Number Of People Dying From Hiv
Situation and trends:650 000 people died of HIV-related illnesses worldwide in 2021. Expanded access to antiretroviral therapy and a declining incidence of HIV infections have led to a steep fall globally in the number of adults and children dying from HIV-related causes. The estimated 650 000 people dying from HIV globally in 2021 were 68% fewer than in 2004 and 52% fewer than in 2010 in spite of a period of substantial population growth in many high burden countries.Nevertheless, there is no room for complacency. Countries need to live up to their commitment to end the AIDS epidemic as a public health threat by 2030 a target included in the 2030 Agenda for Sustainable Development adopted by the United Nations General Assembly in September 2015.The drop in HIV-related mortality is especially evident in the regions with the greatest burden of HIV infection, including the WHO African Region, home to over 64% of people dying from HIV-related causes in 2021. An estimated 420 000 people died in the African Region from HIV-related causes in 2021, which indicates that mortality has dropped by almost 55% since 2010.
Key Points: Hiv Incidence
- HIV incidence declined 8% from 2015 to 2019. In 2019, the estimated number of HIV infections in the U.S. was 34,800 and the rate was 12.6 .
- , the annual number of HIV infections in 2019, compared with 2015, decreased among persons aged 1324 and persons aged 45-54, but remained stable among all other age groups. In 2019, the rate was highest for persons aged 25-34 , followed by the rate for persons aged 35-44 .
- , the annual number of HIV infections in 2019, compared with 2015, decreased among persons of multiple races, but remained stable for persons of all other races/ethnicities. In 2019, the highest rate was for Blacks/African American persons , followed by Hispanic/Latino persons and persons of multiple races .
- , the annual number of new HIV infections in 2019, as compared to 2015, decreased among males, but remained stable among females. In 2019, the rate for males was 5 times the rate for females .
- , the annual number of HIV infections in 2019, compared with 2015, decreased among males with transmission attributed to male-to-male sexual contact, but remained stable among all other transmission categories. In 2019, the largest percentages of HIV infections were attributed to male-to-male sexual contact
For more details on recent HIV incidence statistics, see Estimated HIV Incidence and Prevalence in the United States, 2015-2019.
New Hiv Diagnoses And People With Diagnosed Hiv In The Us And Dependent Areas By Area Of Residence 2020*
Data for 2020 should be interpreted with caution due to the impact of the COVID-19 pandemic on access to HIV testing, care-related services, and case surveillance activities in state and local jurisdictions.* Among people aged 13 and older.Source: CDC.Diagnoses of HIV infection in the United States and dependent areas, 2020. HIV Surveillance Report2022 33
Don’t Miss: Can Hiv Have No Symptoms
New Hiv Infection Rates
New HIV infection rates have dropped over the years. The world has seen a 52% reduction in new HIV infections since the epidemic peaked in 1997. In 1997, 3 million people reported new HIV infections, compared with only 2.1 million in 2010 and 1.5 million in 2020.
This is because people in resource-poor countries now have significantly improved access to HIV treatments. Preventing vertical transmission of HIV, which refers to when the infection passes from a birthing parent to their fetus, has also contributed to lowering transmission rates. Additionally, the medical community has added new HIV prevention tools and methods.
However, the unequal distribution of HIV treatment and prevention strategies still leaves many vulnerable populations behind. Important barriers to improving access to care include stigma, discrimination, social inequities, and exclusion.
Before the COVID-19 pandemic, many people with HIV or at risk of HIV still did not have access to prevention, care, and treatment. The pandemic caused a greater disturbance in the distribution of health services in many countries. Some countries report a 75% disruption of HIV services.
According to UNAIDS, the Joint United Nations Programme on HIV/AIDS, the benefits of providing HIV services outweigh the risk of dying from COVID-19.
HIV spreads through contact with bodily fluids from people who have the virus. Bodily fluids that carry HIV include:
It is not possible to contract HIV through:
Aids Cases In 1985 Exceed Total Of All Previous Years
More people were stricken with AIDS in 1985 than in all of the earlier six years since the fatal disease was discovered, the federal Centers for Disease Control reported yesterday in a regular update.
Last year the AIDS epidemic claimed 8,406 new victims, bringing the total of reported cases in the United States, as of Jan. 13, to 16,458. The 1985 figures showed an 89 percent increase in new AIDS cases compared with 1984.
Of all AIDS cases to date, 51 percent of the adults and 59 percent of the children have died. The new report shows that, on average, AIDS patients die about 15 months after the disease is diagnosed.
The rate of increase was expected and confirmed forecasts by public health experts. The same experts say the epidemic shows no sign of slowing and that 1986 is virtually certain to witness almost twice as many new AIDS cases as were counted last year.
“It continues to be very bad news, but it comes as no surprise,” said Meade Morgan, chief the statistics section at CDC’s AIDS program.
Morgan did, however, point to one good sign in the report. The period of time it takes for the number of AIDS cases to double has continued to lengthen slowly. This confirms earlier indications that the disease was not spreading as fast as the earliest statistics indicated.
In 1982, for example, the number of cases was doubling every five months. Through 1983 and 1984 each doubling came after longer and longer intervals. The most recent doubling took 11 months.
Don’t Miss: Does Blood Test Show Hiv
Too Many People Living With Hiv In The Us Dont Know It
HIV.gov| June 10, 2019
Topics
Approximately 1.1 million people in the United States are living with HIV today. But not all of them know it. In fact, about 15 percent of them are not aware they are living with HIV. That means there are approximately 165,000 people in the U.S. who do not know that they are living with HIV. They are not getting the care and treatment that can preserve their health and protect their partners from getting HIV, too.
Recommended Reading: What Does It Mean To Be Hiv Positive
Hiv/aids Is One Of The Worlds Most Fatal Infectious Disease
Almost 1 million people die from HIV/AIDS each year in some countries its the leading cause of death
HIV/AIDS is one of the worlds most fatal infectious diseases particularly across Sub-Saharan Africa, where the disease has had a massive impact on health outcomes and life expectancy in recent decades.
The Global Burden of Disease is a major global study on the causes of death and disease published in the medical journal The Lancet.1 These estimates of the annual number of deaths by cause are shown here. This chart is shown for the global total, but can be explored for any country or region using the change country toggle.
In the chart we see that, globally, it is the second most fatal infectious disease.
According to the Global Burden of Disease study, almost one million people died from HIV/AIDS in 2017. To put this into context: this was just over 50% higher than the number of deaths from malaria in 2017.
Its one of the largest killers globally but for some countries particularly across Sub-Saharan Africa, its the leading cause of death. If we look at the breakdown for South Africa, Botswana or Mozambique which you can do on the interactive chart we see that HIV/AIDS tops the list. For countries in Southern Sub-Saharan Africa, deaths from HIV/AIDS are more than 50% higher than deaths from heart disease, and more than twice that of cancer deaths.
Read Also: How Soon Would Hiv Symptoms Show
Is Canada Reaching The Global 90
The Joint United Nations Programme on HIV/AIDS and the World Health Organization have established a global health sector strategy on HIV to help eliminate AIDS as a public health threat by 2030. Canada has endorsed this strategy. The strategy can be encapsulated in the phrase 90-90-90 and consists of the following targets for the year 2020:
- 90% of people with HIV know their infection status
- 90% of people diagnosed with HIV receive HIV treatment
- 90% of people taking treatment have an undetectable viral load
Canada is approaching the 90% goal for awareness of HIV status and the 90% goal for treatment and has surpassed the 90% goal for achieving viral suppression. Of the estimated 62,050 people with HIV in Canada in 2018, an estimated:
- 87% were diagnosed and aware they had HIV
- 85% of those who were diagnosed were on treatment
- 94% of those on treatment had achieved viral suppression
This means that 70% of all Canadians with HIV had achieved viral suppression in 2018. If all 90-90-90 measures had been reached, 73% of all Canadians with HIV would have achieved viral suppression.
The Epidemiology Of Hiv In Canada
This fact sheet provides a snapshot of the HIV epidemic in Canada. All epidemiological information is approximate, based on the best available data. Most of the data contained in this fact sheet come from the latest estimates from the Public Health Agency of Canada, which are for the year 2018. More information can be found in the section Where do these numbers come from? at the end of the fact sheet.
You May Like: How Long Does It Take For Hiv Symptoms To Develop
Hiv/aids Is Still A Leading Cause Of Death For Young People
Suzanne Brennan Firstenberg’s ‘In America: Remember’, a memorial for Americans killed by Covid-19, stands on the National Mall in Washington. Reuters
Covid-19 has now killed about 730,000 people in the US, making it the deadliest pandemic in the nation’s history, with more lives claimed than by HIV/Aids.
The tally comes as the US marks four decades since HIV the virus that can cause Aids was first detected in the country, and some are now looking at the two vastly different diseases and seeing parallels.
The US government’s initial approach to both HIV/Aids and Covid was denial and indifference.
As Aids rampaged through communities in New York, San Francisco and elsewhere in the early 1980s, the administration of former president Ronald Reagan looked the other way.
Even as the disease claimed tens of thousands of American lives, Reagan slashed spending on public health agencies, and it wasn’t until 1987 that he recognised the pandemic.
I wish in the HIV response, they tried to bring all Americans along, and it wasn’t just a problem that was in certain communities, Kevin Fisher, director of policy, data and analysis for the Aids Vaccine Advocacy Coalition, told The National.
If they brought everybody along and said this is something that we all need to figure out, then it would have been better.
They’re both diseases that kind of prey on human intimacy, despite differences in how they’re spread, Mr Fisher said.
The US leads the world in deaths from Covid.
Therapies Came In The Late 80s And 90s
The tide started to turn in the late 80s and 90s, as more effective therapies became available and transformed what it meant for an individual to live with HIV.
On March 19, 1987, the Food and Drug Administration approved an antiretroviral drug known as AZT to treat HIV infection.
Another important change also happened that year.
After pressure from activists fighting for their communitys survival, the FDA issued new regulations around clinical drug trials making it possible for patients to access experimental, potentially life-saving therapies without having to wait years for official agency approval.
One of those activists was Ryan White, an Indiana teenager who contracted AIDS in 1984 through contaminated needles while being treated for hemophilia. He experienced discrimination in his community after his diagnosis, even being denied entry to his middle school. As White spoke publicly about his experiences and his family challenged his treatment in court, he became one of the early public faces of the disease.
Princess Diana was also instrumental in shattering stigmas and myths around the illness, famously photographed visiting HIV/AIDS patients in hospital wards and shaking hands with them without gloves.
And in 1991, NBA star Earvin Magic Johnson revealed he had been diagnosed with HIV his identity as a straight, Black man helped demonstrate that anyone could contract the disease.
Also Check: Hiv Viral Load And Transmissibility Of Hiv Infection
How Does Cdc Know The Number Of People Living With Hiv If Some Of Those People Are Unaware Of Their Status
CDC estimates the number of people living with HIV by using a scientific model. This model helps CDC estimate the number of new HIV infections and how many people are infected but dont know it. HIV prevalence is the number of people living with HIV infection at a given time, such as at the end of a given year. More information on HIV prevalence.
Are Some Regions Of The United States More Impacted By Hiv Than Others
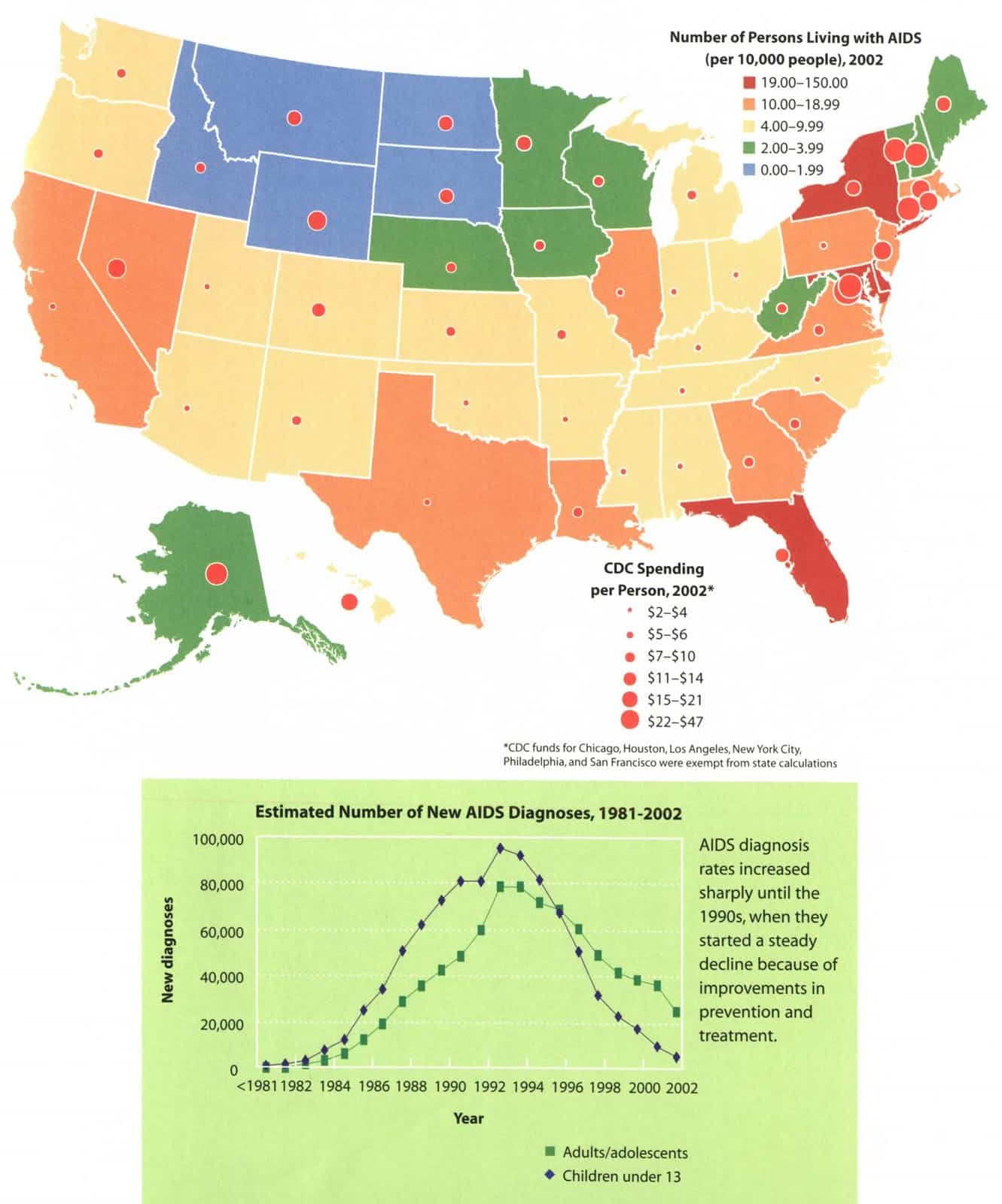
Yes. HIV is largely an urban disease, with most cases occurring in metropolitan areas with 500,000 or more people. The South has the highest number of people living with HIV, but if population size is taken into account, the Northeast has the highest rate of people living with HIV.
*Rates per 100,000 people. Includes adults, adolescents, and children under the age of 13.
Also Check: Is Hiv And Aids Curable
Delayed Diagnosis And Treatment Leads To Deaths
In MSF-supported hospitals in the Democratic Republic of Congo, Guinea, Malawi and elsewhere, many deaths occur within 48 hours of people being admitted to hospital, explains Dr Gilles Van Cutsem, leader of MSFs HIV/AIDS Working Group. People arrive very ill, often with severe opportunistic infections such as tuberculosis, cryptococcal meningitis, or Kaposis sarcoma. When they arrive, sometimes its too late to save them. They might not have been diagnosed on time or they failed to get access to a lifesaving treatment.
AIDS-related deaths are primarily driven by delayed diagnosis, treatment interruptions and virologic and immunologic failure among HIV treatment-experienced people. The World Health Organization estimates that more than 30 per cent of people who start HIV treatment worldwide have advanced disease with severe immune suppression, which puts them at a very high risk of contracting opportunistic infections and dying.
HIV/AIDS
Nearly 700,000 people died from HIV-related causes, while 1.5 million people became newly infected with the HIV virus in 2020.
If primary care clinics are not equipped and trained to detect advanced HIV, people at risk will remain undetected and untreated they will deteriorate until they are terminally ill.
How Does Hiv Affect Different Groups Of People
There are different ways to answer this question.
In 2020, male-to-male sexual contactdaccounted for68% of all new HIV diagnoses in the United States and dependent areas.In the same year, heterosexual contact accounted for 22% of all HIV diagnoses.
Data for 2020 should be interpreted with caution due to the impact of the COVID-19 pandemic on access to HIV testing, care-related services, and case surveillance activities in state and local jurisdictions.NOTE: Does not include other and perinatal transmission categories.* Among people aged 13 and older.
If we look at HIV diagnoses by race and ethnicity, we see that Black/African American people are most affected by HIV. In 2020, Black/African American people accounted for 42% of all new HIV diagnoses. Additionally, Hispanic/Latino people are also strongly affected. They accounted for 27% of all new HIV diagnoses.
Data for 2020 should be interpreted with caution due to the impact of the COVID-19 pandemic on access to HIV testing, care-related services, and case surveillance activities in state and local jurisdictions.* Among people aged 13 and older.Black refers to people having origins in any of the Black racial groups of Africa. African American is a term often used for people of African descent with ancestry in North America.Hispanic/Latino people can be of any race.
The most affected subpopulation is Black/African American gay and bisexual men.
You May Like: How Bad Are Hiv Symptoms
Hiv Statistics From 2020 Recognize Baton Rouge As The Leading City In The Us Regarding The Highest Hiv Rates
In accordance with the most recent figures, Baton Rouge is the city with the highest HIV rates in America. Shared needles are the main source of infection as the city struggles with opioid abuse. Miami, Florida, is in second place, while the third-place belongs to New Orleans, Louisiana. Other cities in the top ten list in descending order are Jackson , Orlando , Memphis , Atlanta , Columbia , Jacksonville , and Baltimore .
Recommended Reading: What Is The Most Common Method Of Hiv Transmission
Impact Across The Country
- Although HIV has been reported in all 50 states, the District of Columbia, and U.S. dependencies, the impact of the epidemic is not uniformly distributed.
- Ten states accounted for about two-thirds of HIV diagnoses among adults and adolescents in 2019 .31 Regionally, the South accounted for more than half of HIV diagnoses in 2019.32
- Rates of HIV diagnoses per 100,000 provide a different measure of the epidemicâs impact, since they reflect the concentration of diagnoses after accounting for differences in population size across states. The District of Columbia has the highest rate in the nation, compared to states, nearly 3 times the national rate and Georgia was the state with highest rate , twice that of the national rate.33,34 Nine of the top 10 states by rate are in the South.35
- New HIV diagnoses are concentrated primarily in large U.S. metropolitan areas , with Miami, Orlando, and Atlanta topping the list of the areas most heavily burdened.36
| Table 1: Top Ten States/Areas by Number and Rate of New HIV Diagnoses , 2019 | |
| State | |
| U.S. Rate | 13.2 |
| CDC. HIV Surveillance Report, Diagnoses of HIV Infection in the United States and Dependent Areas, 2019 vol. 32. May 2021. |
Don’t Miss: How Long Can You Have Hiv Without Knowing It