Origin And Epidemic Emergence
Several of the theories of HIV origin accept the established knowledge of the HIV/SIV phylogenetic relationships, and also accept that bushmeat practice was the most likely cause of the initial transfer to humans. All of them propose that the simultaneous epidemic emergences of four HIV groups in the late 19th-early 20th century, and the lack of previous known emergences, are explained by new factor that appeared in the relevant African regions in that timeframe. These new factor would have acted either to increase human exposures to SIV, to help it to adapt to the human organism by mutation , or to cause an initial burst of transmissions crossing an epidemiological threshold, and therefore increasing the probability of continued spread.
Genetic studies of the virus suggested in 2008 that the most recent common ancestor of the HIV-1 M group dates back to the Belgian Congo city of Léopoldville , circa 1910. Proponents of this dating link the HIV epidemic with the emergence of colonialism and growth of large colonial African cities, leading to social changes, including a higher degree of non-monogamous sexual activity, the spread of prostitution, and the concomitant high frequency of genital ulcer diseases in nascent colonial cities.
Social changes and urbanization
Colonialism in Africa
This theory was later dubbed “Heart of Darkness” by Jim Moore, alluding to the book of the same title written by Joseph Conrad, the main focus of which is colonial abuses in equatorial Africa.
The Aids Epidemic Arises
Though HIV arrived in the United States around 1970, it didnt come to the publics attention until the early 1980s.
In 1981, the Centers for Disease Control and Prevention published a report about five previously healthy homosexual men becoming infected with Pneumocystis pneumonia, which is caused by the normally harmless fungus Pneumocystis jirovecii. This type of pneumonia, the CDC noted, almost never affects people with uncompromised immune systems.
The following year, The New York Times published an alarming article about the new immune system disorder, which, by that time, had affected 335 people, killing 136 of them. Because the disease appeared to affect mostly homosexual men, officials initially called it gay-related immune deficiency, or GRID.
Though the CDC discovered all major routes of the diseases transmissionas well as that female partners of AIDS-positive men could be infectedin 1983, the public considered AIDS a gay disease. It was even called the gay plague for many years after.
In September of 1982, the CDC used the term AIDS to describe the disease for the first time. By the end of the year, AIDS cases were also reported in a number of European countries.
People Who Inject Drugs
Injecting drug use has increased in South Africa over the last two decades. It is estimated that around 75,000 people in the country inject drugs.46
Data on HIV prevalence among people who inject drugs has been scarce but is improving. In 2018, results of a population-level survey suggest 21.8% of people who inject drugs are living with HIV.47
A 2016 study of people who inject drugs in five South African cities found 32% of men and 26% of women regularly shared syringes and other injecting equipment and nearly half reused needles.48
People who inject drugs are also associated with other high-risk behaviours such as sex work and unsafe sexual practices. For example, the same study reported fewer than half of those surveyed used a condom during their last sexual encounter.49
Read Also: Do Youngboy Have Herpes
Voluntary Medical Male Circumcision
In 2010, research emerged from sub-Saharan Africa suggesting that voluntary medical male circumcision can reduce the risk of female-to-male HIV transmission by up to 60%.89 This led the South African government to rapidly roll out a national VMMC programme, which aimed to reach 80% of HIV-negative men by 2016.
However, this target has been missed. In 2017 around 32% of adult men were estimated to have been medically circumcised. The highest proportion of circumcisions have been carried out on young men , with 43% undergoing VMMC.90
Despite being off-target, South Africa is continuing to increase the number of circumcisions. In 2018 more than 572,000 circumcisions were performed, compared to 485,500 in 2015.91 Across the country the VMMC programme has mostly been well received with 78% of women preferring their partner to be circumcised, according to the 2011 youth sex survey.92
Canadian Flight Attendant Theory
A Canadian airline steward named Gaëtan Dugas was referred to as “Case 057” and later “Patient O” with the alphabet letter “O” standing for “outside Southern California”, in an early AIDS study by Dr. William Darrow of the Centers for Disease Control. Because of this, many people had considered Dugas to be responsible for taking HIV to North America. However, HIV reached New York City around 1971 while Dugas did not start work at Air Canada until 1974. In Randy Shilts‘ 1987 book And the Band Played On , Dugas is referred to as AIDS’s Patient Zero instead of “Patient O”, but neither the book nor the movie states that he had been the first to bring the virus to North America. He was incorrectly called “Patient Zero” because at least 40 of the 248 people known to be infected by HIV in 1983 had had sex with him, or with a person who had sexual intercourse with Dugas.
Don’t Miss: Hiv Hair Loss Symptom
Hiv Statistics In South Africa
Estimates suggest that 7.7 million South Africans are living with HIV, representing about 14% of the population . Additional statistics are as follows.
- The HIV rate among adults is more than 20% .
- One in five people aged 15 to 49 years is believed to be infected with HIV.
- 45% of all deaths in the country can be attributed to HIV.
- 13% of South African blacks are infected with HIV versus 0.3% of South African whites.
- It is estimated that there are 600,000 orphaned children as a result of AIDS.
How Did Humans Get Hiv
HIV infection is caused by the Human Immunodeficiency Virus . You can get HIV from contact with infected blood, semen, or vaginal fluids. Most people get the virus by having unprotected sex with someone who has HIV. Another common way of getting the virus is by sharing drug needles with someone who is infected with HIV.
Recommended Reading: Does Nba Youngboy Have A Std
Case Definition For Epidemiological Surveillance
According to a study published in the Proceedings of the National Academy of Sciences in 2008, a team led by Robert Shafer at Stanford University School of Medicine has discovered that the gray mouse lemur has an endogenouslentivirus in its genetic makeup. This suggests that lentiviruses have existed for at least 14 million years, much longer than the currently known existence of HIV. In addition, the time frame falls in the period when Madagascar was still connected to what is now the African continent the said lemurs later developed immunity to the virus strain and survived an era when the lentivirus was widespread among other mammals. The study is being hailed as crucial, because it fills the blanks in the origin of the virus, as well as in its evolution, and may be important in the development of new antiviral drugs.
In 2010, researchers reported that SIV had infected monkeys in Bioko for at least 32,000 years. Previous to this time, it was thought that SIV infection in monkeys had happened over the past few hundred years. Scientists estimated that it would take a similar amount of time before humans adapted naturally to HIV infection in the way monkeys in Africa have adapted to SIV and not suffer any harm from the infection.
Genotyping Of Archived Cape Town Specimens
Briefly, nucleic acid was extracted with the use of the QIAamp DNA Blood Mini Kit according to the manufacturers proposed protocols. All DNA samples were stored at 4°C until further use. Two loci of the HIV-1 genome were targeted for genotyping: the gag p24 and a partial pol fragment, including the entire protease and a large segment of the reverse transcriptase coding region of the polymerase gene . The methodology and primers that were used for the amplification and sequencing of target genes from DNA or cDNA templates, were adopted from Swanson and co-workers for the gag p24 assay and from Plantier and co-workers for the pol assays. The sequencing primers for the pol assay were complemented with the use of Pol 1D and pol 3 . The gag and pol regions were chosen due to the fact that they had successfully been used in the past to infer evolutionary histories,,,,,,,,.
Newly sequenced isolates were checked for sequence quality and possible contamination with the use of the HIV-1 sequence quality control tool from the BioAfrica website.
Don’t Miss: Does Nba Youngboy Have An Std
History Of Hiv In South Africa
The HIV epidemic emerged in South African around 1982. However, as the country was in the midst of the dismantling of apartheid, the HIV problem was, for the most part, largely ignored. Silently, while political unrest dominated the media, HIV began to take hold, both in the gay community and the vulnerable black population.
By 2000, the South African Department of Health outlined a five-year HIV/AIDS plan but received little support from South African President Thabo Mbeki. After consulting a group of AIDS denialists headed by Dr. Peter Duesberg, Mbeki rejected conventional HIV science and instead blamed the growing AIDS epidemic on poverty, colonialism, and corporate greed.
Without government support, the five-year plan did not get off the ground as quickly as planned, with few showing up to receive from free antiretroviral medication. In the meantime, HIV among pregnant South African women soared from eight-tenths of 1% in 1990 to over 30% by 2000.
It was only with the removal of Mbeki from office in 2008 that the government took steps to rein in the catastrophe, ramping up efforts to become what is today the largest HIV drugs program in the world.
However, increasing pressure to expand outreach has been undermined by a deteriorating public health infrastructure and the weakening of the South African currency under President Jacob Zuma. To date, less than 30 of people with HIV are on therapy, while infection rates among young adults continue to rise, unheeded.
Unresolved Questions About Hiv Origins And Emergence
The discovery of the main HIV / SIV phylogenetic relationships permits explaining broad HIV biogeography: the early centres of the HIV-1 groups were in Central Africa, where the primate reservoirs of the related SIVcpz and SIVgor viruses exist similarly, the HIV-2 groups had their centres in West Africa, where sooty mangabeys, which harbour the related SIVsmm virus, exist. However, these relationships do not explain more detailed patterns of biogeography, such as why epidemic HIV-2 groups only evolved in the Ivory Coast, which is one of only six countries harbouring the sooty mangabey. It is also unclear why the SIVcpz endemic in the chimpanzee subspecies Pan troglodytes schweinfurthii did not spawn an epidemic HIV-1 strain to humans, while the Democratic Republic of Congo was the main centre of HIV-1 group M, a virus descended from SIVcpz strains of a subspecies that does not exist in this country. It is clear that the several HIV-1 and HIV-2 strains descend from SIVcpz, SIVgor, and SIVsmm viruses, and that bushmeat practice provides the most plausible cause of cross-species transfer to humans. However, some loose ends remain.
It is not yet explained why only four HIV groups spread considerably in human populations, despite bushmeat practices being widespread in Central and West Africa, and the resulting human SIV infections being common.
Also Check: How Long Does Hiv
Where Did Aids Come From
Scientists have traced the origin of HIV back to chimpanzees and simian immunodeficiency virus , an HIV-like virus that attacks the immune system of monkeys and apes.
In 1999, researchers identified a strain of chimpanzee SIV called SIVcpz, which was nearly identical to HIV. Chimps, the scientist later discovered, hunt and eat two smaller species of monkeysred-capped mangabeys and greater spot-nosed monkeysthat carry and infect the chimps with two strains of SIV. These two strains likely combined to form SIVcpz, which can spread between chimpanzees and humans.
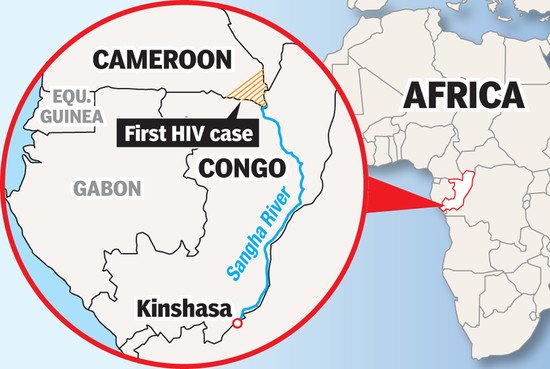
SIVcpz likely jumped to humans when hunters in Africa ate infected chimps, or the chimps infected blood got into the cuts or wounds of hunters. Researchers believe the first transmission of SIV to HIV in humans that then led to the global pandemic occurred in 1920 in Kinshasa, the capital and largest city in the Democratic Republic of Congo.
The virus spread may have spread from Kinshasa along infrastructure routes via migrants and the sex trade.
In the 1960s, HIV spread from Africa to Haiti and the Caribbean when Haitian professionals in the colonial Democratic Republic of Congo returned home. The virus then moved from the Caribbean to New York City around 1970 and then to San Francisco later in the decade.
International travel from the United States helped the virus spread across the rest of the globe.
READ MORE: Pandemics That Changed History: A Timeline
Did Hiv Come From Monkeys

In 1999, researchers found a strain of SIV in a chimpanzee that was almost identical to HIV in humans.
The researchers who discovered this connection concluded that it proved chimpanzees were the source of HIV-1, and that the virus had at some point crossed species from chimps to humans.3
The same scientists then conducted more research into how SIV could have developed in the chimps. They discovered that the chimps had hunted and eaten two smaller species of monkeys . These smaller monkeys infected the chimps with two different strains of SIV.
The two different SIV strains then joined together to form a third virus that could be passed on to other chimps. This is the strain that can also infect humans.4
Also Check: Is Hiv In Semen
Hiv Testing And Counselling In South Africa
South Africa has made impressive progress in recent years in getting more people to test for HIV. In 2017, South Africa reached the first of the 90-90-90 targets, with 90% of people living with HIV aware of their status, up from 85% in 2015.57
This progress follows the launch of two nationwide testing initiatives: the national HIV testing and counselling campaign in 2010 and the HTC revitalisation strategy in 2013, which focused on getting people from the private sector, farms and higher education to test.58 Thanks to campaigns such as these, more than 10 million people in South Africa test for HIV every year.59
Yet the progress made in getting people to test has been uneven. In South Africa women are much more likely to test than men. This is partly because PMTCT programmes enable women to access HIV testing services during routine antenatal appointments.60
In addition, recent research has shown that men often see health facilities as being womens places and so feel that testing for HIV is non-masculine. Men also report worrying that queuing outside a testing facility will be taken as evidence that they are living with HIV, and talk of avoiding testing because they are terrified of a positive result.61 As a result of the testing discrepancy between sexes, 93% of women living with HIV in 2018 were aware of their status compared to 88% of HIV-positive men.62
CASE STUDY: The impact of HIV testing within churches
The Status Of The Hiv/aids Epidemic In Sub
Senior Fellow, Futures Group International
Focus Area
Despite the fact that sub-Saharan Africa contains only about 11 percent of the Earths population, the region is the worlds epicenter of HIV/AIDS. The numbers are daunting. Adult HIV prevalence is 1.2 percent worldwide , but it is 9.0 percent in sub-Saharan Africa. UNAIDS estimates that at the end of 2001, there were 40 million people living with HIV/AIDS, 28.5 million of them from sub-Saharan African. Five million adults and children became newly infected with HIV in 2001, 3.5 million of them from sub-Saharan Africa. Three million people died from AIDS-related causes in 2001, and 2.2 million of these deaths were among sub-Saharan Africans.2
AIDS is now the leading cause of death in sub-Saharan Africa. Life expectancy at birth has plummeted in many African countries, wiping out the gains made since independence. The combination of high birth rates and high AIDS mortality among adults, including many parents, has meant that more than 90 percent of children who have been orphaned as a consequence of the HIV/AIDS epidemic are in this region.2
According to UNAIDS, all the worst affected countries are contiguous to one another in the lower part of the continent. These include South Africa, Lesotho, Swaziland, Botswana, Namibia, Zambia, and Zimbabwe. Botswana, Lesotho, Swaziland, and Zimbabwe have prevalence rates above 30 percent.4
| Total Adults and Children |
|---|
| 20.1 |
References
You May Like: How Long Does Aids Take To Show
Funding For Hiv In South Africa
South Africa largely funds its HIV programmes domestically, only receiving 12% of its HIV funding from external sources in 2018.126
South Africas National Strategic HIV, STI and TB Plan 2017-2022 is predicted to cost 207 billion rand in total. In light of this, in 2017 the South African government increased its budget allocation for HIV and AIDS, despite general budget reductions across the health sector.127
Still the South African National AIDS Council has predicted there will be some funding gaps. However, it is unclear how severe these will be, especially since there is a level of uncertainty around the availability of international funding for HIV and AIDS in the coming years.128
An encouraging sign came with the announcement from the US Presidents Emergency for AIDS Relief that it will be providing 10 billion rand in funding for 2019/2020, an increase from 2018 and 2017 funding levels.129
Treatment and care make up the biggest proportion of the costs, outlined in the NSP. In recent years South Africa has been working hard to negotiate better prices for ARVs, having previously been paying more than most other low- and middle-income countries despite having the worlds largest procurement programme.130 In September 2017 UNAIDS announced a breakthrough pricing agreement, which will allow the single pill regime of Dolutegravir to be sold at around $75 per person per year in south Africa and 90 other low- and middle-income countries.131