Does Having A Caesarean Reduce The Risk Of Passing On Hiv
Advances in treatment mean that a vaginal delivery shouldn’t increase the risk of passing HIV to your baby if both of the following apply:
- the HIV virus can’t be detected in your blood
- your HIV is well managed
In some cases, doctors may recommend a planned caesarean section before going into labour to reduce the risk of passing on HIV.
For example:
- if you’re not taking antiretroviral drugs
- if the HIV virus can be detected in your blood
Special Supplemental Nutrition Program For Women Infants And Children
Income-eligible women who qualify for WIC should be referred to their local WIC agency. WIC provides nutrition advice, nutritious foods for both mother and baby including formula, breastfeeding support and referrals to other services.
WIC provides lactation support by staff with expertise in breastfeeding education and lactation counseling. WIC staff conduct breast pump assessments to ensure that participants have the appropriate pump to meet their needs, and provide instructions in the use of a breast pump, and the care and storage of pumped breastmilk. WIC can also provide breast pumps to participating women.
Breastfeeding And Strategies To Reduce Risk Of Hiv Transmission
Both the evidence regarding the risk of HIV transmission via breastfeeding and the strategies to reduce this type of transmission come from studies conducted in low- and middle-income countries, where rates of infant mortality are high and many families do not have access to safe water and affordable formula. Without maternal ART and infant ARV prophylaxis, the risk of a breastfeeding infants acquiring HIV from a mother with HIV is 15% to 20% over 2 years.19,20
Studies have shown that maternal ART throughout pregnancy and breastfeeding as well as infant ARV prophylaxis during breastfeeding can reduce, but not eliminate, the risk of breast milkassociated HIV transmission.21-25 However, most of these studies provided ARV drugs to women or their infants only through 6 months postpartum and collected limited data on maternal plasma HIV viral load during breastfeeding.
You May Like: Does Nba Youngboy Still Have Herpes
Prevention Of Hiv Infection In Women Who Are Breastfeeding
Acquiring HIV while breastfeeding significantly increases the chance of mother-to-child HIV transmission due to the mothers viremia and increased infectivity during acute HIV infection. The NYS AIDS Institutes Perinatal HIV Prevention Committee recommends that a risk reduction plan should be in place for breastfeeding women who are at significant risk for HIV acquisition toreduce the incidence of acute infection and subsequent transmission to their infants. Risk factors include having a new diagnosis of a sexually-transmitted infection, a partner known to be infected with HIV, or using injection drugs. A discussion of HIV pre-exposure prophylaxis , which is a biomedical intervention using antiretroviral medications in non-HIV infected individuals to reduce their risk of acquiring HIV infection, should be included in the plan. Prevention of acute infection in a breastfeeding woman outweighs any theoretical concerns due to toxicity in the infant from TDF/FTC exposure during breastfeeding. Evidence to date suggests that the use of TDF is safe during breastfeeding and that PrEP drug exposure to infants through breastmilk is much lower than fetal antiretroviral drug exposures that occurs in utero in women who are on combination antiretroviral drug therapy.2
Ways Hiv Cannot Be Spread

HIV is not spread by:
- Air or water
- Mosquitoes, ticks or other insects
- Saliva, tears, or sweat that is not mixed with the blood of a person with HIV
- Shaking hands hugging sharing toilets sharing dishes, silverware, or drinking glasses or engaging in closed-mouth or social kissing with a person with HIV
- Drinking fountains
Also Check: Can You Get Aids From Dried Blood
What Choice Should I Make
You are the only person who should decide how your baby will be fed. If you choose to breastfeed, it is important to take your HIV drugs, and keep up with health care visits and viral load testing, exactly as prescribed and recommended by your provider. It is also very important to find a support network, including a providerand other allieswhom you trust, and who can be good sources for information without judgment.
Making this decision can be a challenging process. You may feel fear, stress, or even some sadness over any of the choices you are considering. It is also important to remember to take care of yourself during this process. It may be helpful to connect with a group of women or others who can offer support, to write about your thoughts and concerns, or to engage in some other activity that helps you feel supported as you prepare to make the best possible decision for you and your growing family.
Eliminating Hiv Transmission Through Breast Milk From Women Taking Antiretroviral Drugs
Don’t Miss: How Long Does It Take For Hiv
Does U=u Apply To Breastfeeding
No. Breast milk is different to blood and other bodily fluids. If you have an undetectable viral load, unfortunately there may still be a possibility of transmitting HIV to your baby. Breast milk contains high numbers of immune cells in which HIV can hide and not be picked up by routine viral load tests. Babies are exposed to large amounts of breast milk .
The current evidence we have is that although taking antiretroviral treatment drastically reduces the amount of HIV in breast milk, it may not remove it entirely. There have been a few documented cases of babies acquiring HIV from mothers with undetectable viral loads. PROMISE, an international study of 1200 breastfeeding mothers, found two cases of HIV transmission from mother to infant during breastfeeding when the mothers had an undetectable viral load. In two earlier studies of 560 breastfeeding women in Botswana, and 300 women in Malawi, a total of four cases were recorded. Nonetheless, the risk of passing on HIV via a single act of breastfeeding is so low as to be negligible.
Transmission Of Hiv From Mother To Child Through Breast Milk
Mother-to-child transmission of HIV is the primary way that children become infected with HIV. Such transmission can take place when the child is still in the mothers womb, around the time of birth, or through breastfeeding after birth. Hundreds of thousands of children are infected this way every year, with most of them in developing countries. Major progress has been made in preventing MTCT when the baby is still in the mothers womb, or around the time the baby is born. In many resource-rich settings, mothers with HIV infection are counseled not to breastfeed their children, and there are feasible and affordable alternatives to breastfeeding. However, in parts of the world where the vast majority of mothers with HIV infection live, complete avoidance of breastfeeding is often not feasible . Therefore, interventions to prevent transmission of HIV infection through breast milk are urgently needed. The authors found that, in addition to complete avoidance of breastfeeding if safe and affordable, exclusive breastfeeding for the first few months of life helps prevent transmission . Another intervention, giving the baby an anti-HIV medicine while breastfeeding, decreases the risk of transmission of HIV from mother to child. Implementation of such interventions, as well as developing more and better interventions, is essential.
Recommended Reading: Does Nba Youngboy Have Aids
How Do You Get Or Transmit Hiv
You can only get HIV by coming into direct contact with certain body fluids from a person with HIV who has a detectable viral load. These fluids are:
- Blood
- Semen and pre-seminal fluid
- Rectal fluids
- Vaginal fluids
- Breast milk
For transmission to occur, the HIV in these fluids must get into the bloodstream of an HIV-negative person through a mucous membrane open cuts or sores or by direct injection.
People with HIV who take HIV medicine daily as prescribed and get and keep an undetectable viral load have effectively no risk of sexually transmitting HIV to their HIV-negative partners.
Why Are Breastfeeding Guidelines Different
First of all, its important to note that not all HIV clinical guidelines for infant feeding are the same.
In high-income countries, women are advised not to breastfeed their infants because of the potential risk of HIV transmission. But in low-income countries, replacement feeding is often neither safe nor feasible, as mothers may not have access to clean water or formula feed. In these cases, the immunological benefits of exclusive breastfeeding far outweigh the risk of HIV transmission for the child in the context of malnutrition, diarrhoea, disease or pneumonia.
Also Check: Is Hiv In Semen
Can Hiv Be Transmitted Through Breastmilk
by yapmt_admin848 | Sep 23, 2019 | HIV/AIDS |
Many diseases and illnesses can be transmitted through the air, through sharing bodily fluids and through the water. One very big question is: Can HIV be transmitted through breast milk? Many new mothers who have been diagnosed with HIV would be keen on breastfeeding their babies. But is it safe to do so? Read more to find out the answer to Can HIV positive mothers breastfeed?
Isit safe?
Thetruthful answer is that it is not. There is a very great risk that thebreastmilk from a mother infected with HIV would carry the disease as well.Babies who drink this milk may also become infected with the virus because theydrink the milk.
Although the overall risk for the virus to be transferred to the infant is only 16%, it would be impossible for doctors to predict how much of the virus would be in the breastmilk that the child consumes. The mother would also have no means of controlling the number of viral loads can be in her breastmilk at any given time. This unpredictability is what makes it unsafe for mothers with HIV to breastfeed.
Whatis antiretroviral treatment?
This is a treatment that would prevent HIV from being passed on to the next generation. If a mother had already been diagnosed with HIV before getting pregnant, they would most likely be having treatment already.
Whatis a good substitute for breastmilk?
Donot let HIV define you
Breastfeeding And Herpes Simplex Virus
Herpes simplex virus is transmitted primarily through contact with an open sore or lesion. While HSV cannot be transmitted through breast milk, contact with sores on the nipples poses a serious risk to a newborn.
In such instances, mothers are advised bottle-feed their babies or use a breast pump so long as the equipment does not come into contact with a sore. Breastfeeding can be restarted once the sores are fully healed.
Read Also: Hiv Screen 4th Generation Wrfx Non Reactive
Is It Safe To Breastfeed With Hiv
Maybe. Recommendations around this issue are complex and differ depending on the organization you consult and your access to resources like clean water, formula, and healthcare.
If a person with HIV wishes to breastfeed, they should speak with their doctor for additional guidance about their personal safety and risks.
Transmission Of Hiv Via The Upper Gi Tract In Blt Mice
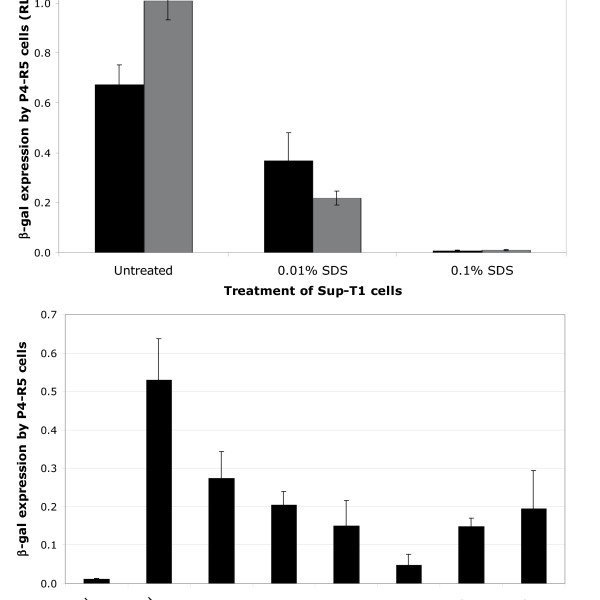
Following ingestion of breast milk from HIV-infected mothers, HIV transmission to neonates may occur in the oral cavity and/or upper GI tract. In BLT humanized mice, this could also be the case given the robust reconstitution of the oral cavity and upper GI tract with human dendritic cells, macrophages and CD4+ T cells. In order to determine if HIV transmission can occur distal to the esophagus, we introduced HIV-1JR-CSF directly into the stomach of BLT mice by oral gavage. After exposure by gavage, viral RNA could be readily detected in the plasma of all BLT mice two weeks post-exposure . This finding indicates that the mucosal surfaces of BLT mice distal to the oral cavity can be directly infected with HIV to effect transmission. These results serve as evidence for this mode of HIV transmission.
To determine if the upper GI tract of BLT mice is susceptible to HIV transmission, we evaluated HIV acquisition after a single direct administration of virus to the upper GI tract via gavage. Infection was monitored in peripheral blood by determining the levels of viral load in BLT mice receiving cell-free HIV-1JR-CSF directly into the stomach by gavage. The viral load for each mouse is indicated and the limit of detection for the assay is illustrated with a dashed line.
You May Like: Does Cookie Johnson Have Hiv
Also Check: How Long Can Aids Be Dormant
Hepatitis In The Mother
The diagnosis of hepatitis in a pregnant woman or nursing mother causes significant anxiety. The first issue is determining the etiology of the hepatitis, which then allows for an informed discussion of risk to the fetus/infant. The differential diagnosis of acute hepatitis includes common causes of hepatitis, such as hepatitis A, B, C, and D uncommon causes of hepatitis, such as hepatitis E and G, CMV, echoviruses, enteroviruses, EBV, HSV, rubella, varicella-zoster virus, yellow fever virus rare causes of hepatitis, such as Ebola virus, Junin virus, and Machupo virus , Lassa virus, and Marburg virus and nonviral causes, such as hepatotoxic drugs, alcoholic hepatitis, toxoplasmosis, autoimmune hepatitis, bile duct obstruction, ischemic liver damage, Wilson disease, 1-antitrypsin deficiency, and metastatic liver disease. The following sections focus on hepatitis viruses A to G. Other infectious agents that can cause hepatitis are considered individually in other sections. provides hepatitis terminology.
Safety Of Maternal And Infant Use Of Antiretroviral Drugs During Breastfeeding
A systematic data review showed a decrease in maternal bone mineral content among breastfeeding mothers who were receiving TDF-based ART compared to mothers who received no ART, but whether this condition persisted after discontinuation of breastfeeding was not known.40 The clinical significance of the reduced bone mineral density is uncertain. Subsequent studies in Africa have shown TDF-based ART to be associated with a decrease in bone mineral density during lactation. In one study, bone mineral density decline through 74 weeks postpartum was greater in breastfeeding women with HIV receiving TDF than in those receiving ZDV-based ART.41 A second study comparing bone mineral density in women with HIV receiving TDF-based ART to women without HIV showed accelerated loss during lactation, with only partial recovery by 3 months after cessation of lactation.42
Likewise, the rates of serious adverse events among infants who receive extended ARV prophylaxis during breastfeeding are low. In one study, the rate of adverse events in infants receiving 6 months of NVP was not significantly different from the rate in infants receiving placebo. A second study that compared two infant ARV prophylaxis regimens found no significant difference between the rates of adverse events among infants receiving the two regimens.22-24,27 Studies to date have examined only short-term adverse events, and few data are available on whether there might be long-term consequences of these drug exposures.
Recommended Reading: Hiv Causes Hair Loss
Is It Safe For A Mother Infected With Hiv To Breastfeed Her Infant
No. The best way to prevent transmission of HIV to an infant through breast milk is to not breastfeed. In the United States, where mothers have access to clean water and affordable replacement feeding , CDC and the American Academy of Pediatricsexternal icon recommend that HIV-infected mothers completely avoid breastfeeding their infants, regardless of ART and maternal viral load. Healthcare providers should be aware that some mothers with HIV may experience social or cultural pressure to breastfeed. These mothers may need ongoing feeding guidance and/or emotional support.
In resource-limited settings, such as some parts of Africa, the World Health Organization recommends that HIV-infected mothers breastfeed exclusively for the first 6 months of life and continue breastfeeding for at least 12 months, with the addition of complementary foods. These mothers should be given ART to reduce the risk of transmission through breastfeeding.
Hiv Breastfeeding And Being Undetectable
Scientists are hesitant to declare that there is no risk of HIV transmission during breastfeeding by mothers with an undetectable viral load, as they have done for sexual transmission. We talk through why its contentious.
Antiretroviral treatment keeps people living with HIV healthy but its also a powerful prevention tool. We now know that with effective HIV treatment, people living with HIV can suppress the virus to an undetectable level which makes the risk of sexual transmission of HIV equal to zero .
The U=U movement has unburdened thousands of people living with HIV with the knowledge that they cannot give HIV to their partners through sex if they are virally suppressed. But there has so far been no consensus on declaring U=U for breastfeeding. Why is that?
Also Check: Hiv Screen 4th Generation Wrfx Nonreactive
Getting Pregnant When Both Parents Have Hiv
Seroconcordant couples , can have an HIV-negative child. If both partners are on treatment, the risk of either partner transmitting HIV to their baby is almost zero.
If you are a seroconcordant couple and you are thinking of becoming pregnant it is important to speak with an obstetrician and an HIV specialist to minimise the risk of transmitting HIV to your baby.