History Of Hiv And Aids Overview
KEY POINTS:
The history of the HIV and AIDS epidemic began in illness, fear and death as the world faced a new and unknown virus. However, scientific advances, such as the development of antiretroviral drugs, have enabled people with access to treatment to live long and healthy lives with HIV.
Here, we go through the key historical moments that have defined the HIV epidemic over the past 30 years.
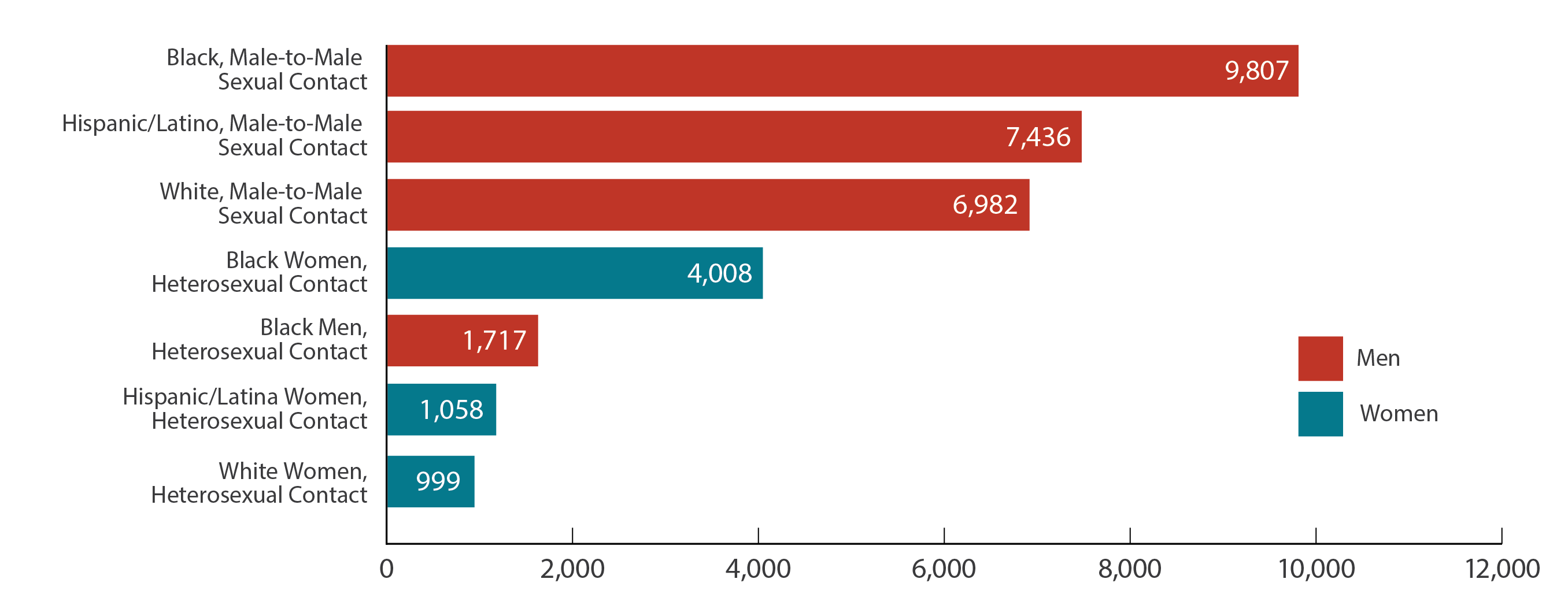
New Hiv Diagnoses Among Gay And Bisexual Men In The Us And Dependent Areas By Race/ethnicity 2019
* Black refers to people having origins in any of the Black racial groups of Africa. African American is a term often used for people of African descent with ancestry in North America. Hispanic/Latino people can be of any race.
From 2015 to 2019, HIV diagnoses decreased 9% among gay and bisexual men overall. But trends varied for different groups of gay and bisexual men.
Hiv Statistics By State In The Us
In the United States, diagnoses are highest in Florida and California.
The table below is given as a reference to understand better where HIV diagnoses are most common in the United States. In regions like these, local governments and NGOs must take the necessary action to help reduce the number of infections. Yearly deaths are also more common in these regions, due to the higher HIV transmission rates.
| State |
Also Check: Nba Youngboy Stds
Impact Across The Country
- Although HIV has been reported in all 50 states, the District of Columbia, and U.S. dependencies, the impact of the epidemic is not uniformly distributed.
- Ten states accounted for about two-thirds of HIV diagnoses among adults and adolescents in 2019 .31 Regionally, the South accounted for more than half of HIV diagnoses in 2019.32
- Rates of HIV diagnoses per 100,000 provide a different measure of the epidemicâs impact, since they reflect the concentration of diagnoses after accounting for differences in population size across states. The District of Columbia has the highest rate in the nation, compared to states, nearly 3 times the national rate and Georgia was the state with highest rate , twice that of the national rate.33,34 Nine of the top 10 states by rate are in the South.35
- New HIV diagnoses are concentrated primarily in large U.S. metropolitan areas , with Miami, Orlando, and Atlanta topping the list of the areas most heavily burdened.36
| Table 1: Top Ten States/Areas by Number and Rate of New HIV Diagnoses , 2019 | |
| State | |
| U.S. Rate | 13.2 |
| CDC. HIV Surveillance Report, Diagnoses of HIV Infection in the United States and Dependent Areas, 2019 vol. 32. May 2021. |
Canada’s Progress On Meeting The 90
In Canada at the end of 2018, an estimated 62, 050 people were living with HIV . Among those living with HIV, an estimated 87% were diagnosed. Of those diagnosed, 85% were estimated to be on treatment and Canada has achieved the third 90 target with an estimated 94% of persons on treatment having a suppressed viral load .
Canada’s 2018 90-90-90 estimates lie within the range reported by other developed countries such as the United States of America, Germany, Australia, and Finland.
Figure 2. Estimated number and percentage of persons living with HIV, diagnosed, on treatment, and virally suppressed in Canada at the end of 2018 .
This graph shows the estimated number of persons in Canada at the end of 2018 who were living with HIV, diagnosed, on treatment, and virally supressed. The horizontal axis shows the four components that were estimated . The vertical axis shows the estimated number of persons, with the low and high ranges associated with each component.
This graph also shows the point estimate and plausible range associated with each of the three 90-90-90 targets. The first target is the percent of persons living with HIV who are diagnosed. The second target is the percent of persons diagnosed who are on treatment. The third target is the percent of persons on treatment who are virally suppressed.
| Estimate |
|---|
| 43,540 47,840 | 42,240 44,070 |
Read Also: How Long Does It Take To Become Undetectable Hiv
New Hiv Infection Rates
New HIV infection rates have dropped over the years. The world has seen a 52% reduction in new HIV infections since the epidemic peaked in 1997. In 1997, 3 million people reported new HIV infections, compared with only 2.1 million in 2010 and 1.5 million in 2020.
This is because people in resource-poor countries now have significantly improved access to HIV treatments. Preventing vertical transmission of HIV, which refers to when the infection passes from a birthing parent to their fetus, has also contributed to lowering transmission rates. Additionally, the medical community has added new HIV prevention tools and methods.
However, the unequal distribution of HIV treatment and prevention strategies still leaves many vulnerable populations behind. Important barriers to improving access to care include stigma, discrimination, social inequities, and exclusion.
Before the COVID-19 pandemic, many people with HIV or at risk of HIV still did not have access to prevention, care, and treatment. The pandemic caused a greater disturbance in the distribution of health services in many countries. Some countries report a 75% disruption of HIV services.
According to UNAIDS, the Joint United Nations Programme on HIV/AIDS, the benefits of providing HIV services outweigh the risk of dying from COVID-19.
HIV spreads through contact with bodily fluids from people who have the virus. Bodily fluids that carry HIV include:
- blood
It is not possible to contract HIV through:
What Should I Do If I Think Im At Risk For Hiv
If you think youre at risk for getting HIV, or that you might already have HIV, get tested and learn about the effective HIV prevention and treatment options available today.
Testing is the only way to know for sure if you have HIV. Find out whether testing is recommended for you.
Many HIV tests are now quick, free, and painless. Ask your health care provider for an HIV test or use the HIV Services Locator to find a testing site near you. You can also buy an FDA-approved home testing kit at a pharmacy or online.
Knowing your HIV status gives you powerful information to help you take steps to keep you and your partner healthy:
- If you test positive, you can start HIV treatment to stay healthy and prevent transmitting HIV to others.
- If you test negative, you can use HIV prevention tools to reduce your risk of getting HIV in the future.
You May Like: How Long Does Hiv Stay Dormant
Hiv/aids In The United States
| Rates of HIV Diagnoses in the US, 2017 |
| New HIV Infections by Race and Transmission Group |
| HIV Diagnosis Trends in the U.S. and Dependent Areas, 20122016 |
| The estimated number of U.S. HIV/AIDS Cases, in 2007 by transmission category |
The AIDS epidemic, caused by HIV , found its way to the United States as early as 1960, but was first noticed after doctors discovered clusters of Kaposi’s sarcoma and pneumocystis pneumonia in homosexual men in Los Angeles, New York City, and San Francisco in 1981. Treatment of HIV/AIDS is primarily via a “drug cocktail” of antiretroviral drugs, and education programs to help people avoid infection.
Initially, infected foreign nationals were turned back at the U.S. border to help prevent additional infections. The number of U.S. deaths from AIDS has declined sharply since the early years of the disease’s presentation domestically. In the United States in 2016, 1.1 million people aged over 13 lived with an HIV infection, of whom 14% were unaware of their infection.Gay and bisexual men, African Americans, and Latinos remain disproportionately affected by HIV/AIDS in the U.S.
Are Some Regions Of The United States More Impacted By Hiv Than Others
Yes. HIV is largely an urban disease, with most cases occurring in metropolitan areas with 500,000 or more people. The South has the highest number of people living with HIV, but if population size is taken into account, the Northeast has the highest rate of people living with HIV.
*Rates per 100,000 people.
Recommended Reading: Hiv Causes Hair Loss
Impact On Gay And Bisexual Men
- While estimates show that gay and bisexual men comprise only about 2% of the U.S. population, male-to-male sexual contact accounts for most new HIV infections and most people living with HIV .58
- Annual new infections among gay and bisexual men declined overall between 2015 and 2019 but remained stable among Black and Latino gay and bisexual men.59
- Blacks gay and bisexual men accounted for the largest number of new diagnoses among this group in 2019, followed by Latino gay and bisexual men .60 Additionally, according to a recent study, Black gay and bisexual men were found to be at a much higher risk of being diagnosed with HIV during their lifetimes compared with Latino and white gay and bisexual men.61 Young Black gay and bisexual men are at particular risk â Black gay and bisexual men ages 20-29 accounted for 51% of new diagnoses among that age group and 13% of all diagnoses.62
Hiv Statistics By State
Human immunodeficiency virus, or HIV, is a virus that weakens a persons immune system by attacking cells that fight off infection, specifically a persons CD4 cells. HIV is spread through body fluids such as blood. If HIV goes untreated and advances, it can lead to acquired immunodeficiency syndrome or AIDS.
Unlike most other viruses, when a person contracts HIV, they have it for life because the human body cannot fight off the virus entirely. HIV, however, can be controlled and its progression can be slowed significantly. There are three stages of HIV:
Recommended Reading: Do Nba Youngboy Have Herpes
Hiv Prevalence Rate Ratios By Race/ethnicity 2019
The rate of Black males living with an HIV diagnosis is 5.6 times that of White males.
The rate of Hispanic/Latino males living with an HIV diagnosis is 2.9 times that of White males.
The rate of Black females living with an HIV diagnosis is 17.2 times that of White females.
The rate of Hispanic/Latina females living with an HIV diagnosis is 4.9 times that of White females.
Laboratory Technology For Hiv Incidence Surveillance
The assay currently used in STARHS is the BED HIV-1 Capture Enzyme Immunoassay , named for the branched peptide sequences for HIV-1 subtypes B, E, and D used in the assay. CDC developed the assay for the express purpose of estimating population-based HIV incidence, not for clinical or diagnostic purposes. Because its individual-level clinical and diagnostic usefulness has not been determined or approved by the Food and Drug Administration, it is at this time considered a tool for public health surveillance only. Therefore, CDC and its surveillance partners are prohibited from providing individual test results to patients or their health-care providers. CDC has recommended to state and local surveillance programs that health-care and partner counseling and referral providers use other readily available epidemiologic, laboratory, and clinical information to choose the best course of action for treatment and partner notification.
You May Like: How Long Before Hiv Turns Into Aids
People Who Inject Drugs
It is now widely accepted that the USA is experiencing a nationwide public health emergency in the form of an opioid epidemic.3940
Heroin use is increasing in the USA among men and women in most age groups and across all income levels, rising by 63% between 2002 and 2013 alone. A study published in 2019 estimated that more than 750,000 people in the USA inject drugs and that this number is rising.41
A huge contributing factor to this is misuse of prescription opioids, which has seen an increasing number of people turn to injecting drug use, particularly in non-urban areas where previously, injecting drugs had not been a significant issue. This has created new HIV prevention challenges as it has placed more people at risk of HIV.
Between 2010 and 2016, new infections among people who inject drugs fell by 30% overall.42 However, there are concerns that the level of new infections may have stagnated or reversed in recent years due to increased levels of injecting.4344
Evidence is emerging of increases in hepatitis C infections and new, localised outbreaks of HIV.45 For instance, Scott County in Indiana, with a population of only 23,744, experienced 181 new HIV infections in 2015.46
The impacts of the opioid epidemic are far reaching: the US has experienced the fastest proportional rise of drug-related overdose deaths ever recorded, which rose by 21.4% between 2015-2016 alone.47
Risk Factors Contributing To The Black Hiv Rate
| This section possibly contains original research. Please improve it by verifying the claims made and adding inline citations. Statements consisting only of original research should be removed. |
Access to healthcare is very important in preventing and treating HIV/AIDS. It can be affected by health insurance which is available to people through private insurers, Medicare and Medicaid which leaves some people still vulnerable. Historically, African-Americans have faced discrimination when it comes to receiving healthcare.
Homosexuality is viewed negatively in the African-American Community. “In a qualitative study of 745 racially and ethnic diverse undergraduates attending a large Midwestern university, Calzo and Ward determined that parents of African-American participants discussed homosexuality more frequently than the parents of other respondents. In analyses of the values communicated, Calzo and Ward reported that Black parents offered greater indication that homosexuality is perverse and unnatural”.
Recommended Reading: Hiv Hair Loss Symptom
Hiv And Aids In The United States Of America
KEY POINTS
- More than one million people are living with HIV in the United States of America one in seven are unaware of their status.
- The HIV epidemic is driven by sexual contact and is concentrated among certain key populations, in particular gay men and other men who have sex with men.
- African Americans are worse affected by HIV across all key population groups.
- Despite condoms being widely available, use is falling, even among people who are at heightened risk of acquiring HIV.
- The USA is experiencing a public health emergency in the form of an opioid epidemic which is threatening the gains made on reducing HIV among people who use drugs.
- Stigma remains a huge barrier to preventing HIV, and is linked to low testing rates, as well as poor adherence to treatment, particularly among young people.
Explore this page to find out more about the , ,, and the.
Around 1.1 million people are living with HIV in the United States of America . Nearly one in seven of these people are unaware they have HIV.1 The size of the epidemic is relatively small compared to the overall population but is heavily concentrated among several . In 2017, 66% of annual new HIV infections occurred among gay men and other men who have sex with men 2 among whom African American/black men are most affected, followed by Latino/Hispanic men. Heterosexual African American/black women, young people and transgender women of all ethnicities are also disproportionately affected.
Tuberculosis Among People Living With Hiv
Tuberculosis is the leading HIV-associated opportunistic infection in low- and middle- income countries, and it is a leading cause of death globally among people living with HIV. Death due to tuberculosis still remains high among people living with HIV, however the number of deaths is decreasing. Most of the global mortality due to TB among those with HIV is from cases in Sub-Saharan Africa.
In the charts here we see the number of tuberculosis patients who tested positive for HIV the number receiving antiretroviral therapy and the number of TB-related deaths among those living with HIV.
People who use ART are living longer
ART not only saves lives but also gives a chance for people living with HIV/AIDS to live long lives. Without ART very few infected people survive beyond ten years.3
Today, a person living in a high-income country who started ART in their twenties can expect to live for another 46 years that is well into their 60s.4
While the life expectancy of people living with HIV/AIDS in high-income countries has still not reached the life expectancy of the general population, we are getting closer to this goal.5
ART prevents new HIV infections
There is considerable evidence to show that people who use ART are less likely to transmit HIV to another person.7 ART reduces the number of viral particles present in an HIV-positive individual and therefore, the likelihood of passing the virus to another person decreases.
We need to increase ART coverage
You May Like: Hiv Gestation Period
Why Is Monitoring Progress Important
Canada has endorsed the Joint United Nations Programme on HIV/AIDS and the World Health Organization global health sector strategy on HIV that includes global targets to generate momentum towards the elimination of AIDS as a public health threat by 2030.Footnote 1 The 90-90-90 targets state that by 2020, 90% of all people living with HIV know their status, 90% of those diagnosed receive antiretroviral treatment, and 90% of those on treatment achieve viral suppression. When these three targets have been achieved, at least 73% of all people living with HIV will be virally suppressed. UNAIDS modelling suggests that achieving these targets by 2020 will enable the world to eliminate the AIDS epidemic by 2030.Footnote 1
The continuum of HIV care is a useful framework for assessing progress against the 90-90-90 targets. The sequential nature of the stages in the continuum can point to where efforts need to be focussed and which areas require improvement. Estimating HIV prevalence is the first step in the continuum of care, and is critical for guiding the planning and investment for treatment, care and ongoing support for people living with and affected by HIV and AIDS. In addition, understanding HIV incidence is fundamental for understanding temporal changes in transmission patterns, and is useful for public health decision makers to monitor, strengthen and evaluate the impact of multi-sectoral public health actions.