Listen To This Article
To hear more audio stories from publications like The New York Times, .
A woman of mixed race appears to be the third person ever to be cured of H.I.V., using a new transplant method involving umbilical cord blood that opens up the possibility of curing more people of diverse racial backgrounds than was previously possible, scientists announced on Tuesday.
Cord blood is more widely available than the adult stem cells used in the bone marrow transplants that cured the previous two patients, and it does not need to be matched as closely to the recipient. Most donors in registries are of Caucasian origin, so allowing for only a partial match has the potential to cure dozens of Americans who have both H.I.V. and cancer each year, scientists said.
The woman, who also had leukemia, received cord blood to treat her cancer. It came from a partially matched donor, instead of the typical practice of finding a bone marrow donor of similar race and ethnicity to the patients. She also received blood from a close relative to give her body temporary immune defenses while the transplant took.
Researchers presented some of the details of the new case on Tuesday at the Conference on Retroviruses and Opportunistic Infections in Denver, Colo.
The sex and racial background of the new case mark a significant step forward in developing a cure for H.I.V., the researchers said.
The Future Of Hiv Treatment
Greene points out that modern HIV medications revolutionized HIV care. When HIV first appeared in the 1980s, it was a devastating disease that killed millions of people worldwide. changed the from a death sentence to a manageable chronic disease, he says.
According to the National Institute of Allergy and Infectious Diseases, the future holds a lot of promise for HIV treatment and care. Researchers in various institutions are working on long-acting medications that wont have to be taken daily and are less toxic and costly.
The three types of treatments under study are long-acting drugs, broadly neutralizing antibodies, and therapeutic vaccines.
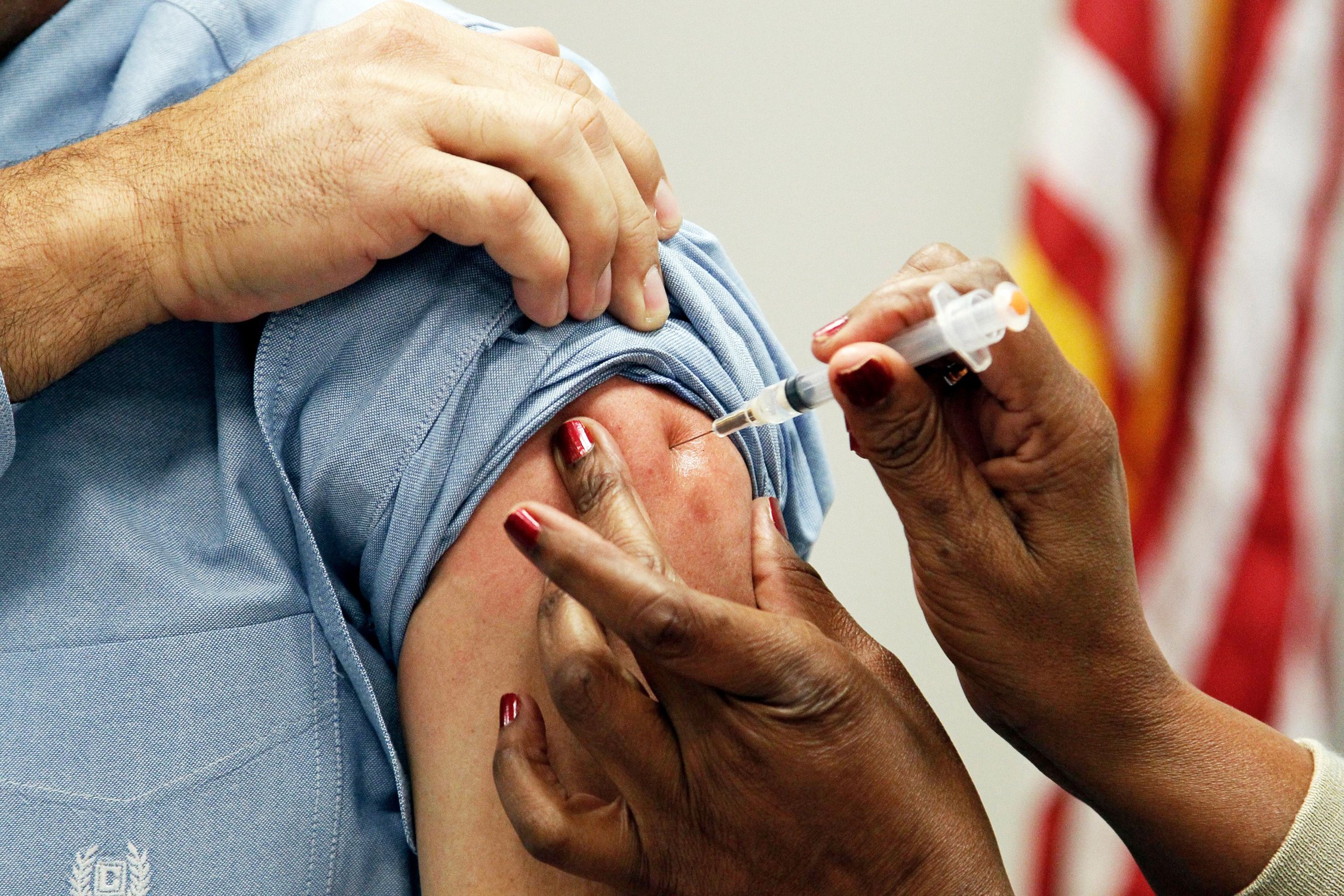
Long-acting drugs. The goal is to develop longer-acting pills as well as other ways to deliver treatment. Instead of pills, there may one day be injections, patches, and implants as options for getting treatment.
Therapeutic vaccines. This is a type of vaccine that would be given to people already living with HIV. It would stimulate the immune system to be ready to recognize and attack the HIV virus if it becomes active and keep it under control. It could end the need for further therapy and keep the virus latent or inactive in the reservoirs. Booster shots might be needed to help keep the virus in long-term remission.
Pippa Wysong
The Hiv Reservoir: How Can We Map And Measure It
This is a central topic in HIV cure research. An original hope, that HIV would eventually fade away under the pressure of long-term therapy, had been dashed in 1999 when it was established that a small percentage of HIV hides away as a ‘reservoir’ in long-lived memory cells within the immune system, establishing lifelong infection.
Although we know a lot more about the reservoir than we did and have used advanced genetic techniques to estimate the number of cells containing HIV in individuals, we still dont know which cells typically form part of the reservoir, including cells that are hard to access such as those in the nervous system. It may even look different in different parts of the world, depending on the predominant HIV strain and different host characteristics.
We dont have an easy way to count the number of cells containing HIV DNA in individuals. We do know it keeps itself going by cell division, so that new clones of the same HIV DNA persist when old cells die off but we dont know what prompts cells to divide and whether division can be turned off. We do know that a lot of HIV is defective and cant give rise to new viruses, but we dont know whether pure chance or specific factors push HIV into becoming defective or ending up in locations where it cant activate. We dont know whether and to what extent defective HIV DNA still gives rise to viral proteins that could cause inflammatory states or, conversely, sustain a useful immune reaction against HIV.
Recommended Reading: How Are Drugs For Hiv Patients Administered
How Far Away Is A Cure
With the reports of people experiencing cure in the news and the advances in research, it might sound like a cure is just around the corner, but its not so straightforward. HIV cure is a hugely complex puzzle. Whether its complete eradication or a functional cure, a cure for HIV is at least several years away, maybe longer. But there is hope, and new efforts are underway that may speed things up.
One is the appearance of big collaborations between various research centers, says Greene, where laboratories working on cures share their findings. Collaborations can speed up research.
A key program for this is the Martin Delaney Collaboratories for HIV Cure Research, the flagship National Institutes of Health program on HIV cure research. It fosters collaborations between researchers studying HIV and working on potential strategies for a cure. Collaborations bring together researchers from academia, industry, government, and communities.
An example of one such collaboration is the HOPE Collaboratory, which consists of a diverse, multidisciplinary, international group of HIV researchers from around the world. People in this particular collaboration are working on the block-and-lock approach.
Scientists Have Possibly Cured Hiv In A Woman For The First Time
An American research team reported that it has possibly cured HIV in a woman for the first time. Building on past successes, as well as failures, in the HIV-cure research field, these scientists used a cutting-edge stem cell transplant method that they expect will expand the pool of people who could receive similar treatment to several dozen annually.
Their patient stepped into a rarified club that includes three men whom scientists have cured, or very likely cured, of HIV. Researchers also know of two women whose own immune systems have, quite extraordinarily, apparently vanquished the virus.
Carl Dieffenbach, director of the Division of AIDS at the National Institute of Allergy and Infectious Diseases, one of multiple divisions of the National Institutes of Health that funds the research network behind the new case study, told NBC News that the accumulation of repeated apparent triumphs in curing HIV continues to provide hope.
Its important that there continues to be success along this line, he said.
It is unethical, experts stress, to attempt an HIV cure through a stem cell transplant a toxic, sometimes fatal procedure in anyone who does not have a potentially fatal cancer or other condition that already makes them a candidate for such risky treatment.
Don’t Miss: Can You Die Of Aids
Fourth Person ‘cured’ Of Hiv But Is A Less Risky Cure In Sight
Issued on: 27/07/2022 – 16:02
Paris AIDS researchers announced on Wednesday that a fourth person has been “cured” of HIV, but the dangerous procedure for patients also battling cancer may be little comfort for the tens of millions living with the virus worldwide.
The 66-year-old man, named the “City of Hope” patient after the Californian centre where he was treated, was declared in remission in the lead up to the International AIDS Conference, which begins in Montreal, Canada on Friday.
He is the second person to be announced cured this year, after researchers said in February that a US woman dubbed the New York patient had also gone into remission.
The City of Hope patient, like the Berlin and London patients before him, achieved lasting remission from the virus after a bone marrow transplant to treat cancer.
Another man, the Duesseldorf patient, has also previously been said to have reached remission, potentially bringing the number cured to five.
Dickter is the lead author of research on the patient which was announced at a pre-conference in Montreal but has not been peer reviewed.
‘i Never Thought I Would See The Day’
Human immunodeficiency virus damages the body’s immune system. This can lead to Aids and the body struggling to fight off infection.
In a statement, the man said: “When I was diagnosed with HIV in 1988, like many others, I thought it was a death sentence.
“I never thought I would live to see the day that I no longer have HIV.”
However, he was given the therapy not for his HIV, but because he developed the blood cancer leukaemia at the age of 63.
The man’s medical team decided he needed a bone marrow transplant to replace his cancerous blood cells. By coincidence, the donor was resistant to HIV.
The virus gets into our body’s white blood cells by using a microscopic doorway – a protein called CCR5.
However, some people, including the donor, have CCR5 mutations that bolt the door shut and keep out HIV.
You May Like: Can Hiv Cause Weight Gain
The Role Of Memory Cd4 T
The key player in AIDS pathogenesis and cure is the memory CD4 T-cells. These cells are predominantly quiescent but are capable of intermittent self-renewal and long-term survival, meaning that these cells have stem cell like properties of HSPCs at the cell-cycle control, self-renewal, asymmetric division, and differentiation into effector cells . Let us briefly view the mechanisms, which memory CD4 T-cells employ to play the pivotal roles in eradication of HIV and cure of AIDS.
Upon naïve CD4 T-cells meeting a pathogen, in this case, the HIV, these cells differentiate into antigen specific effector cells. Some of them die due to the viral infection or their biological destinies, but some survive and become memory cells and further develop into secondary effector cells. When encountering HIV again, these antigen specific T-memory cells, in this case HIV specific, replicate and differentiate into the secondary effector cells . The HIV specific effector cells, specifically memory CD4 T-cells, play decisive roles not only in anti-HIV immunity but also in AIDS pathogenesis, since these cells govern functions of both CD8-cells and B-cells, regulate both cellular and humoral immunities, thereby determine the prognosis of AIDS .
What Is An Hiv Cure
There are two different visions of a potential HIV cure: treatment-free remission and viral eradication.
Treatment-free remission means the virus is controlled without the need for ART drugs, which a person has to take every day for life. Millions of people who have HIV canât afford ART, so other treatments are needed. This idea of an HIV cure is also called a functional cure.
Treatment-free remission means that youâd:
- Live a healthy life thatâs of normal length
- Not have to take ART or any other HIV-related drugs to keep the virus under control
- Not be able to pass on HIV to others
Many therapies are being studied as a way to control HIV without the need for daily ART. These include antibody therapies and therapeutic vaccines. They donât prevent infection, but stimulate your own immune system to fight it.
Viral eradication is another way of looking at a potential cure. Itâs also known as a sterilizing cure. Scientists believe it would take a two-part treatment to wipe out HIV in a personâs body. The first part would involve drugs that make the cells in the HIV reservoir multiply and express proteins that are like a signal to your immune system. The second part would include drugs that detect those protein signals, then seek out and kill the virus.
Other types of drugs that may be able to seek out and kill HIV include histone deacetylase inhibitors, protein kinase activators, latency securing agents, and immunotoxins. These drugs may be used in combination.
Read Also: How Can You Tell If Someone Has Hiv
The City Of Hope Patient
The latest case involves a 66-year-old white man who was diagnosed with HIV in 1988. At one point, his CD4 count fell so low that he was diagnosed with AIDS. He started ART when it became available in the mid-1990s. In 2018, he was diagnosed with acute myelogenous leukaemia.
chemotherapy
The use of drugs to treat an illness, especially cancer.
In early 2019, at age 63, he received a stem cell transplant from an unrelated donor with a double CCR5-delta-32 mutation, which deletes the receptors most strains of HIV use to enter cells. Before the procedure, he underwent reduced-intensity conditioning chemotherapy designed for older and less fit patients, and he developed only mild graft-versus-host disease, a condition that occurs when donor immune cells attack the recipients body.
Tests showed that the man achieved 100% chimerism, meaning all his immune cells originated from the donor, Dickter reported. He continued ART for two years after the transplant. At that point, with a stable undetectable viral load, he and his doctors decided to try a carefully monitored treatment interruption.
More than three years after the transplant and over 17 months after stopping antiretrovirals he has no evidence of HIV RNA viral load rebound and no detectable HIV DNA in peripheral blood cells, a marker of the latent viral reservoir. Gut tissue biopsies also found no evidence of replication-competent virus.
Prevent Hiv After An Exposure
If you believe you have been exposed to HIV, either through condomless sex or other high-risk activities, you can take a 28-day course of HIV drugs to potentially avert the infection.
Called post-exposure prophylaxis , the strategy works best if started soon after exposure to the virus. Research has shown that PEP can reduce the risk of HIV by up to 81% if started within 72 hours. The earlier you start treatment, the better.
Don’t Miss: What System Does Hiv Attack
Does Hiv Treatment Cause Side Effects
Like most medicines, HIV medicines can cause side effects in some people. However, not everyone experiences them. The HIV medicines used today have fewer side effects and are less severe than in the past. Side effects can differ for each type of HIV medicine and from person to person. Some side effects can occur once you start a medicine and may only last a few days or weeks. Other side effects can start later and last longer.
Side effects of HIV medicine most commonly reported include:
- Nausea and vomiting
Hiv Hides In The Body
Scientists had hoped giving strong treatment medications so soon after birth would get rid of the virus or prevent it from spreading and doing damage.
The fact that the HIV virus eventually turned up in the âMississippi babyâ isn’t unexpected, says Robert Siliciano, MD, PhD, professor of medicine in the infectious diseases department at Johns Hopkins University School of Medicine. It supports the theory that HIV cells stay in the body, just out of view in a hidden “reservoir.”
“Curing HIV infection is going to require strategies to eliminate this reservoir,” he says.
You May Like: What Is Aids Look Like
Can Natural Herbal Or Alternative Medicines Cure Hiv
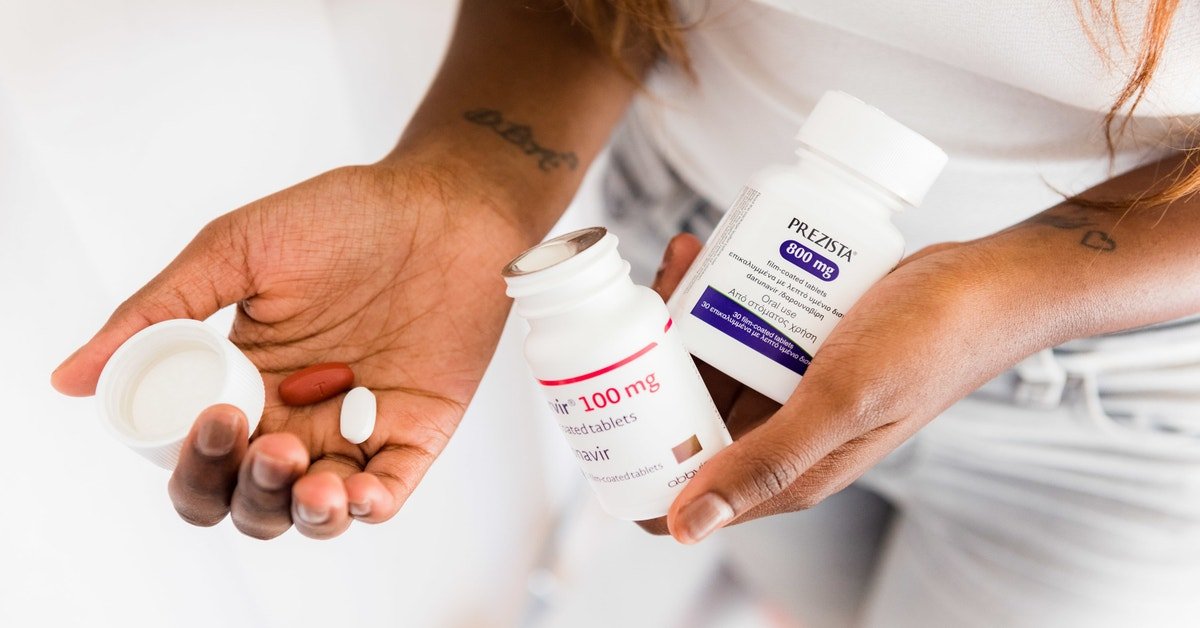
No. There is no natural, herbal or alternative cure for HIV. Antiretroviral treatment is the only medication that can control HIV. Taking herbal medicines can be dangerous as they will not protect your immune system from the damage caused by HIV. Some herbal medicines can also make antiretroviral treatment less effective.
Is There A More Gentle Way To Modify T
As mentioned earlier, transplants of the entire immune system are not a cure technique ever likely to be performed on more than a few people. But there may be gentler ways of modifying peoples immune systems so their T-cells are less responsive to HIV and ongoing replication ceases, thereby depleting the reservoir. Modifying peoples T-cells outside the body and then reintroducing them is not a new technique, first tried in 2011. But it has proved difficult to maintain the population of modified T-cells.
In 2019 Dr Pablo Tebas of the University of Pennsylvania was able to delay viral rebound in some of a group of trial participants given T-cells genetically altered outside the body to lack the CCR5 co-receptor. He added in cyclophosphamide, an immune modulator that reduced the number of native unmodified T-cells in recipients so the modified ones had more chance.
Tebas has since conducted a third round of studies, dropping the cyclophosphamide but adding in CAR T-cells sensitised to HIV.
The problem with the HLA system is that it is not foolproof. Sometimes it starts looking like nonself to the immune system, causing autoimmune disease. Sometimes viruses mutate in such a way that they no longer get flagged HIV can do this. Anything inside the nucleus such as proviral DNA is not displayed. And sometimes HLA downregulates, meaning that if the cells sense nothing wrong, they may cease displaying HLA molecules.
Don’t Miss: When Will Hiv Be Cured
Alternative Therapies And Natural Treatments
There is a range of natural treatments a person can try to ease HIV symptoms and medication side effects and to make them feel better, overall.
Many people do experience positive results from using these therapies. However, there is little research into their safety and effectiveness, and they are not a substitute for medical treatment.
Alternative treatments include:
A Unique Case: 15 Years With Absolute Control Over Replication Of The Virus
The study presented at the 2022 AIDS Conference describes the immune mechanisms of a female post-treatment controller that confer complete control of HIV replication over more than 15 years. The patient was diagnosed in the acute phase of HIV infection and was enrolled in a clinical trial with antiretroviral treatment for 9 months and different immune-modulating interventions with ciclosporin A, an immunosuppressant agent. The patient did not have genetic factors associated with control of HIV, she was not an elite controller of the disease, and furthermore, she presented severe acute-phase infection, something that is uncommon in post-treatment controllers“, said Josep M. Miró.
Furthermore, it has been shown that the patient is not infected with defective viruses, i.e., her virus was viable because it was possible to isolate it and culture it in the laboratory. Over these years, we have found a pronounced and gradual drop in the number of viruses in the reservoir, which suggests control by the immune response“, explained Sonsoles Sánchez-Palomino.
The researchers saw that the patients blood cells were highly resistant to infection by the HIV virus in in vitro cultures, but her purified CD4+ T cells were susceptible to infection to HIV. This suggests that other populations of blood cells were blocking the infection and may contribute to controlling the HIV.
Don’t Miss: When Should I Get Tested For Hiv