Differences Between Human And Chimpanzee Hiv Infection
- Humans become immunodeficient and do not maintain normal levels of critical immune factors, CD4 and T lymphocytes. Chronically infected chimpanzees maintain normal levels and do not become immunodeficient.
- In contrast to humans, HIV does not reproduce well in chimpanzees.
- Humans develop opportunistic infections and cancers associated with HIV chimpanzees do not.
- Humans drop their antibody count prior to systemic illness chimpanzees do not.
Because of these significant disparities, HIV studies with chimpanzees have failed to produce a vaccine, treatment, or cure for AIDS. In fact, all vaccines that have proven safe and efficacious in chimpanzees have failed in humans, with one in 2007 actually increasing a humans chance of HIV infection. Admittedly, the HIV virus is very difficult to study, but using the wrong toolthe chimpanzeehas not helped scientists in their pursuits.
Hiv Is The Same As Aids
HIV is an acronym for human immunodeficiency virus, which is the virus that causes AIDS . Contracting HIV can lead to the development of AIDS or stage 3 HIV, which causes serious damage to the immune system. While this virus is the underlying cause of AIDS, not all HIV-positive individuals have AIDS, as HIV can remain in a latent state for many years. If undiagnosed or left untreated, HIV usually progresses to AIDS, defined as possessing a CD4+ lymphocyte count under 200 cells/l or HIV infection plus co-infection with an AIDS-defining opportunistic infection. HIV cannot be cured, but it can be treated, and its transmission can be halted. Treating HIV can prevent new infections, which is the key to ultimately defeating AIDS.
Highly Active Anti-Retroviral Therapy in many cases allows the stabilization of the patient’s symptoms, partial recovery of CD4+ T-cell levels, and reduction in viremia to low or near-undetectable levels. Disease-specific drugs can also alleviate symptoms of AIDS and even cure specific AIDS-defining conditions in some cases. Medical treatment can reduce HIV infection in many cases to a survivable chronic condition. However, these advances do not constitute a cure, since current treatment regimens cannot eradicate latent HIV from the body.
Did Hiv Come From Monkeys
In 1999, researchers found a strain of SIV in a chimpanzee that was almost identical to HIV in humans.
The researchers who discovered this connection concluded that it proved chimpanzees were the source of HIV-1, and that the virus had at some point crossed species from chimps to humans.3
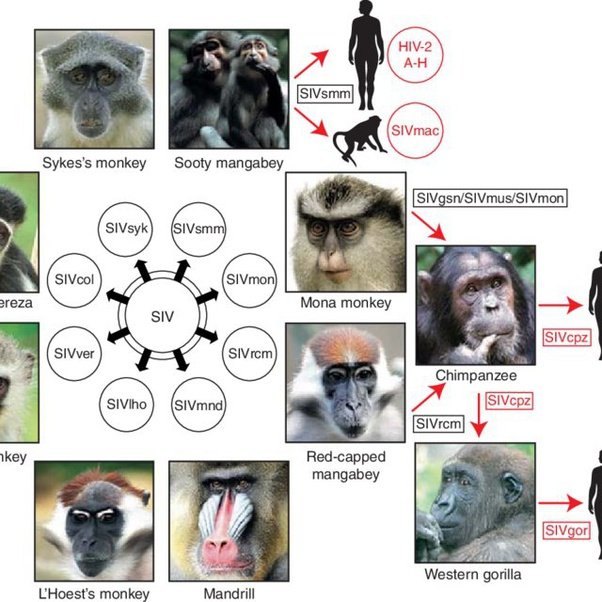
The same scientists then conducted more research into how SIV could have developed in the chimps. They discovered that the chimps had hunted and eaten two smaller species of monkeys . These smaller monkeys infected the chimps with two different strains of SIV.
The two different SIV strains then joined together to form a third virus that could be passed on to other chimps. This is the strain that can also infect humans.4
Recommended Reading: What Treatment Is Used For Hiv
Genetic Sequencing Confirms Geographical Origin
In order to determine this, the scientists compared the genetic diversity of viruses found in the Congo Basin, including the DRC and Cameroon. What they were able to determine was that, using the genetic clues and historical data, the outbreak did not start in Cameroon as previously thought, but was a result of the spread of the virus between Kinshasa and Cameroon as a result of river trade.
The investigators ultimately confirmed that the virus found in Kinshasa exhibited more HIV-1 genetic diversity than anywhere elseresulting from the spread of the rapidly mutating virus from person to personas well as the oldest known HIV-1 genetic sequences.
From the 1920s to the 1950s, rapid urbanization and the development of railways made Kinshasa a transport capital, thereby allowing the spread of HIV-1 throughout the country and soon after to East and Southern Africa. The genetic footprint left during this period illustrated dissemination of the virus throughout the DRC as people traveled on railways and along waterways to the cities of Mbuji-Mayi and Lubumbashi in the south and Kisangani in the north.
Between the 1950s and 1960s, the use of unsterilized hypodermic needles in sexually transmissible diseases clinics and the growth of commercial sex trade were among the factors for the rapid spread of the viruses, particularly in mining communities where there was a high migratory workforce.
Natural History Of Sivcpz Infection
Initially, SIVcpz was thought to be harmless for its natural host. This was because none of the few captive apes that were naturally SIVcpz infected suffered from overt immunodeficiency, although in retrospect this conclusion was based on the immunological and virological analyses of only a single naturally infected chimpanzee . In addition, SIV-infected sooty mangabeys and African green monkeys showed no sign of disease despite high viral loads in blood and lymphatic tissues , leading to the belief that all naturally occurring SIV infections are nonpathogenic. However, the sporadic prevalence of SIVcpz, along with its more recent monkey origin, suggested that its natural history might differ from that of other primate lentiviruses. To address this, a prospective study was initiated in Gombe National Park, Tanzania, the only field site where SIVcpz infected chimpanzees are habituated and so can be observed in their natural habitat.
Recommended Reading: What Is Hiv 1 And 2 Antibody Test
Hiv Cannot Be The Cause Of Aids Because The Body Develops A Vigorous Antibody Response To The Virus
This reasoning ignores numerous examples of viruses other than HIV that can be pathogenic after evidence of immunity appears. Measles virus may persist for years in brain cells, eventually causing a chronic neurologic disease despite the presence of antibodies. Viruses such as Cytomegalovirus, Herpes simplex virus, and Varicella zoster may be activated after years of latency even in the presence of abundant antibodies. In other animals, viral relatives of HIV with long and variable latency periods, such as visna virus in sheep, cause central nervous system damage even after the production of antibodies.
HIV has a well-recognized capacity to mutate to evade the ongoing immune response of the host.
When Did Hiv Enter The Population
By looking at the genome sequences of different viruses over time, researchers can calibrate a molecular clock based on the rate of sequence change, or mutations. Scientists can then use this to infer the rate of evolution and thus determine approximately when the most recent common ancestor existed.
Using this technique, researchers estimated that HIV-1 group M originated in 1908 and group O in 1920. HIV-2 groups A and B originated a bit later approximately in 1940 and 1945, respectively.
Read Also: How Do Anti Hiv Drugs Work
Debunked: The Polio Vaccine And Hiv Link
Hilary Koprowski, MDThe Historical Medical Library of The College of Physicians of Philadelphia
When the Human Immunodeficiency Virus was discovered in the 1980s, people immediately wondered where it had come from and how it had found its way into humans. One conjecture that arose in the 1990s put the blame for HIV on a public health measure: a polio vaccine.
In the late 1950s, several different groups of researchers were developing vaccines against polio, which at the time was still epidemic worldwide. One of these vaccines, developed by Hilary Koprowski, MD , was used in trials in Africa, after first being tested in the United States. The vaccine virus was grown in tissue cultures taken from macaque monkeys before being administered to about a million people in Burundi, Rwanda, and what is now the Democratic Republic of the Congo.
In 1992, Rolling Stone magazine published a story that discussed Koprowskis oral polio vaccine as a possible source of HIV and, in turn, the AIDS epidemic. Koprowski sued Rolling Stone and the writer of the article, and the magazine issued a clarification statement in December 1993, saying
Although Hoopers claims were widely publicized, evidence does not support the idea of a link between OPV and HIV.
A Sharp Decline In Hiv/aids Chimpanzee Research
When Jeroms infected blood failed to induce any significant illness in the other three chimpanzees, it served as a wake-up call to researchers using chimpanzees for HIV research. A drop in the number of HIV protocols with chimpanzees followed.
This line of research decreased dramatically from where it was at its peak of roughly 30 studies per year in 1998 to just four in 2005 and three in 2006-2007.
You May Like: What Is The Hiv Rate In Atlanta
Hivs Unusual Family Tree
When epidemiologists talk about HIV, the numbers are staggering. An estimated 34 million people around the world were living with HIV in 2011, according to a report from the United Nations.
But evolutionary biologists are concerned with smaller figures.
Two: the number of HIV precursor strains that merged their genetic material inside a chimpanzee to create a much more virulent bug, deadly to chimps â and which ultimately spawned HIV.
One: the unfortunate chimp first infected with that new virus, known as simian immunodeficiency virus cpz, or SIVcpz.
Four: the number of times HIV jumped from chimp to human. HIV likely arose from blood contact when humans handled bushmeat from SIV-infected apes.
In some ways itâs surprising that HIVâs chimp precursor hasnât cropped up more often, said Fred Hutchinson Cancer Research Center virologist Dr. Michael Emerman.
The birth of SIVcpz âwas a very unusual event, because it only happened one time that we know of in evolutionary history,â said Emerman, who studies the viral, chimp and human evolutionary steps that ultimately allowed HIV to come into the world. âAnd we know that there are lots of exposures, because chimpanzees eat a lot of monkeys and a lot of these monkeys have their own version of these SIVs.â
Case Definition For Epidemiological Surveillance
According to a study published in the Proceedings of the National Academy of Sciences in 2008, a team led by Robert Shafer at Stanford University School of Medicine has discovered that the gray mouse lemur has an endogenouslentivirus in its genetic makeup. This suggests that lentiviruses have existed for at least 14 million years, much longer than the currently known existence of HIV. In addition, the time frame falls in the period when Madagascar was still connected to what is now the African continent the said lemurs later developed immunity to the virus strain and survived an era when the lentivirus was widespread among other mammals. The study is being hailed as crucial, because it fills the blanks in the origin of the virus, as well as in its evolution, and may be important in the development of new antiviral drugs.
In 2010, researchers reported that SIV had infected monkeys in Bioko for at least 32,000 years. Previous to this time, it was thought that SIV infection in monkeys had happened over the past few hundred years. Scientists estimated that it would take a similar amount of time before humans adapted naturally to HIV infection in the way monkeys in Africa have adapted to SIV and not suffer any harm from the infection.
You May Like: Can You Get Hiv From Positive Undetectable
Fatal Errors: Ignoring Differences
The flawed chimpanzee model of HIV not only failed to produce any sort of vaccine or treatment for HIV/AIDS, but actually contributed toward the suffering and deaths of thousands of citizens in France.
According to Claude Reiss, a leading French scientist:
In the early ’80s, the observation that HIV does not affect the chimpanzee led experts to assume that the virus is harmless to humans too. They consequently advised health authorities to allow transfusion with contaminated blood samples, the very cause of the French blood scandal that claimed thousands of innocent victims.
In 1996, when the UK parliament attempted to assess the risk and containment of mad cow disease, Pierre Tambourin, then head of the life science department at the National Center for Scientific Research referred to the French blood crisis in his testimony:
What are the chances of developing a prion disease following ingestion of contaminated meat? Nobody knows, but we must not repeat the error we did in 1983-1985 with AIDS, when we referred to animal models to dramatically underestimate the risk to which humans are exposed.
Hiv ‘may Have An Ancient Origin’

The origins of HIV can be traced back millions rather than tens of thousands of years, research suggests.
HIV, which causes Aids, emerged in humans in the 20th Century, but scientists have long known that similar viruses in monkeys and apes have existed for much longer.
A genetic study shows HIV-like viruses arose in African monkeys and apes 5 million to 12 million years ago.
The research may one day lead to a better understanding of HIV and Aids.
HIV affects 34 million people worldwide.
The disease emerged during the 20th century after a HIV-like virus jumped from chimps to humans.
Scientists have long known that similar viruses, known as lentiviruses, are widespread in African primates.
Past genetic research has suggested these “cousins” of HIV arose tens of thousands of years ago, but some experts have suspected this is an underestimate.
Don’t Miss: What City Has The Highest Hiv Rate
Jumping Species: How Hiv Entered Our World
Have you ever wondered what mysteries primate poop could unlock? No? Me neither. But luckily, Dr. Beatrice Hahn did. Dr. Hahn was deeply curious about the origin and evolution of HIV so, naturally, her path lead to poop.
Dont see the connection? Well, during Dr. Hahns recent visit to The Rockefeller University, she walked us down the poop path toward some astounding conclusions.
Why monkeys?
When HIV was identified in 1983, researchers almost immediately suspected that the virus came from non-human primates. This suspicion was heightened when a team of researchers found AIDS , the fatal final stage of HIV, in a captive colony of macaque monkeys.
Over the last two decades, Dr. Hahns team has shown that HIV originated in a sub-species of chimpanzee. But how did they solve this mystery?
HIV in Humans
HIV is diagnosed in humans by looking for antibodies against the virus in the blood and saliva. When infectious agents like viruses or bacteria enter our body, our immune system generates antibodies that help destroy the invaders. Importantly, each of the thousands of antibodies we make generally recognizes one type of foreign substance. For instance, I got chicken pox when I was three, so if you searched in my blood, you would find antibodies against this virus. Conversely, I thought I had malaria on my 21st birthday, but a blood test revealed that my body was not producing antibodies against it- I was just really sick for some other reason.
SIV in monkeys
Jumping Barriers
Where Did Hiv Come From A Look At The Origins Of The Pandemic Of Our Time
A chimpanzees virus has killed 35 million humans.
That virus, commonly known as HIV, is the defining pandemic of our time. More than 35 million people have been killed by the virus to date. But the virus itself didnt get its start in humans.
HIV/AIDS is, like the vast majority of emerging viruses infecting people, zoonotic in nature. The AIDS crisis, as we generally think of it, began in the 1980s. First as a mysterious illness primarily infecting gay men in urban areas in the United States. But thats not really the beginning. Before the diseases first mention in 1982 in the New York Times, people had been dying of AIDS for at least a decade, though probably not much longer. In Africa, HIVthe virus that causes AIDShad jumped from chimpanzees to humans sometime early in the 20th century.
To date, the earliest known case of HIV-1 infection in human blood is from a sample taken in 1959 from a man whod died in Kinshasa in what was then the Belgian Congo.
Its this fact which keeps me awake at night. Imagine, for a moment, that the HIV virus in that 1959 sample had been studied and identified. If, in the 1950s, the scientific community realized the potential harm this new virus could unleash. What could we have done? What therapies could we have developed before it became one of the deadliest pandemics in human history? Would we have a cure by now?
That work takes several forms, including:
Recommended Reading: How Do You Get Hiv 2
Hiv Is Not The Cause Of Aids
There is broad scientific consensus that HIV is the cause of AIDS, but some individuals reject this consensus, including biologist Peter Duesberg, biochemist David Rasnick, journalist/activist Celia Farber, conservative writer Tom Bethell, and intelligent design advocate Phillip E. Johnson.
A great deal is known about the pathogenesis of HIV disease, even though important details remain to be elucidated. However, a complete understanding of the pathogenesis of a disease is not a prerequisite to knowing its cause. Most infectious agents have been associated with the disease they cause long before their pathogenic mechanisms have been discovered. Because research in pathogenesis is difficult when precise animal models are unavailable, the disease-causing mechanisms in many diseases, including tuberculosis and hepatitis B, are poorly understood, but the pathogens responsible are very well established.
AZT and other antiretroviral drugs, not HIV, cause AIDS
The vast majority of people with AIDS never received antiretroviral drugs, including those in developed countries prior to the licensure of AZT in 1987. Even today, very few individuals in developing countries have access to these medications.
Behavioral factors such as recreational drug use and multiple sexual partnersnot HIVaccount for AIDS
AIDS among transfusion recipients is due to underlying diseases that necessitated the transfusion, rather than to HIV