erythema, or red palms, can stem from various health conditions. About 60% of people with RA experience it. It happens when small blood vessels in hand become dilated, which draws more blood to the surface. Signs include redness of both palms that may extend to the fingers. A slight feeling of warmth may accompany the redness. Youll notice that the redness fades if you press on. Red palms do not typically hurt or itch. Vary in size and can be as small as a pea or as large as a golf ball.
Read Also: How To Tell If Your Hiv Positive
What Is The Outlook For People With Rheumatoid Arthritis Rashes
There are no permanent solutions that can completely prevent RA rashes from occurring. Doctors may try a combination of medications to help you manage your condition. These treatments may reduce inflammation and minimize joint damage.
Its important that people with RA take measures to live as healthy a lifestyle as possible. Examples of lifestyle practices that may benefit a person with RA include:
- Getting plenty of rest, which can help to reduce fatigue symptoms and minimize joint inflammation.
- Exercising whenever possible, which can help to enhance joint mobility and build strong, flexible muscles.
- Taking measures to cope with stress, such as meditation, reading, taking a walk, or doing other activities to promote relaxation.
- Eating a balanced diet full of fruits, vegetables, whole grains, and lean proteins. This can help you maintain a moderate weight, which is important in supporting joint health.
A Sensation Of Prickling Or Numbness In Your Hands
If your hands feel like theyre burning or numb, it may be a sign of carpal tunnel syndrome , which is a problem with the nerve that runs from the wrist to the fingers. CTS often occurs in people who have RA, according to CreakyJoints. Talk to your physician right away if you notice changes in how your hands feel. Theres no reason to live with pain or discomfort from CTS, and treatment helps preserve hand function. CTS treatment may include wrist splints worn at night, steroid injections, adjustments to RA medication, or less commonly, surgery that helps release the pressure on the nerves in the hands.
Don’t Miss: Where Did Aids Come From And How Did It Start
Rheumatoid Arthritis And Itching Attacks
Are you experiencing persistent and painful itching with rheumatoid arthritis ? Youre not alone. While itching is not a classic symptom of RA, myRAteam members are frequently plagued by prickly skin patches, rashes, and hives. Ill scratch and scratch. It makes me crazy! reported one member. It feels like something is crawling on me, said another. I’m literally digging myself raw, added one man.
Itching can be an allergic reaction or side effect of RA medication. It may also be related to an underlying condition – or the RA itself.
Treatment Of Rheumatoid Arthritis
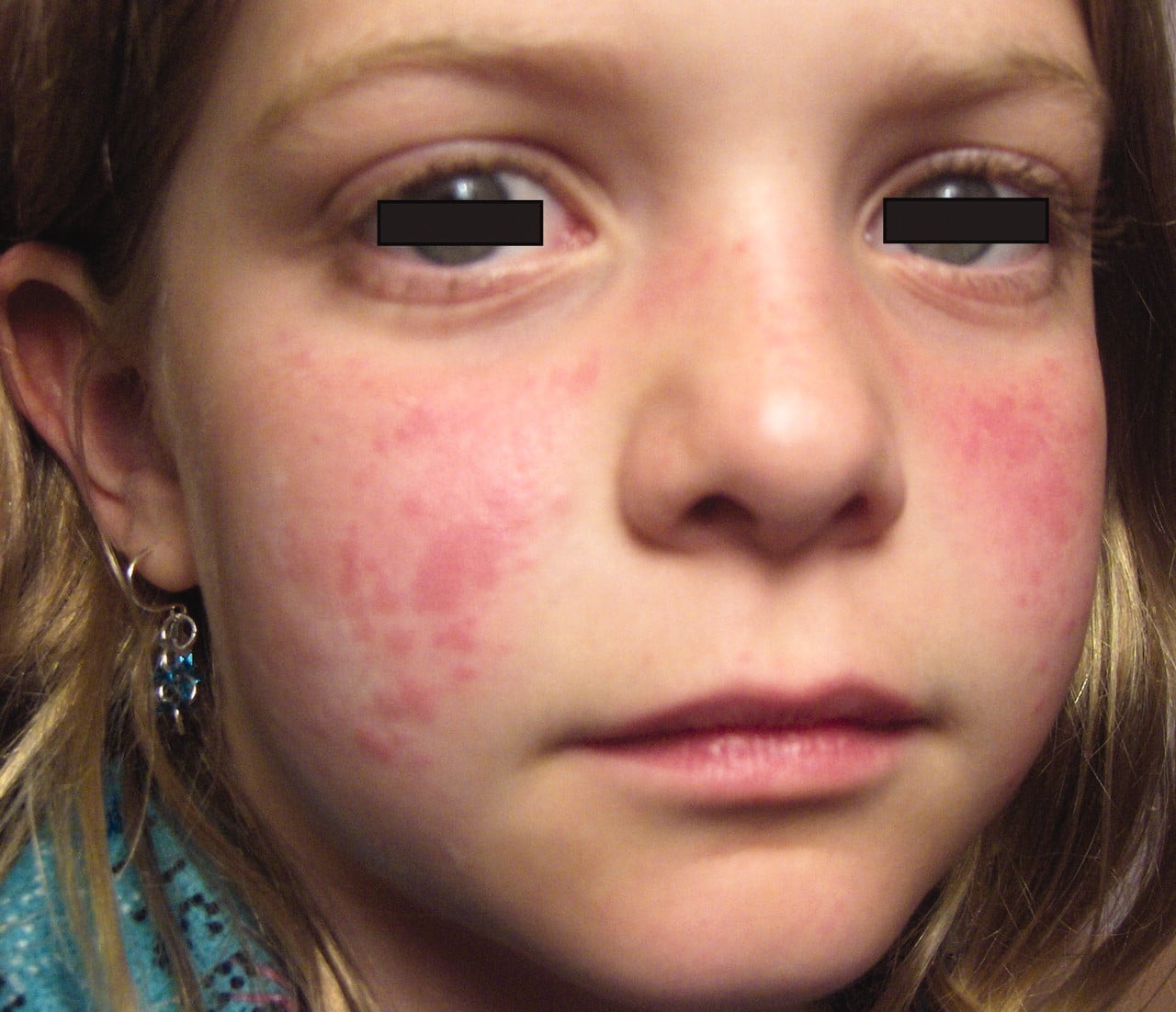
Treatment for RA rashes focuses on the underlying condition. Reducing the severity of RA symptoms will usually help clear up the rash.
In more severe cases of RA rash, a doctor may treat the rash directly. In these instances, a doctor may prescribe topical antibiotics or steroids to help treat or prevent any secondary infections.
Some people use skin creams and ointments to treat an RA rash. These can help reduce pain or itchiness. Topical steroids may also reduce swelling.
In cases where a reaction to RA medication directly causes a skin rash, a doctor can advise a person on how to reduce or replace their current medication.
Medications used to treat RA can also make a person more susceptible to other skin problems. For example, some drugs cause a person to bruise more easily or be more sensitive to sunlight.
Also Check: Is Hiv An Autoimmune Disease
How Rheumatoid Arthritis Affects More Than Joints
Learn more about how the inflammation associated with RA can impact organs and systems beyond the joints.
Arthritis can cause painful, swollen knees or fingers that are impossible to ignore. But other parts of the body, including the skin, eyes and lungs can also be affected. Rheumatoid arthritis is a systemic disease, meaning it can affect many parts of the body.
In addition, the drugs used to treat RA can also cause health problems. Many of these problems such as bone thinning or changes in kidney function cause no immediate symptoms so your doctor may monitor you through lab tests or checkups. For other problems such as skin rashes or dry mouth its important to report any symptoms to your doctor, who can determine the cause, and adjust your treatments accordingly.
Its important to be aware of the affected areas of the body and side effects you may experience. This way, early aggressive treatment can help you avoid RA-related health issues.
What Does A Rheumatoid Arthritis Rash Look Like
One of the most common general rashes for people with rheumatoid arthritis is reddened palms, or palmar erythema. One study found that almost 60 percent of those with RA reported palmar erythema at some point. It usually occurs on both hands and is not painful or itchy. The hands may feel slightly warmer than usual.
Eczema is a common skin condition characterized by an intensely itchy, red or purple rash. While eczema can occur without rheumatoid arthritis, one study found the rates of RA in those with atopic dermatitis were 72 percent higher than in the general population. Researchers are studying whether some forms of eczema are an autoimmune disease.
A small percentage of those with rheumatoid arthritis may develop a specific complication called cutaneous vasculitis. I had this rash on my ankles and legs when my RA flared up, but they diagnosed it as vasculitis, one myRAteam member said.
Cutaneous vasculitis is also sometimes referred to as rheumatoid vasculitis. It usually appears as a purplish rash on the skin. In more severe cases, skin ulcers may appear on the legs. The rash is often accompanied by lack of sensation, numbness, or tingling in the affected area. Other parts of the body may also experience symptoms of rheumatoid vasculitis: the liver or spleen may be enlarged, and hematuria can occur as well. Cutaneous vasculitis is an emergency, and you should talk to your rheumatologist about it right away if you notice symptoms.
Recommended Reading: How Can Someone Get Aids