Hiv Rashes Caused By Medication
Drugs that treat HIV and related infections can trigger rashes. These often go away several days or weeks after you stop taking the drug. Talk with your doctor before stopping any medication.
If you have a rash along with fever, fatigue, headache, muscle pains, upset stomach, vomiting, and belly pain, you might have a âhypersensitivity reaction,â which can happen with several HIV medications, including:
Get medical help right away if you have those symptoms or if you have:
- Fever
- Painful red or purplish rash
- Blisters that spread on your skin and around your mouth, nose, and eyes
These could be signs of Stevens-Johnson syndrome, a severe form of hypersensitivity reaction. Itâs rare but can be life-threatening.
How Do Healthcare Providers Treat Kaposi Sarcoma
Healthcare providers treat each type of Kaposi sarcoma in different ways. There are many ways to treat this cancer. For example, acquired Kaposi sarcoma treatment might simply be eliminating the immunosuppressant drugs that cause people to develop lesions.
What is the treatment for epidemic Kaposi sarcoma?
Healthcare providers typically use a combination of anti-AIDS drugs to treat someone who has Kaposi sarcoma Kaposi and Human Immunodeficiency Virus/Acquired Immune Deficiency . Treating the underlying AIDS/HIV infection can shrink lesions. Other options include:
- Highly active antiretroviral therapy or HAART.
What is the treatment for classic or Mediterranean Kaposi sarcoma?
Treatments might include:
- Cryosurgery, which uses extremely cold chemical to treat lesions.
- Electrocoagulation, where providers treat lesions using heat from an electric current.
What Are Monkeypox Symptoms Heres What You Need To Know
For dozens of countries that do not typically encounter monkeypox, the fast-moving outbreak has caught both health officials and patients off guard. The World Health Organization declared monkeypox a global emergency on July 23, but in the United States, where the federal response and communication around the crisis has a ways to go, many people dont know how it spreads, what it looks like or what care they can get if they suspect theyve been infected.
Thats true in part because were still learning about how the monkeypox virus, or MPV, is behaving during this outbreak. We know it spreads via close skin-to-skin contact and, in some cases, through certain objects or fabrics . But WHO Director-General Tedros Adhanom Ghebreyesus noted in a statement regarding the declaration that the current crisis is being fueled by new modes of transmission, about which we understand too little.
One of the issues for epidemiologists is thinking about whether maybe sustains itself better in the human population than we realize, said Stephen Morse, an epidemiology professor at the Columbia University Medical Center.
The U.S. currently has the most confirmed monkeypox cases more than 5,000 compared to any other country, according to the Centers for Disease Control and Prevention. San Francisco issued a local emergency declaration on July 28 in order to mobilize resources and personnel to respond to the escalating crisis. New York City officials on July 30.
Read Also: Post Exposure Prophylaxis Treatment For Hiv
What Does An Hiv Rash Look Like
Usually HIV infection leads to a brief period of symptoms shortly after infection occurs. Not everybody notices these symptoms, and theyre easy to mistake for a cold or the flu. One of the symptoms may be a rash.
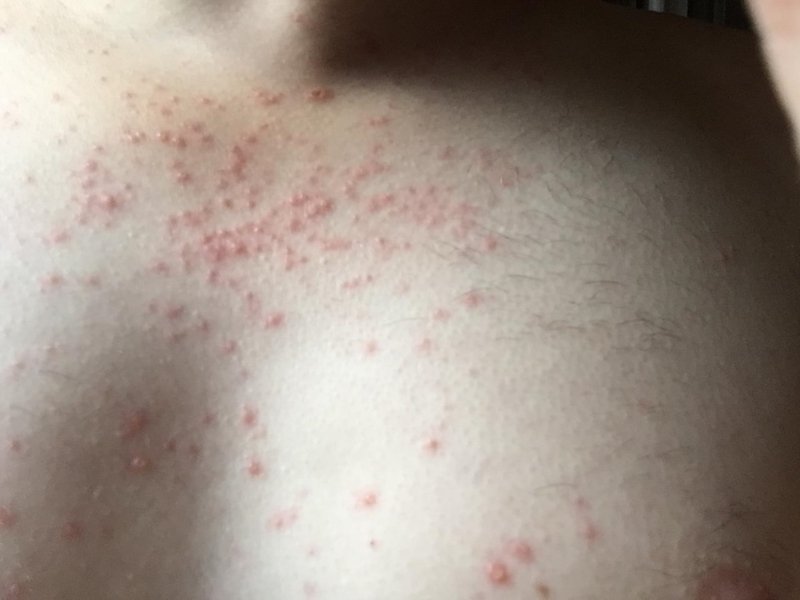
The most common HIV rash occurs shortly after infection. It is an itchy rash that usually appears on the abdomen, face, arms, or legs and features a flat, red area covered in small red bumps.
What Is Kaposi Sarcoma
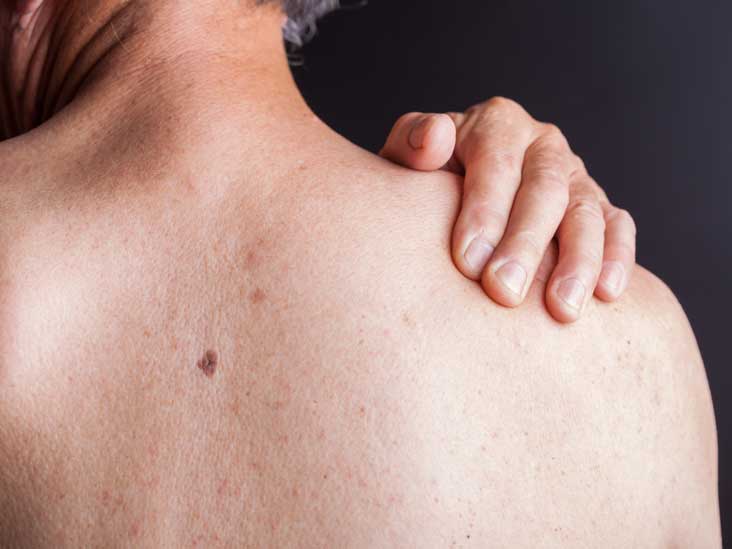
Kaposi sarcoma is a rare cancer that gained widespread attention during the early days of Human Immunodeficiency Virus/Acquired Immune Deficiency infections. Since then, innovative medical research and treatment significantly reduced the number of Kaposi sarcoma cases.
People with weakened immune systems are susceptible to Kaposi sarcoma. That said, people only develop Kaposi sarcoma if they are infected with human herpesvirus 8 . HHV-8 is a rare virus. Less than 10% of people in the United States carry HHV-8. This virus is believed to be transmitted via saliva.
Kaposi sarcomas most common visible symptom is dark-colored flat or bumpy blotches or patches that appear on a person’s arms, legs and face. The patches or blotches, called lesions, can be blue, black, pink, red or purple. Lesions might also appear in a person’s mouth, nose and throat. Lesions can spread to internal organs such as the liver, lungs, stomach and the digestive tract.
Recommended Reading: How Many People Have Hiv And Aids
Monkeypox Virus Outbreak 2022
The multi-country outbreak, which the World Health Organization has been tracking since May, has not yet been linked to any areas where the virus is usually found.
“This is the first time we’re seeing cases across many countries at the same time in people who have not traveled to the to the endemic regions in Africa,” Lewis said in May when asked why there’s so much concern now even though the disease has been around for at least 40 years.
The current outbreak is being primarily driven by sex between men, according to one of the first peer-reviewed papers analyzing recent cases, in the New England Journal of Medicine. In New York City, the epicenter for the virus in the U.S., only one woman has been reported to have the virus, according to NYC Health. In the BMJ study, all 197 participants identified as men, and 196 identified as gay 96% reported recent sexual contact.
“The clinical presentation of these infections suggest that sexual transmission, not just close physical contact, may be helping spread the virus among this population,” Jennifer Nuzzo, an epidemiologist at Brown University, told NBC News.
This really might be the canary in the mine thats alerting to us a new disease threat that could spread to other groups, Dr. Catherine Smallwood, senior emergency officer at the WHO, told CNBC.
How Does Hiv Rash Look On Black Or Dark Skin
Theres no one-size-fits-all or one-look-fits-all, as it were when it comes to an HIV rash. It can show up in a range of colors, depending on your skins base color. On melanin-rich skin, the raised area may look purple. The small bumps on the raised area may look flesh-colored, white, red, or purple. It may also appear on your hands or feet instead of your trunk and face.
Some common HIV medications can also cause rashes, including:
- non-nucleoside reverse transcriptase inhibitors , such as efavirenz or rilpivirine
- nucleoside reverse transcriptase inhibitors , such as abacavir
- protease inhibitors, such as ritonavir and atazanavir
Based on their environment and the strength of their immune system, an individual can have more than one of these conditions at the same time. Treatment might need to address them individually or all at once.
If a rash is present on the skin, consider discussing symptoms with a healthcare provider. Theyâll assess the type of rash, consider current medications, and prescribe a treatment plan to relieve the symptoms.
Read Also: Risk Of Contracting Hiv From Needle Stick
Who Is Considered High Risk For Monkeypox Exposure
Right now, gay, bisexual and other men who have sex with men make up a large portion of confirmed monkeypox cases in the U.S. A recent CDC report on nearly 3,500 cases found that 99 percent of males with confirmed infections who also provided information on sexual activity reported male to male sexual contact. Of a subset of people with information on the sex they were assigned at birth, 99.1 percent were assigned male.
For patients with known information on race and ethnicity, around 38 percent were white and non-Hispanic, 26 percent were Black and 32 percent were Hispanic of any race. The agency notes that data are missing for a large number of cases. Thats due in part to insufficient testing.
A separate analysis of 528 confirmed MPV cases across 16 countries found that 98 percent of people with infections were gay or bisexual men, 75 percent were white and 41 percent had HIV. Sexual activity was the suspected mode of transmission for 95 percent of cases among the group.
Thats why men who have sex with men and other groups who may be at increased risk of exposure to MPV due to sexual activity including sex workers of all genders, per Washington, D.C.s guidance are being prioritized to receive a vaccine that can both protect against MPV and stop or slow disease progression in people who have already been infected depending on when they get their first dose .
What Do We Know About Mpv Itself
The monkeypox virus is part of the broader orthopox genus, which includes cowpox and the variola virus, the pathogen that causes smallpox. MPV is endemic to parts of Central and West Africa.
There are two different clades or groups of MPV: the West African clade and the Central African clade. Experts believe the milder, less lethal West African version of the virus is fueling the current global outbreak.
Deaths associated with the type of MPV thats circulating globally are rare, but three deaths attributable to monkeypox two in Spain and one in Brazil have been recorded outside of Africa as of Aug. 1. Seventy-five suspected deaths have been reported in Africa, primarily in Nigeria and Congo, where the more virulent clade is spreading, according to the Associated Press.
Vaccination after monkeypox exposure can help prevent disease, or make it less severe if you get the vaccine later than four days, Fryhofer said. For example, if you get it between four and 14 days it may reduce symptoms but may not prevent disease.
ACAM2000 is a single-dose, live replicating vaccine with a range of side effects and contraindications that can be serious, and recipients are considered fully protected after 28 days. Its not recommended for people with immune conditions like HIV, those with skin conditions like eczema or those who are pregnant or lactating. The second dose of JYNNEOS is administered four weeks after the first, and full protection kicks in two weeks after that.
Don’t Miss: Can You Get Hiv From Breast Milk
Molluscum Contagiosum Top Of Page
Molluscum contagiosum is almost as prevalent as warts. In people with AIDS, molluscum may be very widely distributed, especially on the face and neck, and much more difficult to control. Molluscum can be distinguished from warts by several features. Molluscum papules tend to be dome-shaped and to have a certain translucence. In better-developed lesions, there is often an umbilication. Histologically, the papules contain protein and viral particles known as molluscum bodies. Unlike warts, molluscum, which are caused by a pox virus, do not occur in the mouth or anorectal mucosa and have no known oncogenic potential.
Acute Hiv Rash: A Symptom Of Hiv Infection
When people are first infected with HIV, they may experience an acute, ‘flu-like’ illness called a ‘seroconversion illness,’ about 2-4 weeks after being infected. The HIV rash is a symptom of this condition.
The rash will mostly affect the upper part of the body and will probably be found on the shoulders, chest area, face, torso and palms of the hands.
Typically the rash will be flat or barely raised with small reddish dots/spots in people with light skin, and dark purple/ black in people with dark skin.
The rash is not usually itchy and it tends to disappear within 3 weeks.
Read Also: What Comes First Hiv Or Aids
Noninfectious And Nonmalignant Cutaneous Manifestations Of Hiv Infection
For xerosis, emollients and dry skin care regimens are effective. For seborrheic dermatitis, coal tar, sulfur, and salicylic acid shampoos topical corticosteroids topical tacrolimus and 2% ketoconazole cream may be effective.
For psoriasis and Reiter syndrome, ultraviolet B and psoralen with UV-A may be useful. Systemic corticosteroids, methotrexate, and cyclosporine may increase the immune suppression and must be considered only with careful monitoring. Zidovudine is also reported to be useful in the treatment of HIV-associated psoriasis.
For pruritic papular eruption, topical steroids, UV-B, PUVA, and pentoxifylline have been reported to be effective. Eosinophilic folliculitis may respond to UV-B, isotretinoin, or zidovudine treatment. For severe aphthous stomatitis, tacrolimus is reported to be effective.
Thrush In Patients With Aids:
Oral thrush is another condition that affects the oral cavity including the tongue. They appear similar to oral hairy leukoplakia, but with a thicker layer. These lesions can also be caused by fungus unlike most of the other lesions which are caused by viruses. Treatment includes oral medications and anti-fungal mouth washes. In AIDS patients, this condition often reoccurs and needs repeated treatment.
Recommended Reading: How Long Does Hiv Live Outside The Body In Sperm
Epidemiology Of Oral Lesions Of Hiv
Several studies done worldwide showed varying reports of oral lesions from 40% to 93% . The prevalence of oral lesions seen in a German study showed 39% , in South Africa, 73% was reported by Kaminu and Naidoo . Nigerian reports also showed a prevalence of 36.4% â 84% in various studies done in the different geopolitical zones. .
All studies carried out showed presence of oral lesions as a manifestation of HIV/AIDS infection.
You May Like:
What Is An Hiv Rash
Those who suffer from HIV infection , have a low immunity due to the decrease in their immune cells in the blood. When the immunity is low, a host of various organisms such as bacteria, virus, fungus and parasites can invade the body to cause diseases.
Human immunodeficiency virus itself may cause rash. Medications that are used in various infective stages can also be a cause of the rash in an HIV patient.
However, in many cases, rashes can be one among the first of the signs that appear in an HIV infected person . So it is important to be evaluated by your doctor.
Also Check: How Do I Tell My Partner I Have Hiv
Warts Associated With Aids
Skin warts associated with HIV infections are caused by HPV or human papillomavirus. The lesions appear flesh coloured small specks with cauliflower like appearance. The lesions tend to bleed when exposed to irritation especially if they are located in skin folds or mouth. These warts are prone to infection, if they are irritated or if they become open wounds. These lesions are recurrent in AIDS patients and are treated by surgical excision.
Also Read:
Are There Different Types Of Kaposi Sarcoma
There are four types of Kaposi sarcoma:
- Epidemic Kaposi sarcoma: This is the most common type of Kaposi sarcoma in the U.S. It occurs in six cases per one million people who have HIV/AIDS. Someone who has epidemic Kaposi sarcoma is likely to develop cancerous lesions throughout the body.
- Acquired Kaposi sarcoma: This sarcoma type, sometimes called transplant-related sarcoma, appears in people who have HHV-8 and are undergoing organ or bone transplant that requires medication to suppress their immune system. Acquired Kaposi sarcoma is relatively rare, affecting about one in 200 people undergoing organ or bone marrow transplant. Acquired Kaposi sarcoma usually causes skin lesions.
- Classic Kaposi sarcoma: This sarcoma type is also known as Mediterranean sarcoma because its usually diagnosed in older men of Mediterranean, Middle Eastern and Eastern European descent. People who have classic Kaposi sarcoma typically have slow-growing skin lesions that grow in size and number. Lesions might also spread to internal organs.
- Endemic Kaposi sarcoma: Also known as African sarcoma. This sarcoma type is found in people living in equatorial Africa. This sarcoma is similar to classic Kaposi sarcoma. The difference is age of diagnosis people generally develop endemic Kaposi sarcoma at a much younger age than those who have classic Kaposi sarcoma.
Don’t Miss: How Many People Have Died From Hiv Aids
What Is A Skin Lesion
A skin lesion refers to any skin area that has different characteristics from the surrounding skin, including , shape, size, and texture. Skin lesions are very common and often appear as a result of a localized damage to the skin, like sunburns or . Others, however, can be manifestations of underlying disorders, such as infections, , and autoimmune or genetic disorders. Although most skin lesions are benign and harmless, some of them can be malignant or , meaning they have the potential to evolve into .
What Causes Kaposi’s Sarcoma
Kaposi’s sarcoma is caused by a virus called the human herpesvirus 8 , also known as the Kaposi’s sarcoma-associated herpesvirus .
The virus is thought to be spread during sex, through blood or saliva, or from a mother to her baby during birth.
HHV-8 is a relatively common virus, and most people who have it will not develop Kaposi’s sarcoma.
The virus only seems to cause cancer in some people with a weakened immune system, and people who have a genetic vulnerability to the virus.
A weakened immune system allows the HHV-8 virus to multiply to high levels in the blood, increasing the chance of it causing Kaposi’s sarcoma.
The virus appears to alter the genetic instructions that control cell growth. It affects the cells that line the inside surface of blood vessels and lymphatic vessels, called endothelial cells.
The endothelial cells reproduce uncontrollably and form lumps of tissue known as tumours.
Don’t Miss: Do You Automatically Get Hiv From Someone Who Has It
Acute Hiv Infection Rash
A rash is one of the earliest symptoms of HIV. It develops during acute HIV infection, which occurs just after contracting the virus. A rash is just one of the many possible symptoms of acute HIV infection, which include:
- Fever
- Swollen tonsils or mouth ulcers
- Diarrhea
These symptoms may begin a few days after being exposed to HIV, but they typically become most noticeable about two to four weeks after infection occurs. They can last anywhere from a few days to several weeks or months.
An acute HIV infection rash and other symptoms of this stage of infection can easily be confused for other ailments or conditions, like the flu or a cold. As a result, many people dont realize that they have HIV.
If you experience an unexplained rash and you have potentially been exposed to the virus, get tested for HIV as soon as possible. Be extra cautious about having safe sex since if you do have an acute HIV infection the viral load is very high during this stage, and youre more likely to pass the virus on to your partners. If youve been taking PrEP and find out you have HIV, you need to stop taking it right away to avoid other health complications.