Impact Across The Country
- Although HIV has been reported in all 50 states, the District of Columbia, and U.S. dependencies, the impact of the epidemic is not uniformly distributed.
- Ten states accounted for about two-thirds of HIV diagnoses among adults and adolescents in 2019 .31 Regionally, the South accounted for more than half of HIV diagnoses in 2019.32
- Rates of HIV diagnoses per 100,000 provide a different measure of the epidemicâs impact, since they reflect the concentration of diagnoses after accounting for differences in population size across states. The District of Columbia has the highest rate in the nation, compared to states, nearly 3 times the national rate and Georgia was the state with highest rate , twice that of the national rate.33,34 Nine of the top 10 states by rate are in the South.35
- New HIV diagnoses are concentrated primarily in large U.S. metropolitan areas , with Miami, Orlando, and Atlanta topping the list of the areas most heavily burdened.36
| Table 1: Top Ten States/Areas by Number and Rate of New HIV Diagnoses , 2019 | |
| State | |
| U.S. Rate | 13.2 |
| CDC. HIV Surveillance Report, Diagnoses of HIV Infection in the United States and Dependent Areas, 2019 vol. 32. May 2021. |
Hiv And Aids In China
KEY POINTS
- China accounts for 3% of new HIV infections globally each year. In 2018, a 14% rise in new infections was reported, with 40,000 in the second quarter alone.
- The majority were transmitted through sex in the general population. In 2017, China steadily promoted comprehensive prevention programmes targeting female sex workers and men who have sex with men.
- The lack of comprehensive sexuality education is a major barrier to an effective response and open discussion of sex and sexual health is still taboo.
- Although significant progress has been made in tackling the HIV epidemic, HIV activists, non-governmental organisations and civil society are still being silenced.
Explore this page to read more about , , , , , , , and .
Chinas multi-sectoral approach to HIV, which engages government, civil society and the private sector and draws on comprehensive national data, can provide important lessons for many countries in Asia and the Pacific and beyond, particularly for south-south collaboration and sustainability.1
China has made substantial progress in tackling its HIV epidemic in the last decade but the national response to the HIV epidemic has been anything but steady, with negligence being a critical factor in the spread of HIV in the early 1990s. In recent years, a more committed national response has meant that the rate of new infections has slowed and that quality of life for some people living with HIV has improved.
Young Women And Adolescent Girls
HIV prevalence among young women is nearly four times greater than that of young men.14 In 2018, 540,000 young women were living with HIV, compared to 180,000 young men.15
In the same year, 69,000 young women became HIV-positive, compared to 28,000 young men, meaning they are over three times more likely to acquire HIV than their male counterparts. The difference is particularly acute among 10 to 19-year-olds, with 33,000 adolescent girls becoming HIV-positive in 2018, compared to 4,200 adolescent boys.16
Intergenerational relationships between older men, a group with high HIV prevalence, and young women are understood to be driving a cycle of infections. The National Strategic HIV Plan has centred its approach to HIV prevention around interrupting this cycle.1718
CASE STUDY: Sugar daddies
Lebogang Motsumi was 27 when she acquired HIV from a ‘sugar daddy’ a significantly older man who showered her with gifts, which she believed she needed to fit in with her friends and feel more accepting of herself. She was reluctant to use a condom in case she was perceived as promiscuous by men and felt she was not in control of the situation when she was with her sexual partners.
Now a mother, Motsumi says she wishes she had received more information at home and at school about risky sexual behaviour, and is using her experience to advocate non-judgemental, face-to-face conversations with young people about relationships with older men.19
Read Also: Can Syphilis Turn Into Hiv
Funding For Hiv In South Africa
South Africa largely funds its HIV programmes domestically, only receiving 12% of its HIV funding from external sources in 2018.126
South Africas National Strategic HIV, STI and TB Plan 2017-2022 is predicted to cost 207 billion rand in total. In light of this, in 2017 the South African government increased its budget allocation for HIV and AIDS, despite general budget reductions across the health sector.127
Still the South African National AIDS Council has predicted there will be some funding gaps. However, it is unclear how severe these will be, especially since there is a level of uncertainty around the availability of international funding for HIV and AIDS in the coming years.128
An encouraging sign came with the announcement from the US Presidents Emergency for AIDS Relief that it will be providing 10 billion rand in funding for 2019/2020, an increase from 2018 and 2017 funding levels.129
Treatment and care make up the biggest proportion of the costs, outlined in the NSP. In recent years South Africa has been working hard to negotiate better prices for ARVs, having previously been paying more than most other low- and middle-income countries despite having the worlds largest procurement programme.130 In September 2017 UNAIDS announced a breakthrough pricing agreement, which will allow the single pill regime of Dolutegravir to be sold at around $75 per person per year in south Africa and 90 other low- and middle-income countries.131
Access To Care & Treatment
- There are a number of sources of care and treatment for women with and at risk for HIV in the U.S., including government programs such as Medicaid, Medicare, and the Ryan White Program for those who are eligible.
- Looking across the spectrum of access to care, from HIV diagnosis to viral suppression, reveals missed opportunities for reaching women. Among women living with HIV in the U.S., 9 in 10 were aware of their HIV status however, many were tested late, many years after acquiring HIV, suggesting missed prevention opportunities. Moreover, only 65% have been linked to care and just 51% are retained in regular care and are virally suppressed.57
- In 2017, among women who are HIV positive, 22% were tested for HIV late in their illness that is, simultaneously diagnosed with HIV and AIDS a similar share as men .58
- Pre-exposure prophylaxis , a highly effective medication, prevents acquisition of HIV, but uptake has been slow among women in the U.S., suggesting potential barriers to the provision of PrEP for women. In 2016, women accounted for only 4.7% of PrEP users in the U.S.59
Also Check: How To Tell Someone Your Hiv Positive
Hiv And Tuberculosis Coinfection In China
China has some of the worlds highest burden for TB, multi-drug resistant TB and TB/HIV coinfection. In 2017, estimated TB-related deaths among people living with HIV stood at 1,800.85 China continues to follow the National Work Plan for the Implementation of the co-infection of Mycobacterium Tuberculosis and HIV and to screen people with HIV both people living with HIV and those newly diagnosed for TB. TB patients are also being tested for HIV in the 294 key counties for the prevention and control of HIV and TB coinfection.
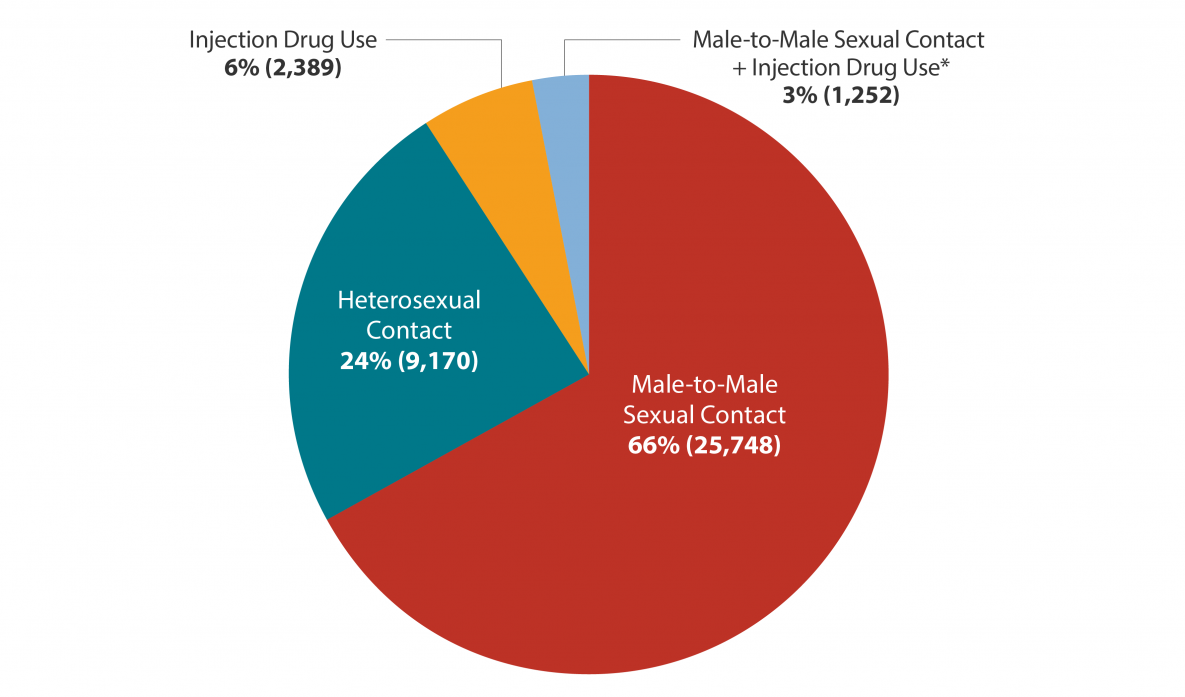
New Hiv Diagnoses In The Us And Dependent Areas By Transmission Category 2019
NOTE: Does not include other and perinatal transmission categories.
Source: CDC. Diagnoses of HIV infection in the United States and dependent areas, 2019. HIV Surveillance Report 2021 32.
If we look at HIV diagnoses by race and ethnicity, we see that Black/African American people are most affected by HIV. In 2019, Black/African American people accounted for 42% of all new HIV diagnoses. Additionally, Hispanic/Latino people are also strongly affected. They accounted for 29% of all new HIV diagnoses.
Recommended Reading: What Happens When You Stop Taking Hiv Meds
Under 1 Percent Of Us Adults Have Hiv: Report
By Maggie Fox, Health, Science Editor
3 Min Read
WASHINGTON – About one-half of one percent of young adults living in homes in the United States are infected with the AIDS virus, around 600,000 people, the National Center for Health Statistics reported on Tuesday.
The agencys snapshot of HIV infection in the United States shows the rate continues to be stable and confirms other surveys that show black men are far more likely than other Americans to be infected.
The report covers adults aged 18 to 49 and only people living in households — not prisoners, the homeless or patients in institutions, said Gerry McQuillan, who led the study.
The data comes from people taking part in the federal governments National Health and Nutrition Examination Survey, who volunteer to have their blood tested for everything from cholesterol to AIDS and herpes, as well as undergo full physical exams.
What we have done is taken data from our surveys in 1999 to 2006 because HIV has a very low prevalence. You have to combine all the years, Gerry McQuillan, who led the study, said in a telephone interview.
In 1999 to 2006, the prevalence of HIV infection among adults aged 18-49 years in the civilian noninstitutionalized household population of the United States was 0.47 percent, the report reads.
That works out to anywhere between 447,000 people and 841,000 people, with 618,000 the middle number, McQuillan said.
The report does not include data on how many people are newly infected with HIV.
Hiv Statistics By State
Human immunodeficiency virus, or HIV, is a virus that weakens a persons immune system by attacking cells that fight off infection, specifically a persons CD4 cells. HIV is spread through body fluids such as blood. If HIV goes untreated and advances, it can lead to acquired immunodeficiency syndrome or AIDS.
Unlike most other viruses, when a person contracts HIV, they have it for life because the human body cannot fight off the virus entirely. HIV, however, can be controlled and its progression can be slowed significantly. There are three stages of HIV:
Also Check: How Many Ppl Have Hiv
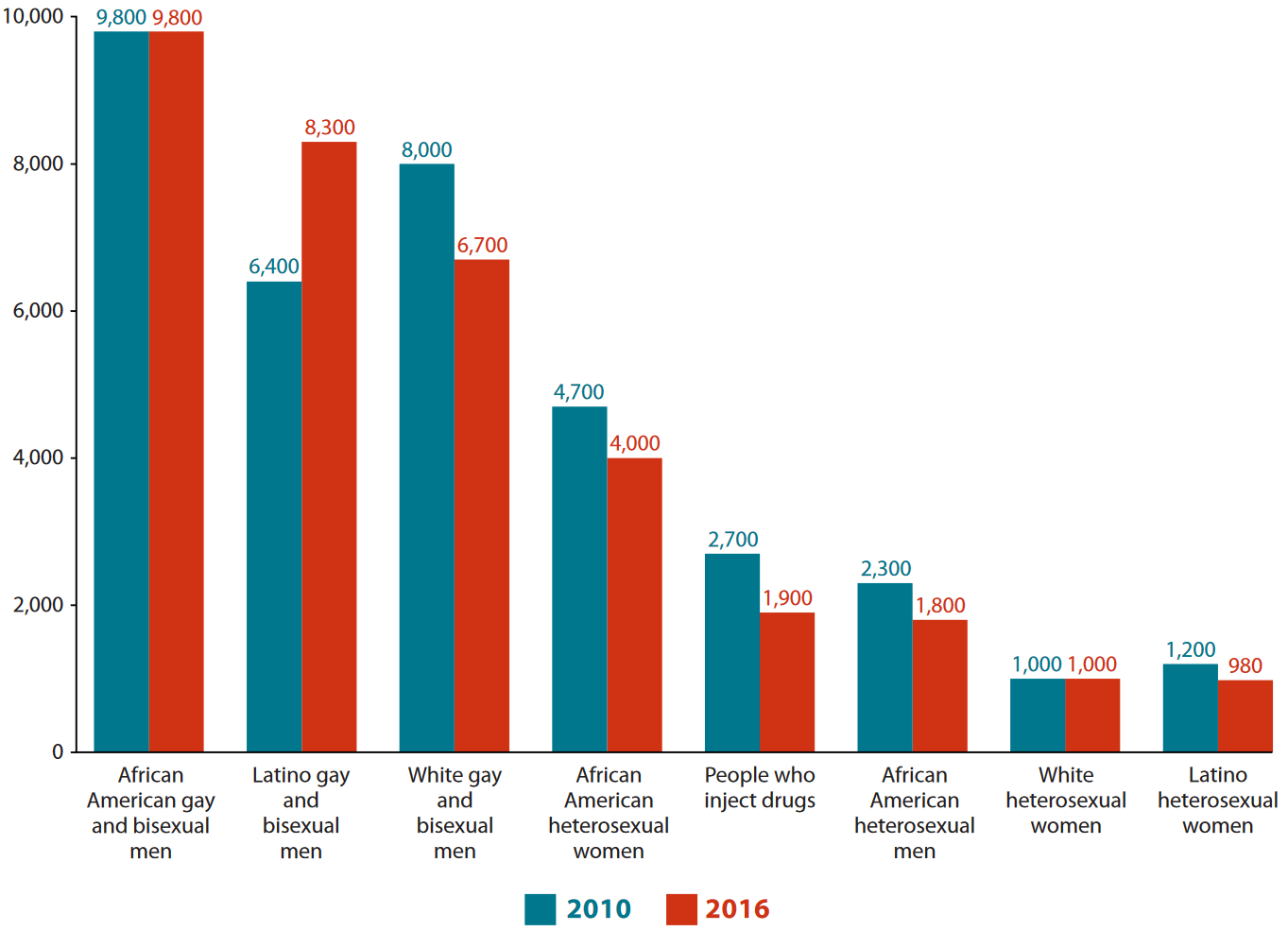
Men Who Have Sex With Men
Men who have sex with men are the group most affected by HIV in the USA, accounting for an estimated 2% of the population, but 66% of new annual HIV infections.13 At the end of 2015, the most recent data available, around 632,300 USA-based men who have sex with men were living with HIV. One in six of these people were unaware they were HIV positive.14
Between 2010 and 2016, new HIV infections among men who have sex with men remained stable at about 26,000 a year.15 However, trends vary greatly by age and ethnicity. For example, new infections among African American/black men who have sex with men remained stable overall, at about 10,000 new infections but they increased by 65% among those aged 25 to 34 . Among Latino and Hispanic men who have sex with men, new infections rose by around 30%, from 6,400 to 8,300. Again, the greatest rise was among 25 to 34-year-olds, where new infections increased by 68%. Among white men who have sex with men, new infections decreased to less than a-fifth overall, from 8,000 to 6,700.16
In 2016, it was estimated that, if current diagnosis rates continued, one in six American men who have sex with men would be diagnosed with HIV in their lifetime. This equates to one in two African American/black men who have sex with men, one in four Hispanic/Latino men who have sex with men and one in 11 white men who have sex with men.17
Hiv Testing And Counselling In China
China promotes HIV testing and scale up, and has made notable achievements in strengthening HIV counselling and testing in recent years. As well as more testing, a large number of new infections have been identified. Between 2008 and 2017, the number of HIV testing facilities increased from 7,600 to 30,500 the annual number of HIV tests increased from 45 million to 201 million , and due to more testing, the number of new infections reported increased from 56,350 to over 134,500.43
In 2017, a landmark study found that a patient-centred approach to streamlined HIV testing and treatment resulted in improved clinical outcomes for people living with HIV.
The approach aims to streamline pathways to HIV treatment, minimising the time and number of hospital or clinic visits between HIV testing and treatment initiation – a major reason why people do not remain in HIV care, and a major contributor to morbidity of people living with HIV in China.
Prior to streamlining, just 43% of patients who had received an initial positive result in some parts of the country were later given a confirmatory diagnosis. On top of this, just 57% of people newly diagnosed received a CD4 test within six months of diagnosis. In 2017, when national health guidelines still required a CD4 count to determine whether a person should start treatment, 80% of people newly identified as HIV-positive did not receive timely antiretroviral treatment.
Social media is encouraging gay Chinese men to get tested for HIV
Don’t Miss: How Long Do Hiv Results Take
How Can You Tell If You Have Hiv
The only way to know for sure if you have HIV is to get tested. You cant rely on symptoms to tell whether you have HIV.
Knowing your HIV status gives you powerful information so you can take steps to keep yourself and your partner healthy:
- If you test positive, you can take medicine to treat HIV. By taking HIV medicine daily as prescribed, you can make the amount of HIV in your blood very lowso low that a test cant detect it . Getting and keeping an undetectable viral load is the best thing you can do to stay healthy. If your viral load stays undetectable, you have effectively no risk of transmitting HIV to an HIV-negative partner through sex.
- If you test negative, there are more HIV prevention tools available today than ever before.
- If you are pregnant, you should be tested for HIV so that you can begin treatment if you’re HIV-positive. If an HIV-positive woman is treated for HIV early in her pregnancy, the risk of transmitting HIV to her baby can be very low.
Use the HIV Services Locator to find an HIV testing site near you.
HIV self-testing is also an option. Self-testing allows people to take an HIV test and find out their result in their own home or other private location. You can buy a self-test kit at a pharmacy or online, or your health care provider may be able to order one for you. Some health departments or community-based organizations also provide self-test kits for free.
New Hiv Diagnoses In The Us And Dependent Areas By Race/ethnicity 2019
*Black refers to people having origins in any of the black racial groups of Africa. African American is a term often used for people of African descent with ancestry in North America.Hispanic/Latino people can be of any race.
The most affected subpopulation is Black/African American gay and bisexual men.
Don’t Miss: How Many Hiv Positive In Usa
Funding Hiv Prevention For People Who Inject Drugs
Funding low-cost harm reduction initiatives such as NSPs and OST is a much more cost-effective way of tackling HIV among people who inject drugs than having to pay for antiretroviral treatment for the rest of a person’s life.44
Despite this, a deepening funding crisis is facing harm reduction services globally. The majority of countries that have a large HIV prevalence among their drug user population are middle-income countries. However, international HIV funding for these countries is shrinking as large donors such as the Global Fund shift their focus to low-income countries under the assumption that the funding gap for services will be filled by domestic resources. While there has been an increase in domestic investment in HIV programmes in some countries, very few are prioritising HIV prevention for key populations including harm reduction for people who inject drugs.45
Under-investment in HIV prevention for people who inject drugs is often not a question of lack of resources but of allocation. For example, an estimated US$100 billion is spent annually on global drug control. Reallocating as little as 2.5% of this money from drug enforcement to harm reduction programmes could reduce new HIV infections among people who inject drugs by 78%, alongside a 65% drop in HIV-related deaths. A shift of 7.5% of drug control funding would reduce new infections and HIV-related deaths by around 94%.46
– Harm Reduction International47
Hiv Prevention Programmes In China
HIV prevention programmes have consistently developed across the country in the last decade. Reducing sexual transmission of HIV has been the focus of Chinas prevention programming for some time since this is the main transmission route.46 In 2017, China steadily promoted comprehensive prevention programmes targeting key affected populations at greater risk of HIV including female sex workers and men who have sex with men.
We have limited resources to contain HIV. Shandong Province has over 100 counties, and each county has a population of over one million people. The least populous county still has 300,000 to half a million people. Yet each county has only one to three CDC staff dedicated to HIV prevention.
– Dr. Liao Meizhen, Shandong Center for Disease Control and Prevention , China
Recommended Reading: How Can Hiv Affect The Body
Civil Societys Role And Hiv In China
Restrictions on civil society in China make it very challenging for people to organise, occupy civil space and claim human rights in general, and even more so for members of key populations who are particularly vulnerable to HIV, or living with HIV.
In the face of an increasingly vocal public and more visible civil society activity in recent years, the government has further restrained peoples right to the freedoms of association, peaceful assembly and expression under the guise of protecting national security and preventing terrorism.
saw a marked increase in the use of detention, show trials and forced confessions, with human rights lawyers notably targeted. New punishments were introduced in late 2017 for such broad offences as disrespecting Chinas flag, national anthem and emblem. This fresh crackdown came as President Xi Jinping moved to consolidate his position at the helm of Chinas global power.
– Andrew Firmin, Editor-in-Chief, Civicus
Civil society organisations , activists and lawyers have been harassed, arbitrarily arrested and detained. Although protests are common in China, officially they are banned in most of the country and are particularly dangerous to hold in some regions, including Tibet, where they are regularly broken up and protestors are beaten. In the Xinjiang autonomous region in the north west, civic space is under extreme pressure: a counter-terrorism operation launched in 2014 has led to an almost total denial of free expression.