Your Hiv Treatment Plan Can Impact Coverage Options
Your HIV treatment history is a crucial component of the type of life insurance you qualify for.
Fortunately, many physicians now consider HIV a chronic condition, rather than a terminal illness as it was viewed decades ago.
Antiretroviral therapy has been a spectacular success. People are now asking if the end of AIDS is possible.
The End of AIDS: HIV Infection as a Chronic Disease, National Institutes of Health
Plan to answer some specific questions about your treatment during the application process .
While each carriers underwriting questions vary, consider the following as examples of what you should be prepared to answer.
Data Structure And Editing
The dataset included all ARV by pharmaceutical registration numbers distributed on a monthly basis, regardless of whether the use was for prevention or treatment of HIV. Additional relevant items were product name, substance name, drug class, Anatomical Therapeutic Chemical classification code which is unique for each ARV and thus will be used synonymously throughout the paper , patent status, pharmacy retail price and defined daily dose . DDD was determined as the daily per capita consumption for each antiretroviral substance grouped by ATC, based on manufacturer specifications and guidelines . The ATC codes considered are listed by substance class, antiretroviral substances and quarter/year of launch as a generic drug . For the sake of clarity, two items were excluded from the analysis: 1) ARV that were not available in tablet form and 2) the DDD of single TDF mainly used for the treatment of hepatitis B . The DDD of the booster substances ritonavir and cobicistat were quantified by counting the DDD of the necessary combined protease inhibitor, ATC class J05AE , and their recommended boosting doses .
Table 1 Anatomical Therapeutic Chemical classifications by substance class, antiretroviral substances and quarter/year of launch as a generic drug in Germany
Cost Of Hiv Treatment
The cost of HIV treatment is a complicated issue with an extremely wide range of costs due to varying factors such as the type of antiretroviral therapy and the country in which the treatment is administered. The first line therapy of HIV, or the initial antiretroviral drug regimen for an HIV-infected patient, is generally cheaper than subsequent second-line or third-line therapies. There is also a great variability of drug prices among low, middle, and high income countries. In general, low-income countries have the lowest cost of antiretroviral therapy, while middle- and high-income tend to have considerably higher costs. Certain prices of HIV drugs may be high and difficult to afford due to patent barriers on antiretroviral drugs and slow regulatory approval for drugs, which may lead to indirect consequences such as greater HIV drug resistance and an increased number of opportunistic infections. Government and activist movements have taken efforts to limit the price of HIV drugs.
In 2019 the government of India reported that it was supplying 2/3 of drugs for HIV treatment.
Don’t Miss: What Is Usually The First Sign Of Hiv In Man
Medication Payment Assistance In Ontario
The price of medications can lead to financial hardship. In most cases, assistance to cover prescription drug costs is available. The following information about drug cost assistance may be valuable. It can help offset expenses. It can help you afford the medications. It is important that you take HIV medications at regular times. You need to avoid missed doses.
Before you start drug treatment, make sure you have payment assistance. This will help prevent interruption of your drug therapy. Some of the ways to get assistance are complex. You might benefit from assistance from a professional with experience in this area. Your Social Worker, Physician, Nurse, or staff in many social service agencies including AIDS Service Organizations can often help you set this up. Note that you must usually pay a non-waived pharmacy dispensing fee for each drug.
For patients in Ontario, various sources cover HIV/AIDS drug costs. The first three systems are the most utilized. They are drug coverage mechanisms that many people know about. They are likely the ones you need to understand and pay attention to. The other systems are less common. It most cases involving these additional six systems, a professional involved in your care will know it is needed and will set it up with you.
Why Is Hiv Treatment Expensive
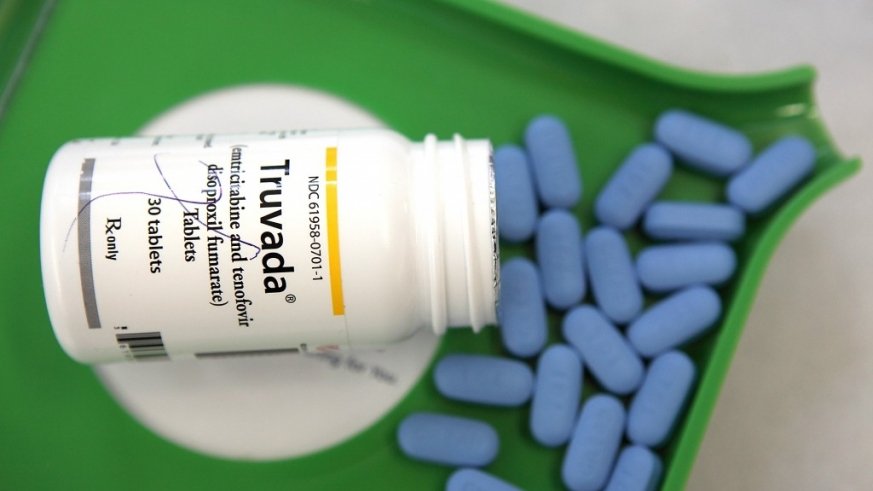
Certain HIV drugs may be prohibitively expensive and difficult to afford as a result of patent restrictions on antiretroviral drugs and the slow approval of new drugs by the Food and Drug Administration. This may have indirect consequences such as increased HIV drug resistance and an increase in the number of opportunistic infections.
Recommended Reading: Can You Get Hiv From Donating Blood
Discount Programs For Std Treatment
If you are not eligible for Medicare and do not have prescription drug coverage, you may qualify for patient assistance programs. Additionally, there are clinics and online programs to help you access treatment after a positive test result. Below are a few options to help you get the treatment you need.
Why Is Hiv Treatment So Expensive
Around two-thirds of the lifetime cost of managing HIV in the UK relates to the cost of antiretroviral drugs, with £429 million spent on anti-HIV drugs in 2015-2016. Prices of drugs vary depending on whether they are branded or generic, and the discounts that the NHS can negotiate with pharmaceutical companies.
Branded drugs are typically far more expensive than generic drugs because the pharmaceutical company that owns the drugs patent has a monopoly on its production. When a drugs patent expires, other companies are allowed to manufacture and sell the drug. If multiple companies are competing against each other, this drives prices down. Generic prices are usually around 80% lower than the prices paid for branded drugs.
Price discount agreements are often confidential, but an anonymised study found that they are generally 20-30% lower than the list price of a drug. However, list prices can vary dramatically from country to country, even for the same drug.
As a result of a global campaign in the 1990s to improve access to HIV treatment, low-income countries typically have licensing agreements with pharmaceutical companies which mean they can access HIV drugs at much lower prices. Pharmaceutical companies then charge higher prices to high-income countries to offset this discount.
comorbidity
The presence of one or more additional health conditions at the same time as a primary condition .
You May Like: Who To Contact To Remove Bee Hives
Cost Of Std Treatment
To get treated for an STD, you first need to get tested to determine the proper course of treatment. The cost of STD testing and treatment depends on the type of health insurance you have. If you have health insurance, you normally pay the copay charged by your provider.
If you do not have health insurance, STD testing and treatment can get pretty expensive. Testing alone can cost anywhere from $108-$600 without insurance. Then, there are different costs associated with each treatment, depending on if you have a bacterial or viral STD.
Where & How Do I Get Tested For Hiv
Under the Affordable Care Act, nobody can be denied health insurance due to a pre-existing condition. Most health insurance plans must cover certain recommended preventive services. This includes HIV testing for everyone between the ages 15 and 65 and for people of other ages at increased risk without additional cost-sharing, such as copays or deductibles.
Whether or not you have insurance, you can likely get an HIV test at the following locations:
- Local health clinic
- Primary care doctor
- Hospitals
If you don’t have insurance, you can become a Mira member and get an STD test for just $50- results are private and fast.
There are other options for HIV testing if you don’t have insurance.
- Health clinics or community health centers
- STD or sexual health clinics
- Your local health department
- Substance abuse prevention or treatment programs
You May Like: What Does The Acronym Hiv Stand For
Should I Get Tested For Hiv
âHIV can be detected by a blood antigen test in as little as 18 days after exposure. Thus, if one thinks that they are exposed to HIV, they should be tested within 30 days, but they may have to return to get tested again because it can take up to 45 days for HIV to be detectable after exposure. Testing every 3-6 months for people who are sexually active with multiple partners, and do not use protection, is sufficient unless they have direct knowledge of being exposed to HIV. A yearly test for people that are sexually active and use protection is recommended by the CDC. If one is in an exclusive, monogamous relationship with someone who is not HIV positive, then testing is likely unnecessary,â says Dr. Zrenchik.
The CDC recommends everyone between the ages of 13 and 64 get tested for HIV at least once. Some people at higher risk should get tested more often.
If your last HIV test result was negative, you should get an HIV test. If you answer “yes” to any of the questions below, you might be a person of higher risk for HIV:
Consequences Of High Antiretroviral Therapy Costs
Some consequences of high antiretroviral drug prices include greater occurrences of HIV resistance and an increase in the number of opportunistic infections. Patients may have financial difficulties obtaining access to expensive drugs, resulting in greater difficulties in adhering to recommended drug regimens for adequate viral suppression. For example, the lack of cheap and easily accessible generic pediatric DTG has contributed to inadequate nevirapine-based treatments in 40% of children who followed an HIV treatment regimen. With suboptimal adherence to treatment, there is an increased risk of HIV drug resistance in which the previously used treatment would no longer adequately suppress the HIV infection. The detection for HIV resistance can also be difficult and expensive as well, rendering lower-middle income countries unable to have access to various resistance tests and identifying resistant patients for treatment switches. HIV patients who have already developed resistance to first-line treatment are often barred from overcoming their resistance due to the difficulty in obtaining second- or third-line treatments, which can be several times more expensive than first-line treatment.
Don’t Miss: What To Do If I Have Hiv
How Much Does Std Treatment Cost Without Insurance In 2021
Sexually transmitted diseases and sexually transmitted infections will require treatment costing anywhere from $4 to $9,000 depending on your diagnosis without insurance. There are also initial costs of screening and doctorâs visit fees that may apply.
Routine STD screening is important to prevent future complications. A membership with Mira can help you access same-day STD testing for $99 instead of $521 out of pocket. Get peace of mind with affordable, convenient health care services today.
Paying For Pep For Another Reason
- If you cannot get insurance coverage, your health care provider can apply for free PEP medicines through the medication assistance programs run by the manufacturers.
- These requests for assistance can be handled urgently in many cases to avoid a delay in getting medicine.
Links with this icon indicate that you are leaving the CDC website.
- The Centers for Disease Control and Prevention cannot attest to the accuracy of a non-federal website.
- Linking to a non-federal website does not constitute an endorsement by CDC or any of its employees of the sponsors or the information and products presented on the website.
- You will be subject to the destination websites privacy policy when you follow the link.
- CDC is not responsible for Section 508 compliance on other federal or private website.
Also Check: Mode Of Transmission Of Hiv Aids
What Is Hiv & Aids
HIV stands for Human Immunodeficiency Virus. HIV is a virus that breaks down certain cells in your immune system . When HIV damages your immune system, itâs easier for you to get very sick and even die from infections that your body could normally fight off.
Once you have HIV, the virus always stays in your body. Thereâs no cure for HIV, but medicines can be used to stay healthy and reduce the risk of infections. Medications for HIV lowers or even completely diminishes the risk of spreading the virus to other people. Studies show that if HIV treatment is used as directed, it can lower the amount of HIV in a person’s blood so much that it might not even show up on a test â in this case, they canât transmit HIV through sex.
The Most Common Sexually Transmitted Diseases
It is crucial to get tested for STDs regularly â especially if you are sexually active. STDs do not always cause symptoms and may be dormant in your body, so it is possible to have an STD without knowing it. If this is the case, the STD may cause long-term damage to your body if left untreated.
Outlined below are some of the most common sexually transmitted infections in the United States:
- Bacterial Vaginosis
- Syphilis
- Trichomoniasis
Each of these STDs is passed differently. Some are carried in bodily fluids such as semen and blood, while others can be passed from skin-to-skin contact.
Therefore, one of the best ways to treat STIs is to prevent them in the first place. If you are having sex, using protective barriers, such as condoms and dental dams, are among the best safe sex practices to protect you from STD transmission.
Read Also: Does Hiv Change Sperm Color
Reasons For High Antiretroviral Therapy Prices
Excessive patent protection may also be attributed to evergreening, or methods to extend patents that are about to expire. Drug companies may extend patents well beyond their original expiration date by making slight modifications to their drug, preventing antiretroviral drugs from attaining reduced prices. For example, GSK added a secondary patent for abacavir with only minor changes and was able to effectively extend its patent of the drug by eight years in Ukraine. As such, the price of ABC in Ukraine has been as high as $277.40 per patient per year while other countries with the equivalent generic drug offered them at $123.42 per patient per year . The brand name drug Truvada, which provides the WHO recommended treatment of TDF/FTC, has also been able to extend its original patent expiry year of 2017 to 2026 through minor modifications to the drug.
The Issue And Why Its Important
In 2017, HIV/AIDS spending in Canada amounted to 686.8 million USD . This translates into USD 6,127.3 spending per prevalent HIV/AIDS case . Government spending as a share of total HIV/AIDS spending comprised 93.9% , whereas the shares of prepaid private spending and out-of-pocket spending were 1.2% and 4.9% , respectively . The proportion of HIV/AIDS spending on curative care and treatment was 63.6% and the proportion of spending on prevention was 15% .
The cost of HIV care for older patients has been consistently higher than for younger patients over the recent years and accounted for an increasing and disproportionately larger percentage of total HIV care costs . With the aging of people living with HIV, despite a stable HIV status and CD4 count equivalent to those of younger patients, older patients will continue to account for a disproportionately greater burden of care and costs in the future .
The aim of this review is to highlight out-of-pocket costs associated with HIV in jurisdictions with publicly funded health care systems.
Don’t Miss: Does Hiv Rash Go Away
Many Health Plans Now Must Cover Full Cost Of Expensive Hiv Prevention Drugs
Ted Howard started taking Truvada a few years ago because he wanted to protect himself against HIV, the virus that causes AIDS. But the daily pill was so pricey he was seriously thinking about giving it up.
Under his insurance plan, the former flight attendant and customer service instructor owed $500 in copayments every month for the drug and an additional $250 every three months for lab work and clinic visits.
Luckily for Howard, his doctor at Las Vegas Huntridge Family Clinic, which specializes in LGBTQ care, enrolled him in a clinical trial that covered his medication and other costs in full.
If I hadnt been able to get into the trial, I wouldnt have kept taking PrEP, said Howard, 68, using the shorthand term for preexposure prophylaxis. Taken daily, these drugs like Truvada are more than 90% effective at preventing infection with HIV.
Starting this month, most people with private insurance will no longer have to decide whether they can afford to protect themselves against HIV. Most health plans must begin to cover the drugs then without charging consumers anything out-of-pocket .
The task force recommended PrEP for people at high risk of HIV infection, including men who have sex with men and injection drug users.
Whether youre shopping for a new plan during open enrollment or want to check out what your current plan covers, here are answers to questions you may have about the new preventive coverage requirement.
Is Hiv Art Expensive
India has the cheapest antiretroviral therapy available, with first-line treatment costing the government Rs 5,000/person/year and second-line medication for patients who have developed resistance to the first-line meds costing the government Rs 29,000/person/year. Approximately 26,000 patients are receiving second-line therapy.
Don’t Miss: What Is In Prep Hiv
Experimental Hiv Drug Seems Effective At A Twice
An experimental new HIV treatment could, with just one dose, reduce the amount of virus in an infected person for up to six months. But experts arent convinced the advance will significantly change how we treat HIV anytime soon.
A group of researchers from Gilead Sciences developed a new drug dubbed lenacapavir, described Wednesday in Nature, that targets an HIV protein called capsid that has been nearly untargetable until now. Targeting capsid weakens the HIV virus outer coating, making it harder for the virus to infect our cells or protect itself from our bodys defenses. Current HIV treatments which most patients must take daily target proteins involved in the early stages of the virus life cycle, but targeting capsid affects multiple phases.
Experts are hesitant to use this drug alone in the clinic if it is approved. Patients are currently prescribed a combination of antiretrovirals that target different HIV proteins a way to prevent HIV from becoming resistant to the treatment. Gilead is still hoping it can develop other long-acting antiretrovirals that could be given to patients in combination with lenacapavir, according to Martin Rhee, the companys director of clinical research.
Right now, nearly everyone with HIV about 1.2 million people in the United States takes a combination antiretroviral pill every single day.
Experts say this issue must be addressed in the next phases of the clinical trial.