Mortality In The Second And Third Years Of Hiv Treatment
There were dramatic declines in mortality rate in the second and third years of HIV treatment over time from 1996 to 2010. These declines were consistent across North America and Europe, different age groups, and different CD4 cell counts when ART was started. However, people who inject drugs had higher mortality rates than other people.
Improvements in survival during the second and third years of ART are probably caused by increased viral suppression, declining rates of viral failure, and increasing treatment options, the authors said. Simpler regimens might have contributed to improvements in both short-term and long-term adherence to ART.
How Long Can You Live With Hiv Very
Roz Woodward for Photodisc via Thinkstock
Just this past week, I met John , a 50-year-old long-term survivor with HIV, in our clinic in Denver, Colorado. He was on a well-tolerated treatment regimen, had an undetectable viral load and normal CD4 count. He asked me about new studies on HIV treatments, and about both his projected quality and quantity of life.
I told him that, on average, life expectancy for people living with HIV — provided they get tested, find their way into a care center, initiate antiretroviral treatment and continue taking that treatment regularly — is similar to people who don’t have HIV infection.
He gave me a suspicious look. “Are you sure?” he asked.
Gains And Losses In Life Years
Factors that influence life expectancy are either static or dynamic .
Static factors, like race or sexual orientation, influence life expectancy because they are ones people are often unable to escape. For example, high levels of poverty in Black communities combined with a lack of access to health care and high levels of HIV stigma take back many of the gains seen in White communities.
Dynamic factors, by comparison, have a strong cause-and-effect relation to survival times. For instance, treatment adherence is directly related to disease progression. The less adherence is maintained, the greater the risk of drug resistance and treatment failure. With each failure, a person loses more and more treatment options.
When looking at both static and dynamic risk factors, we can begin to identify where an individual can gain or lose life-years without even knowing it. Among them:
Recommended Reading: Who Was The First Person To Get Hiv
People Are Living Longer Thanks To Treatment
According to the new research, which retrospectively analysed data from 88,504 patients starting treatment over three-year periods between 1996 and 2010, life expectancy rose by nine years for woman, and ten years for men. This means that a 20 year-old person living with HIV in these regions, starting treatment after 2008, can now expect to live to 78.
This figure is very much reflective of the improvements in antiretroviral agents, along with the expanded access of effective HIV treatment and care programmes. Antiretroviral drugs are less toxic, with fewer side-effects. Screening and managing drug resistance is easier, and we now have more options for switching drugs in the event that resistance occurs. The onset of opportunistic infections and screening for and managing other related co-morbidities is better integrated into programming meaning people with HIV are experiencing better health outcomes.
Hiv Life Expectancy ‘near Normal’ Thanks To New Drugs
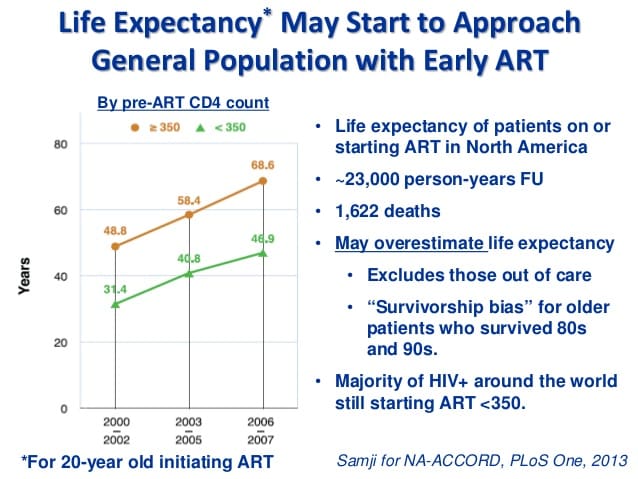
Young people on the latest HIV drugs now have near-normal life expectancy because of improvements in treatments, a study in The Lancet suggests.
Twenty-year-olds who started antiretroviral therapy in 2010 are projected to live 10 years longer than those first using it in 1996, it found.
Doctors say that starting treatment early is crucial to achieve a long and healthy life.
Charities say there are still too many people unaware they have the virus.
This is particularly true in the developing world, where the majority of HIV deaths occur because access to drugs is limited.
Read Also: How Can Hiv Be Contracted
The Global Distribution Of Deaths From Hiv/aids
In some countries HIV/AIDS is the cause of more than a quarter of all deaths
Globally, 1.7% of deaths were caused by HIV/AIDS in 2017.
This share is high, but masks the wide variations in the toll of HIV/AIDS across the world. In some countries, this share was much higher.In the interactive map we see the share of deaths which resulted from HIV/AIDS across the world. Across most regions the share was low: across Europe, for example, it accounted for less than 0.1% of deaths.
But across some countries focused primarily in Southern Sub-Saharan Africa the share is very high. More than 1-in-4 of deaths in South Africa and Botswana were caused by HIV/AIDS in 2017. The share was also very high across Mozambique Namibia Zambia Kenya and Congo .
Death rates are high across Sub-Saharan Africa
The large health burden of HIV/AIDS across Sub-Saharan Africa is also reflected in death rates. Death rates measure the number of deaths from HIV/AIDS per 100,000 individuals in a country or region.
In the interactive map we see the distribution of death rates across the world. Most countries have a rate of less than 10 deaths per 100,000 often much lower, below 5 per 100,000. Across Europe the death rate is less than one per 100,000.
Across Sub-Saharan Africa the rates are much higher. Most countries in the South of the region had rates greater than 100 per 100,000. In South Africa and Mozambique, it was over 200 per 100,000.
Us Hiv Life Expectancy: What The Numbers Say
The Centers for Disease Control and Prevention estimates that average life expectancy for a person born within the U.S. in 2012 is about 79 years. It’s a little more for women and a little less for men .
For people who weren’t born yesterday, the numbers actually look better: Taking into consideration that there are some causes of death that mostly affect younger people, a person who reaches age 65 can currently be expected to live an additional 19 years , on average.
That’s for the U.S. population as a whole. What about for people with HIV in particular?
In a recent scientific presentation looking at people who received care in the massive U.S. Kaiser Permanente health system between 1996 and 2011, we learned how incredibly far we’ve come in a very short time in treating HIV. The study showed that additional life expectancy for a 20-year-old person with HIV was only 19 years back in 1996, meaning a total lifespan of only 39 years on average. By 2011, additional life expectancy had increased to 53 years, meaning a total lifespan of 73 years on average. By comparison, the study found that a 20-year-old person without HIV lived an additional 65 years, for a total of 85. So, in this study, overall, HIV-positive folks were found to live about eight years less than HIV-negative folks as of 2011.
Also Check: Can I Have Hiv Symptoms After 1 Week
What Is Life Expectancy
LE is an important indicator of health that is used widely by governments, healthcare agencies, and insurance companies to monitor trends in survival over time, and to determine resource allocation . Formally, LE indicates the average number of years that a person would be expected to survive beyond a given age. That given age would usually be birth however, in the context of HIV, the given age may be difficult to interpret as, in most cases, individuals are not born with HIV but acquire it at some point during their life. Thus, LE is commonly quoted from a specific given age or after some specific event, such as HIV diagnosis . Of note, LE at a particular age is not the same as LE at birth minus that age, as LE at a particular age is calculated after conditioning on the fact that the individual has already survived to that age.
Life Expectancy Outside Of High
However, in low- and middle-income countries, the life expectancy picture isnt as clear. Whilst there have been fewer studies undertaken, theres certainly been a marked decline in deaths from HIV.
In South Africa, the country with the largest population of people living with HIV, a recent study also showed life expectancy to be near normal for those people who started treatment early. However, many health system and structural challenges will have to be overcome for every person living with HIV in South Africa, and other developing economies, to experience the positive health outcomes related to starting treatment early.
Accessing treatment and staying on it for life present a very different reality to those people living with HIV in developed countries.
Read Also: Does Hiv Cause Hair Loss
Can We Improve Le Further
Late HIV diagnosis remains extremely common in many countries , and has been reported to be a major risk factor for mortality . In Brazil, it was estimated that 95.5% of deaths occurring in the first year after diagnosis were attributable to late diagnosis study investigators estimated that averting late diagnosis would have reduced the AIDS mortality rate 2003 to 2006 by 39.5%, a similar reduction to that produced by cART. In the UK, earlier diagnosis would have reduced short-term mortality by 84% in MSM and by 56% in those infected heterosexually . Using the HIV Synthesis model, a stochastic computer simulation model of HIV progression, Nakagawa showed that LE from birth was 71.5 years, with 10.5 years lost to HIV infection, in a scenario in which diagnosis occurred at a late stage of HIV infection , but under a scenario of earlier diagnosis , LE from birth was 75.0 years, with only 7.0 years lost, on average, due to HIV. Thus, earlier diagnosis of HIV might go some way to improve LE further.
How Life Expectancy Has Improved
Antiretroviral Therapy was not yet readily available in 1996. Thats changed over the past two decades. As a result of there being easier access ART, it revolutionized HIV treatment. By preventing the virus from reproducing, ART is able to lower the viral load in the bloodstream. When successful, the viral load is so low that the virus is undetectable. HIV is still there. And it can still be spread to someone else. But there arent any symptoms.
Treatment is more effective across the board. Over half of those eligible for treatment are now receiving it. Also, Linkage to Care numbers continues to increase. The necessary work is being done.
In addition to being more effective, HIV treatment is now simpler, too. Fewer pills are needed. And theres no longer a complex schedule to follow. A lot of patients can now take one pill a day and be fine. They work for a longer period of time and have fewer side-effects. Its less likely for a patient to have to switch medications periodically.
Recommended Reading: How Does Hiv Aids Spread
Data Extraction And Management
The following characteristics were extracted from the research articles matching the inclusion criteria, and entered into a database by a single reviewer : study characteristics , characteristics of participants , life expectancy and standard error or 95% confidence intervals around life expectancy estimates at specific ages both overall and stratified by gender. Income region was classified according to World Bank Income categories, as low/middle income or high income .
Comorbidities And Healthy Aging
Because modern-day HIV medications are highly effective and well-tolerated, interventions that improve the life expectancies of people living with HIV will need to address other health conditions that may affect people living with HIV at a disproportionate rate or more severely.
Improving the health of people growing older with HIV is a critical priority, said Harris, Rabkin and El-Sadr, in an editorial published in AIDS. Older adults living with HIV may experience more severe side effects of antiretroviral medications, higher risk of kidney disease, declines in bone mineral density, peripheral neuropathy and cardiovascular disease. An estimated 6.9 million people living with HIV will be over age 50 by the year 2020.
The greying of the epidemic raises important questions regarding understanding the effect of aging on people living with HIV, the effect of HIV infection on the aging process, and optimal approaches to HIV prevention among older adults, said Harris and colleagues.
Harris, T. G., Rabkin, M. and El-Sadrr, W. M. Achieving the fourth 90: healthy aging for people living with HIV. AIDS, 2018.
Don’t Miss: What Are The Signs And Symptoms Of Hiv
Average Life Expectancy Togo
One important indicator of the status of health in Togo is the overall average life expectancy in Togo. The latest WHO information shows that in 2009 the average life expectation in Togo was 59. The average life expectancy for woman was 61, while men had a life expectancy of 57 in Togo. The average life expectancy in Africa region was 54 years. This is 5 years lower than the average life expectancy in Togo. In 2000 the average life expectancy in Togo was 56 years, compared to 50 years in Africa.
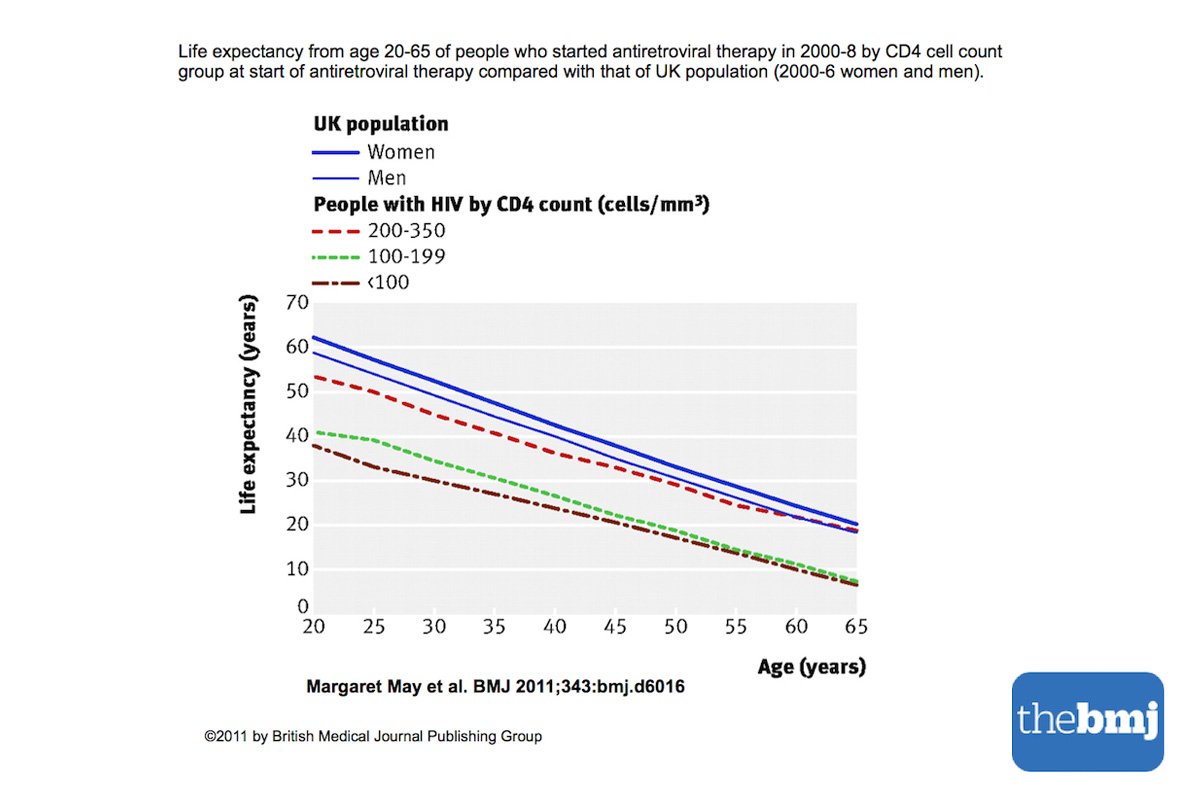
How Did The Researchers Interpret The Results
The researchers conclude that life expectancy for people treated for HIV infection increased by over 15 years between 1996 and 2008, but is still about 13 years less than the general population. However, they predict we should expect further improvements for patients starting antiretroviral therapy now with improved modern drugs and new guidelines recommending earlier treatment.
Also Check: How Does The Immune System Fight Hiv
Mortality In The First Year Of Hiv Treatment
A total of 2,106 people died in the first year of starting ART and 2,302 people died during the 15,813 person-years included in the study.
People starting HIV treatment in later years were much less likely to die in the first year of treatment than people starting HIV treatment in earlier years . The increased availability of more effective and better tolerated HIV medications over time is likely to have contributed to this disparity, the authors said. Mortality in the first year of HIV treatment was strongly influenced by people starting treatment very late in their HIV infection .
Factors That Reduce Life Expectancy
But there are challenges that can take back many of those gains. From an individual perspective, longevity is subject to numerous factors that can either increase or decrease life expectancy in a person with HIV. These factors range from things we can control to things we can’t .
Moreover, HIV is really only part of the long-term concern. Even for those able to maintain an undetectable viral load, the risk of non-HIV-associated diseases, like cancer and heart disease, is far greater than in the general population and can occur anywhere from 10 to 15 years earlier.
So profound are these concerns that a person with HIV is far more likely to die prematurely of a non-HIV-related illness than an HIV-related one.
Recommended Reading: How Long Does It Take For Hiv Symptoms To Develop
What You Can Do
The most important things you can do to protect your health as you live with HIV are to take your ART as your doctor prescribes and to see your health care team regularly.
There are several other things you can do to stay healthy and keep your immune system working well:
- Eat healthy foods. A diet with plenty of nutrients will keep your energy up and help your immune system fight infections. It also helps your body absorb your medications.
- Get regular exercise: A fitness program will help you stay strong and will give you endurance. It also will give your mental health a boost and help you to manage stress.
- Donât smoke. If you have HIV, smoking doesnât just raise your chances of cancer, heart disease, stroke, and early death. It also makes you even more prone to mouth sores, which are a common problem for people with the virus. Worst of all, your ART doesnât work as well when you smoke, so make it a top goal to be smoke-free.
Conference on Retroviruses and Opportunistic Infections: âIncreased overall life expectancy but not comorbidity-free years for people with HIV.â
AIDSinfo: âHIV and Opportunistic Infections, Coinfections, and Conditions,â âSide Effects of HIV Medicines,” âHIV and Osteoporosis.”
“Jama: âComorbidities in Persons With HIV: The Lingering Challenge.â
Health and Quality of Life Outcomes: âMeasuring quality of life among people living with HIV: a systematic review of reviews.â
CDC: âHealthy Living with HIV.â
Reasons For The Gaps:
Women
The overall life expectancy of HIV-positive women in this study was less than that of MSM and HIV-negative women. The researchers suggested several possibilities for their findings. It is possible that women may be accessing HIV-related care at later stages of HIV disease than men. The study enrolled large numbers of women who had a history of injecting street drugs . In general, people who inject street drugs have worse survival, regardless of HIV status, than non-IDUs. Women in this study may have had less education, lower incomes and more difficulty interacting with the health care system and may have experienced more social stigma and isolation than HIV-positive MSM in the study.
Unmentioned by the researchers are the many roles that women have thrust upon them, including caring for children and other family members, running a household and working outside the home. Due to these multiple roles, women sometimes are forced to prioritize the care of others and have insufficient time to care for themselves. All of these factors could have impacted the overall health and survival of women in this study.
People who inject street drugs
The research team suggested that the following factors likely played a role in the poorer life expectancy of people who inject street drugs in this study:
- having co-morbidities such as hepatitis C virus
- difficulty taking ART every day exactly as directed
- the destabilizing effect of active drug use
- unstable housing
- low income
Also Check: What Is Hiv 4th Generation
Despite Medical Advances People With Hiv Still Live Shorter Sicker Lives
HealthDay Reporter
THURSDAY, June 18, 2020 — HIV may not be the death sentence it was 20 or 30 years ago, but people who are HIV-positive still face much shorter lives than other adults — even if they’re treated with medications that make the virus undetectable.
A new study reports that people who were HIV-positive at age 21 had an average life expectancy of 56 years — nine years fewer than their virus-free peers.
The likely reason: a weaker immune system and a greater risk for other chronic health issues, even when HIV is kept in check.
“Our findings suggest that people with HIV who initiate treatment early are approaching the same lifespan as people without HIV, but that we need to be paying closer attention to preventing comorbidities among people with HIV,” said lead author Dr. Julia Marcus, an assistant professor at Harvard Medical School in Boston.
When antiretroviral therapy — or HAART — was introduced for HIV treatment in 1996, it was a game-changer.
Taken daily, the medications can suppress the virus to undetectable levels, keeping patients healthy and eliminating the risk of sexual transmission. The U.S. Department of Health and Human Services recommends starting HAART immediately after an HIV diagnosis.
To find out, they reviewed disease and death histories drawn from Kaiser Permanente records for nearly 430,000 people between 2000 and 2016. About 39,000 were HIV-positive, and nearly nine in 10 of these patients were male .
JAMA Network Open