Stage : The Asymptomatic Stage
Once a person has been through the acute primary infection stage and seroconversion process, they can often start to feel better. In fact, HIV may not cause any other symptoms for up to 10 or even 15 years .
However, the virus will still be active, infecting new cells and making copies of itself. HIV can still be passed on during this stage. If left untreated, over time, HIV infection will cause severe damage to the immune system.
How Have Deaths From Hiv/aids Changed Over Time
Global deaths from HIV/AIDS halved within a decade
The world has made significant progress against HIV/AIDS. Global deaths from AIDS have halved over the past decade.
In the visualization we see the global number of deaths from HIV/AIDS in recent decades this is shown by age group. In the early 2000s 2004 to 2005 global deaths reached their peak at almost 2 million per year.
Driven mostly by the development and availability of antiretroviral therapy , global deaths have halved since then. In 2017, just under one million died from the disease.
You can explore this change for any country or region using the change country toggle on the interactive chart.
HIV/AIDS once accounted for more than 1-in-3 deaths in some countries, but rates are now falling
Global progress on HIV/AIDS has been driven by large improvements in countries which were most affected by the HIV epidemic.
Today the share of deaths remains high: more than 1-in-4 deaths in some countries are caused by HIV/AIDS. But in the past this share was even higher.In the visualization we see the change in the share of deaths from HIV/AIDS over time. From the 1990s through to the early 2000s, it was the cause of greater than 1-in-3 deaths in several countries. In Zimbabwe, it accounted for more than half of annual deaths in the late 1990s.
We see that over the past decade this share has fallen as antiretoviral treatment has become more widely available.
Children living with HIV
New HIV infections of children
Although Strides Have Been Made In The Hiv Response Children Are Still Affected By The Epidemic
Of the estimated 38.0 million people living with HIV worldwide in 2020, 2.78 million were children aged 0-19. Each day in 2020, approximately 850 children became infected with HIV and approximately 330 children died from AIDS related causes, mostly because of inadequate access to HIV prevention, care and treatment services.
As of 2020, roughly 15.4 million children under the age of 18 had lost one or both parents to AIDS-related causes. Millions more have been affected by the epidemic, through a heightened risk of poverty, homelessness, school dropout, discrimination and loss of opportunities, as well as COVID-19. These hardships include prolonged illness and death. Of the estimated 680,000 people who died of AIDS-related illnesses in 2020, 120,000 of them were children under 20 years of age.
Global trends
In 2020, around 160,000 children aged 0-9 were newly infected with HIV, bringing the total number of children aged 0-9 living with HIV to 1.03 million . Nearly 90 per cent of these children live in sub-Saharan Africa. One bright spot on the global horizon is the rapid decline of approximately 52 per cent in new HIV infections among children aged 0-9 since 2010 due to stepped-up efforts to prevent mother-to-child transmission of HIV. However, the number of new HIV infections among adolescents has declined at a slower rate of about 38 per cent.
Geographic disparity
Recommended Reading: How Common Is It To Get Hiv
The Haitian Connection Controversy
The Haitian connection controversy refers to the debate regarding the origins of the HIV virus in Haiti and the United States and whether or not HIV was spread into the US by Haitians or into Haiti by Americans. The controversy began in the 1982, when the CDC noted that 34 cases of immunodeficient patients were Haitian. This “connection” noted by physicians caused the erroneous labeling of Haitians as a risk factor group for HIV, leading to the rise of the term “the 4-H’s” referring to Homosexuals, Hemophiliacs, Heroin addicts, and Haitians as the major groups prone to HIV infection.
In his 1990 book “AIDS and Accusation,” Paul Farmer refutes the idea that Haiti was an HIV entry point to the USA. Referencing an epidemiological study on the prevalence of sarcomas associated with HIV/AIDS contraction, Farmer suggests that Cambronne’s plasma business occurred before identifiers of HIV infection were recorded in Haiti, indicating that the disease did not arrive in Haiti until at least the late-1970s. Farmer instead argues that HIV/AIDS in Haiti was introduced by visitors from the US.
Regardless of origin, the consequences of HIV/AIDS in Haiti were severe. The disease spread rapidly throughout Haiti, infecting thousands. Haiti’s burgeoning tourist industry suffered greatly from the association with HIV/AIDS, and Haitians living in the USA were placed on the banned list for blood donations, alongside homosexuals and intravenous drug users, until 1990.
Key Points: Hiv Incidence
HIV incidence declined 8% from 2015 to 2019. In 2019, the estimated number of HIV infections in the U.S. was 34,800 and the rate was 12.6 .
, the annual number of HIV infections in 2019, compared with 2015, decreased among persons aged 1324 and persons aged 45-54, but remained stable among all other age groups. In 2019, the rate was highest for persons aged 25-34 , followed by the rate for persons aged 35-44 .
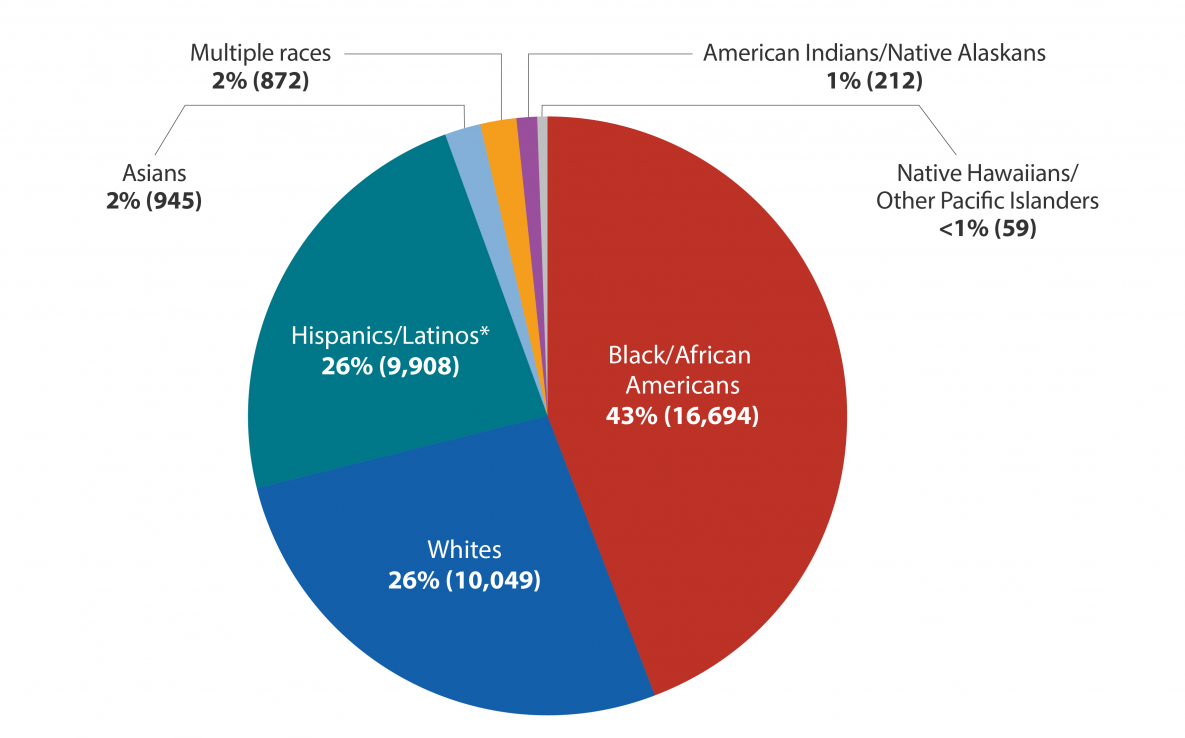
, the annual number of HIV infections in 2019, compared with 2015, decreased among persons of multiple races, but remained stable for persons of all other races/ethnicities. In 2019, the highest rate was for Blacks/African American persons , followed by Hispanic/Latino persons and persons of multiple races .
, the annual number of new HIV infections in 2019, as compared to 2015, decreased among males, but remained stable among females. In 2019, the rate for males was 5 times the rate for females .
, the annual number of HIV infections in 2019, compared with 2015, decreased among males with transmission attributed to male-to-male sexual contact, but remained stable among all other transmission categories. In 2019, the largest percentages of HIV infections were attributed to male-to-male sexual contact
For more details on recent HIV incidence statistics, see Estimated HIV Incidence and Prevalence in the United States, 2015-2019.
Also Check: Can You Get Hiv Through Oral Sex
People With Diagnosed Hiv In The Us And Dependent Areas By Region Of Residence 2019*
*Rates per 100,000 people.
a American Samoa, Guam, the Northern Mariana Islands, Puerto Rico, the Republic of Palau, and the US Virgin Islands.b In the 50 states and the District of Columbia.c The term male-to-male sexual contact is used in CDC surveillance systems. It indicates a behavior that transmits HIV infection, not how individuals self-identify in terms of their sexuality.d Includes infections attributed to male-to-male sexual contact and injection drug use .
Hiv Treatment And Prevention
Nearly 75% of HIV treatment in Haiti is sponsored and overseen by the NGOs Partners In Health and Haitian Study Group on Kaposi’s Sarcoma and Opportunistic Infections in collaboration with the Haitian Ministry of Health. Alongside them, the Joint United Nations Team on AIDS in Haiti also helps provide the resources to tackle HIV through prevention, treatment, and testing, accelerating the nationwide HIV response. As of 2016, around 55% of HIV positive Haitians received antiretroviral therapy.
Recommended Reading: When Was The First Case Of Hiv
Estimates Number Of New Hiv Infections
The Agency estimates that 2,242 new infections occurred in Canada in 2018. This estimate is a slight increase from the estimate for 2016 .
The resulting estimated incidence rate in Canada for 2018 was 6.0 per 100,000 population which is a slight increase from the estimate for 2016 .
Figure 8. HIV incidence: Estimated annual number of new HIV infections in Canada
This graph shows the point estimates of new HIV infections by year with each associated plausible ranges for point estimates. The vertical axis shows the estimated number of new HIV infections per year, with the low and high ranges. The horizontal axis shows the calendar years.
| Year |
|---|
| gbMSM-PWID | 2.7% |
Among the estimated new infections in 2018, an estimated 1,109 were among gay, bisexual and other men who have sex with men , representing just under half of all new HIV infections in 2018, despite representing approximately 3-4% of the Canadian adult male population. Although the gbMSM population continues to be over-represented in new HIV infections in Canada, the proportion of new infections among this population has decreased compared to 2016. .
Three hundred and twelve of the estimated new infections in 2018 were among people who inject drugs , accounting for 13.9% of new infections. The proportion of new infections attributed to heterosexuals increased slightly to 34.0% from 31.7% in 2016.
What Is The Impact Of Hiv On Racial And Ethnic Minorities In The Us
HIV can affect anyone regardless of sexual orientation, race, ethnicity, gender, age, or where they live. However, in the United States, some racial/ethnic groups are more affected than others, given their percentage of the population. This is because some population groups have higher rates of HIV in their communities, thus raising the risk of new infections with each sexual or injection drug use encounter. Additionally, a range of social, economic, and demographic factors such as stigma, discrimination, income, education, and geographic region can affect peoples risk for HIV.
Black/African American and Hispanic/Latino communities are disproportionately affected by HIV compared to other racial/ethnic groups. For example, in 2018 Blacks/African Americans represented 13% of the US population, but 41% of people with HIV. Hispanics/Latinos represented 18% of the population, but 23% of people with HIV.
Source: CDC, Estimated HIV incidence and prevalence in the United States, 20142018.
Certain subpopulations within racial and ethnic minority groups are affected as well. For example, gay, bisexual and other men who have sex with men are by far the most affected group in the US. They account for about 70% of new infections each year, even though they make up only 2% of the population.
According to CDC, in 2018:
For in-depth information about the impact of HIV on different racial and ethnic populations, see these CDC fact sheets:
Read Also: Is Hiv Curable Or Treatable
Is There A Cure For Aids
There is still no cure for AIDS. And while new drugs are helping some people who have HIV live longer, healthier lives, there are many problems associated with them:
-
Anti-HIV drugs are highly toxic and can cause serious side effects, including heart damage, kidney failure, and osteoporosis. Many patients cannot tolerate long-term treatment with HAART.
-
HIV mutates quickly. Even among those who do well on HAART, roughly half of patients experience treatment failure within a year or two, often because the virus develops resistance to existing drugs. In fact, as many as 10 to 20 percent of newly infected Americans are acquiring viral strains that may already be resistant to current drugs.
-
Because treatment regimens are unpleasant and complex, many patients miss doses of their medication. Failure to take anti-HIV drugs on schedule and in the prescribed dosage encourages the development of new drug-resistant viral strains.
-
Even when patients respond well to treatment, HAART does not eradicate HIV. The virus continues to replicate at low levels and often remains hidden in “reservoirs” in the body, such as in the lymph nodes and brain.
In the U.S., the number of AIDS-related deaths has decreased dramatically because of widely available, potent treatments. But more than 95 percent of all people with HIV/AIDS live in the developing world, and many have little or no access to treatment.
Hiv And Tuberculosis In South Africa
South Africa has the world’s sixth largest tuberculosis epidemic, and the disease is the leading cause of death in the country.120 South Africas HIV epidemic fuels the TB epidemic because people living with HIV are at a far higher risk of developing TB due to weakened immune systems. It is estimated that 60% of people living with HIV in South Africa are also co-infected with TB. In 2017 there were 193,000 new cases of TB among people living with HIV and 56,000 people living with HIV died due to a TB-related illness.121
In light of this, the South African National AIDS council combined the HIV and STI strategy with the national TB strategy to improve the integration of these two services. One of the aims of this strategy is to get more people living with HIV on isoniazid preventative therapy , a preventative medicine for TB.122 But as of 2017, only around half of people living with HIV in the country had access to IPT.123
The TB treatment success rate has improved in recent years, and stood at 83% in 2016.124
We cannot fight AIDS unless we do much more to fight TB.
Don’t Miss: Where Did Hiv Aids Begin
Hiv Prevention Programmes In Nigeria
Nigeria accounted for 59% of all new HIV infections in West and Central Africa in 2016.73 This rate of new infections has remained relatively stable in recent years, with only a 5% decrease between 2017 and 2010.74
The National Strategic Framework laid out by the NACA, outlined key targets for the next five years: aiming to provide 90% of the general population with HIV prevention interventions by 2021 and for 90% of key populations to be adopting HIV risk reduction behaviours by 2021. They identify strengthening community structures as being a main way to achieve this.75
Health Resources And Services Administrations Health Center Program
- COVID-19 Information for Health Centers and PartnersThis page provides the latest information on COVID-19 for health centers and Health Center Program partners. HRSA-funded health centers are a vital part of the nations response to HIV.
- Interpersonal Violence Toolkit and COVID-19 Resource PageFutures Without Violence, a HRSA-funded National Training and Technical Assistance Partner, developed this toolkit to assist health centers in designing a comprehensive response to IPV and human trafficking. During COVID-19, increases in IPV have been reported across the US there is a strong association between IPV and risks for HIV infection.
Also Check: Who Was The First Person To Get Hiv
How Many People Are Infected With Hiv Worldwide
- 36.9 million people worldwide live with HIV .
- Of these, 21.7 million people have access to antiretroviral therapy. This is 2.3 million more than in 2016 and almost 14 million more than in 2010.
- 940.000 people died of AIDS in 2017, compared to 1.5 million in 2010.
- In 2017, around 1.8 million people around the world were newly infected with HIV, the same number as in the previous year.
- In eastern and southern Africa, where more than 50% of people are living with HIV, the number of adult new infections has fallen the most in the world, by a total of 30% since 2010.
- In Eastern Europe and Central Asia, by contrast, the number of new infections has risen by 30% in the last six years.
- In terms of the UNAIDS * 90-90-90 targets, in 2017, 75% of people living with HIV worldwide knew about their status, 79% of whom had access to treatment, and 81% of those had a suppressed viral load.
Key Messages About Covid
Widespread vaccination is a critical tool to help stop the pandemic. Here are three key messages we need to share:
- Everyone over 12 years of age, regardless of HIV status, get vaccinated.
- Those with advanced HIV disease and/or not on medications, get a third dose of the vaccine.
- Those in HIV care and treatment who are virally suppressed, talk with your health care provider about the need for an additional dose.
Harold J. Phillips, Director, White House Office of National AIDS Policy
Read Also: How Long Can Hiv Live Outside The Body
Hiv/aids Annual Surveillance Statistics
The following tables provide annual data on new diagnoses of HIV , concurrent HIV/AIDS and AIDS, as well as the number of persons living with HIV and AIDS and the number of deaths among persons with HIV and AIDS. The data are shown for New York City overall and by sex, race, age, borough, area-based poverty level, risk factor, and United Hospital Fund neighborhood.
Impact On Young People
- Teens and young adults continue to be at risk, with those under 35 accounting for 57% of new HIV diagnoses in 2019 .51 Most young people are infected sexually.52
- Among young people, gay and bisexual men and minorities have been particularly affected.53
- Perinatal HIV transmission, from an HIV-infected mother to her baby, has declined significantly in the U.S., largely due to increased testing efforts among pregnant women and ART which can prevent mother-to-child transmission.54,55,56
- A recent survey of young adults found that HIV remains a concern for young people, especially for young people of color.57
Recommended Reading: Did Hiv Come From Monkeys
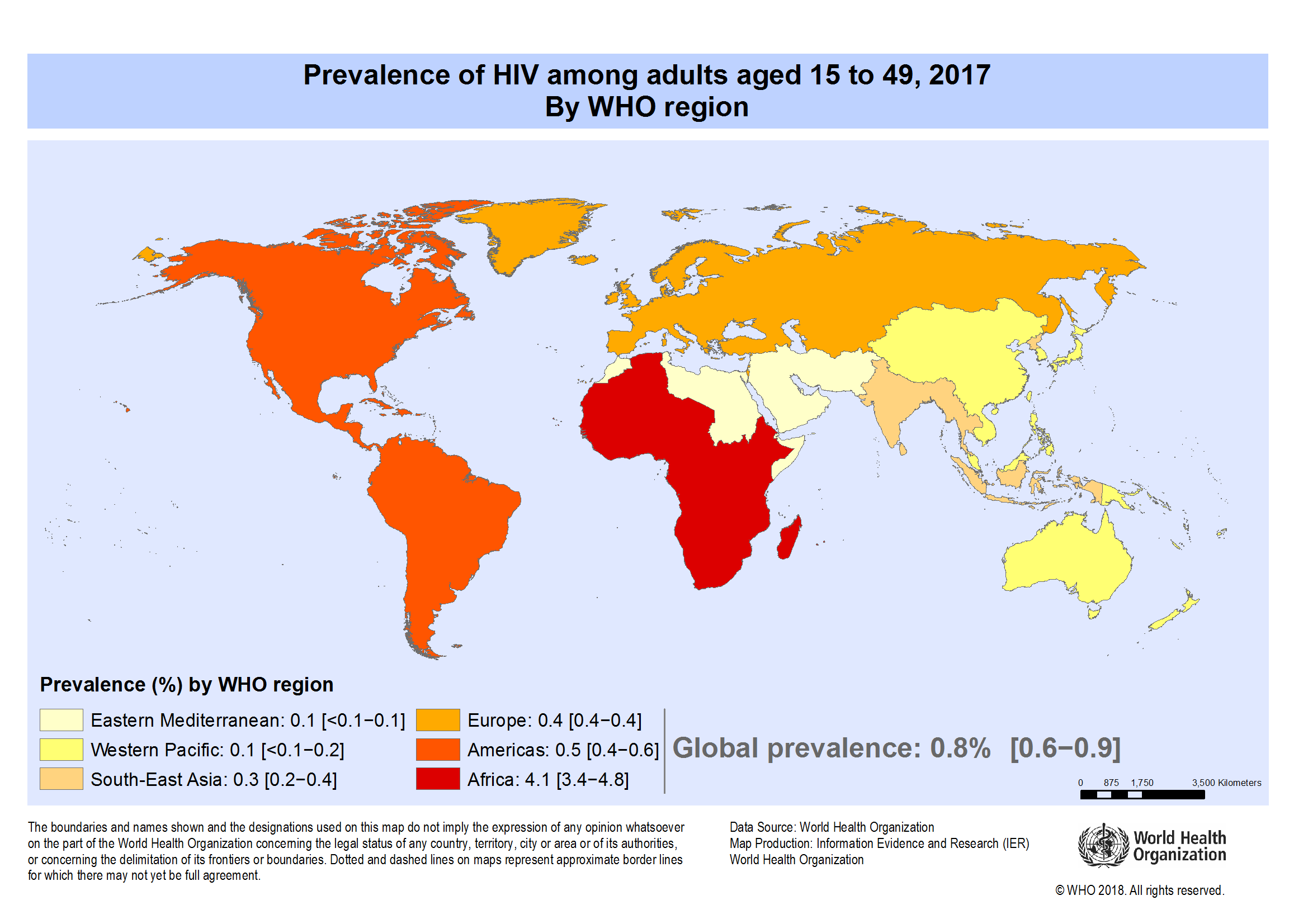
What Is The Global Prevalence Of Hiv Infection
According to the Joint United Nations Programme on HIV/AIDS , worldwide in 2018, approximately 37.9 million people were infected with HIV. UNAIDS estimates that approximately 1.7 million people were newly infected with HIV and that 770,000 people died of AIDS in 2018, both statistics showing a decline over time.
The vast majority of infections remain in sub-Saharan Africa, where 5.2% of the population is believed to be infected. Between 2004 and 2006, the prevalence of HIV infection in central and eastern Asia and Eastern Europe increased by 21%. During this period, the number of new HIV infections in persons aged 15 to 64 years rose by 70% in Eastern Europe and central Asia.
The infection rates in many developed countries remain stable, and some developing countries have achieved significant gains in controlling and even reversing the effects of the HIV epidemic. However, this is partially due to deaths in HIV-infected people, together with simultaneous prevention of new infections. India, for example, has used a national prevention campaign focusing on high-risk populations that may have prevented 100,000 new HIV infections over the 5 years it has been implemented, with increasing results seen in areas with higher levels of investment. These figures together show that global HIV infection is in a state of flux.
Swaziland has the highest overall prevalence of HIV infection .
References
Weber J. The pathogenesis of HIV-1 infection. Br Med Bull. 2001. 58:61-72. .